Burgeoning benefits make dual certification a growing trend
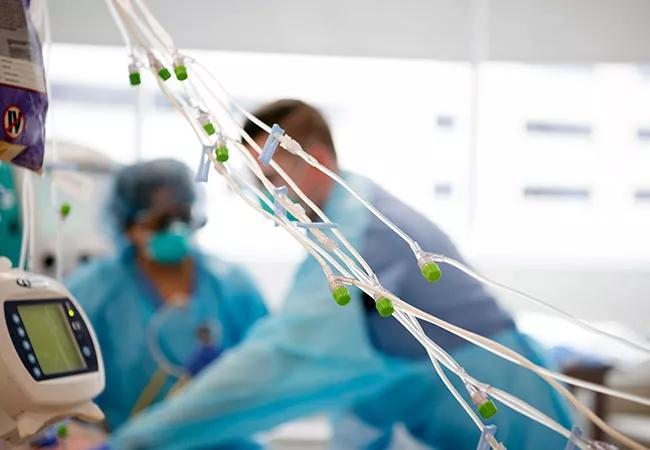
A visit to any contemporary cardiac intensive care unit (CICU) in recent years makes clear that the disciplines of advanced heart failure treatment and cardiac critical care are overlapping with increased frequency as these units fill with growing numbers of aging, vulnerable patients who have limited cardiac reserve and multiple comorbidities.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
This intersection of highly specialized needs is giving rise to a novel training pathway that combines advanced heart failure and transplant cardiology (AHFTC) with cardiac critical care and general cardiology to foster a distinctive and complementary skill set for a small subset of cardiology fellowship trainees. This pathway has been undertaken by a handful of trainees at Cleveland Clinic in recent years, and its merits were profiled in a recent perspective article in the Journal of Cardiac Failure (2021;27[10]:1152-1155) by Venu Menon, MD, Director of the Cardiac Intensive Care Unit and the Cardiovascular Fellowship Program at Cleveland Clinic, and Zachary IlˊGiovine, MD, a Cleveland Clinic fellow who is currently completing the training pathway.
“As the complexity and range of cardiac and noncardiac diagnoses in the cardiac critical care unit increase, there is a parallel need for an expansion of the ideal skill set to care for these patients,” says Dr. Menon. “We are finding that having staff with dual board certification in AHFTC and cardiac critical care is valuable to optimal operation of the CICU.”
Recent advances in cardiology have led to dramatic increases in longevity among patients with a range of cardiovascular conditions. The one downside of this progress is that it has created a larger population of vulnerable patients at increased risk of ultimately needing cardiac critical care for acute cardiac issues, often with significant involvement of one or more other organ systems. As a result, a focus simply on the heart may be inadequate for the ideal care of these patients.
This trend already prompted the emergence of cardiac critical care fellowship programs nearly a decade ago, with Dr. Menon establishing one of the nation’s first such dedicated programs at Cleveland Clinic. Yet as cardiac critical care has matured, the needs for specialized expertise have continued apace, with heart failure, cardiogenic shock and severe sepsis emerging as increasingly common diagnoses in CICUs.
“Because of this growing focus on heart failure and associated conditions as a predominant symptom in the CICU, it is natural to consider enhancing cardiac critical care training by supplementing it with dedicated subspecialty heart failure experience as well,” Dr. Menon explains.
That is precisely what Cleveland Clinic and several of its cardiovascular medicine fellows over the past few years have done. They have informally fashioned a three-part, five-year training program consisting of the following:
There is no clear preference for the sequence of the AHFTC and critical care training components, which has varied among the trainees who have undertaken the pathway to date.
While such extensive training makes sense primarily for cardiologists seeking to practice in tertiary or quaternary institutions, the benefits to such institutions and their patients are clear, especially in the context of the CICU. For example, having staff with both heart failure and critical care expertise promotes earlier recognition and better support for patients with impending or manifest cardiogenic shock. Additionally, CICU staff with subspecialty AHFTC expertise can facilitate decision-making around deployment of temporary mechanical circulatory support, including the nuances of exit strategies.
From his vantage point as director of a CICU that now has three staff physicians who have completed this training pathway, Dr. Menon says it has enhanced the quality of care delivery in the CICU. “This has been particularly true during the COVID-19 pandemic, where we have had many patients with diseases involving multiple organ systems,” he notes. “Having staff with significant expertise in both cardiac issues and care of patients on a ventilator, for example, has been a boon over the past two years.”
Beyond benefits to institutions, this novel training pathway offers multiple benefits to the trainees themselves, as outlined below.
Ability to practice in a variety of settings. Dual certification in AHFTC and cardiac critical care expands a cardiologist’s career and employment options and allows him or her to practice in a variety of settings while maintaining continuity of care. “This pathway allows for unique insights outside the traditional silos of medicine,” says Dr. IlˊGiovine, the current fellow who co-authored the perspective article with Dr. Menon. “A dual-trained cardiologist can serve as a bridge between disciplines and add increased support for some of our most vulnerable patients.”
Longitudinal relationships with patients. “A main reason I sought this pathway was to be able to walk with patients on their journey from acute illness to an eventual destination,” says Ran Lee, MD, who joined Cleveland Clinic as a staff cardiologist in 2020 after completing fellowships in both AHFTC and cardiac critical care. “I have a distinct interest in caring for patients in cardiogenic shock. My dual training allows me to be part of decisions from the critical illness perspective as well as decisions involving long-term heart failure care, whether it be recovery, mechanical circulatory support or transplant.”
The rewards of care continuity are echoed by Andrew Higgins, MD, who joined the staff in 2021 after completing successive fellowships at Cleveland Clinic in general cardiology, cardiac critical care and AHFTC. “Although I am early in my career here, I’ve already had several patients with heart failure whom I’ve cared for initially in the outpatient setting, then in the cardiac ICU, then on the nursing floor and then again in the outpatient clinic for follow-up,” he says. “There are others who I met in the cardiac ICU, helped through stabilization and recovery, and now follow in clinic for long-term recovery. The chance to see the downstream effects of your care beyond the ICU is gratifying.”
Professional fulfillment. Such gratification is linked to another benefit of this training pathway — the satisfaction that comes from simply being able to care for vulnerable patients more fully. “During my general cardiology fellowship, I realized I needed to expand my skill set to provide optimal, holistic care to the sickest of the sick patients I encountered in the ICU,” says Dr. IlˊGiovine. “My dual subspecialty training affords the opportunity to take care of these patients before, during and after their most critical moments.”
There’s consensus among Cleveland Clinic cardiologists and trainees that this novel training pathway will continue to grow in popularity as CICU patients’ needs become more complex.
“Upcoming residents and fellows often inquire about the pathway I chose and seek advice on how to navigate their futures,” says Dr. Lee.
“Trainees are eager to fill this need,” Dr. IlˊGiovine concurs. “Social media has been key in increasing awareness of and interest in combined training in critical care and advanced heart failure.”
“Many centers are trying to find the best combination of training for CICU management,” Dr. Higgins concludes. “The skill set of a cardiac critical care/advanced heart failure trainee would benefit almost any hospital system.”

Over 50 Cleveland Clinic faculty cover what’s new and notable in all major subspecialties

26th annual offering will mix the tried and true with emerging developments

Popular case-based course takes a multidisciplinary approach to wide range of care issues

Popular CME course takes a soup-to-nuts approach with a diverse faculty and inventive programming

Two-day CME designed for general cardiologists and primary care clinicians

Evidence-based updates on management advances and overcoming barriers to care

CME favorite in New York to cover care of tricuspid valve disease too

Over 40 global experts will convene for 4th annual crowd-pleasing CME event