Cross-specialty collaboration to develop standard-of-care is still needed

Aspirin desensitization appears to be effective in improving pulmonary outcomes for patients with aspirin-exacerbated respiratory disease (AERD), according to a recent study appearing in Otolaryngology–Head and Neck. The meta-analysis examined results from 13 studies, which measured endoscopic polyp grading, changes in radiologic severity of chronic rhinosinusitis and sinus quality-of-life scores.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
AERD patients have a higher risk for nasal polyps, chronic sinusitis, asthma and aspirin sensitivity. Patients with this condition are also 10 times more likely to need sinus surgery than patients without the condition. Since aspirin desensitization’s initial discovery, several studies have found that aspirin desensitization can drastically improve quality of life, nasal polyp burden, and need for surgical intervention for this patient population.
“There are several protocols published mostly by asthma and allergists, and there is a low dose or high dose protocol,” according to Mohamad Chaaban, MD, an otolaryngologist in Cleveland Clinic’s Head & Neck Institute and one of the authors of the study. “In our study, we divided patients into two groups based on this protocol–those who take less than 650 mg of aspirin per day or those who take more than 650 mg.”
A total of 6055 articles were initially reviewed for eligibility, and 13 studies met the inclusion criteria. These 13 studies were published between 1984 and 2018 and consisted of five randomized controlled trials and eight cohort studies. The authors of the present study did not find any significant improvement in sinonasal quality of life or smell scores with aspirin desensitization. However, pooled analysis of the three studies that included medication/steroid use showed a statistically significant reduction in the use of medications (SMD = –0.792, P =< .001). For FEV-1 (forced expiratory volume in 1 second), there was a statistically significant improvement (SMD = 0.451, P = .031) among the studies that included this outcome measure.
“I didn’t expect positive results in the pulmonary perspective; I thought the positive effect would be limited to the improvement of sinonasal symptoms,” says Dr. Chaaban. “The good thing is that it really helps many patients and doctors who treat this condition, like allergists, sinus doctors, ENTs, pulmonologists, and some primary care doctors as well.”
In the included studies, aspirin dosage was highly variable, ranging from 100 mg to 1300 mg daily. The duration of follow-up was also highly variable, ranging from one month to 36 months. Dr. Chaaban believes these variances reinforce the importance of developing a set of standard protocols. “One of the main advantages of the study is that it opens up the need for physicians to find an ideal regimen or ideal protocol to treat those patients,” he says. “It may also lead to improved collaboration between pulmonologists and ENTs, and develop an algorithm for when patients actually need this treatment and a standard-of-care to follow.”

Expert advocates for a stepladder approach
Prompt surgery was necessary when symptoms drastically increased
Strong communication with the patient and a thorough approach are essential

Research on children with UHL explores the quality-of-life benefits and outcomes of cochlear implants

A look at how custom-fitted oral appliances work and when they’re a good fit for patients

With a wide scope of skills, comprehensive otolaryngologists care for patients of all ages in the community
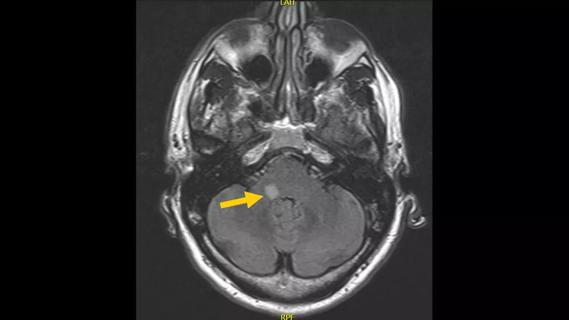
Subtle information gleaned from clinical examinations prompted concern
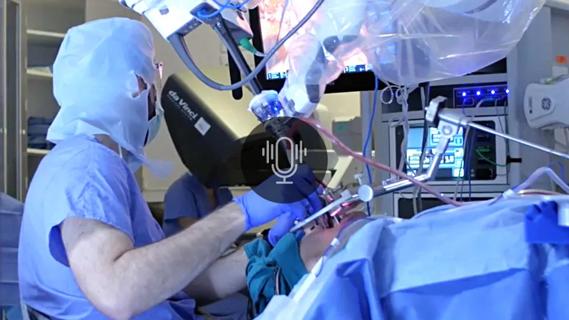
A new single-port system well-suited for oropharyngeal cancer treatment