HPV and bacterial flora increasingly implicated
By Brian B. Burkey, MD, FACS
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Over the past decade, clinicians and researchers involved in the treatment of squamous cell carcinoma (SCC) of the upper aerodigestive tract have noted a significant increase in the incidence of these cancers in the oropharynx. In fact, more than 7,000 new cases of oropharyngeal SCC are being diagnosed each year, many of them in men with a minimal history of tobacco use.
Cleveland Clinic’s Head & Neck Institute, in conjunction with its Taussig Cancer Institute, is conducting several ongoing studies to assess various aspects of this disease entity.
Most SCCs of the oropharynx are now being attributed to the effects of human papillomavirus (HPV) infection. HPV integrates into the cellular DNA and facilitates the development of neoplastic cells and eventually cancer. Even aside from its association with oropharyngeal cancers, HPV is a major health problem in the United States. It has become the most common sexually transmitted disease, and at least half of all sexually active people will be exposed to this virus.
Of the more than 100 strains of HPV, two — HPV-16 and HPV-18 — are associated with an increased risk of oropharyngeal cancer. These are the same two strains that are linked to cervical cancer in women. It is surmised that the connection between the two manifestations is that they are both spread by direct mucosal contact.
The increase in HPV infection among men, and hence the risk of oropharyngeal cancer, appears to be related to the performance of oral sex upon infected women.
The HPV-related oropharyngeal cancers are distinct from the base-of-tongue and tonsillar cancers that historically have been seen in older populations of patients with a history of tobacco and alcohol abuse, who are usually HPV-negative.
We are now finding that HPV-related oropharyngeal cancers are occurring in younger patients in whom tobacco abuse is much less common. These patients present with a more advanced stage of disease, and their cancers are more poorly differentiated than are HPV-negative tumors.
The good news is that HPV-related oropharyngeal cancers respond better to treatment than do the tobacco- and alcohol-related oropharyngeal cancers. As many as 80 to 90 percent of HPV-related cancers can be cured with combined-modality treatment — either chemoradiation therapy or surgery and radiation therapy. These cure rates are twice as high as those for HPV-negative tumors.
One of the current studies underway in Cleveland Clinic’s Head & Neck Institute and Taussig Cancer Institute is an investigation of the prevalence of HPV in SCCs of the cervical lymph nodes in which the primary site is unknown. Our goal is to correlate HPV status with treatment outcomes. The complete genesis of these cancers remains controversial, but many clinicians believe they originate in small nests in the oropharynx.
Our findings suggest that the improvement in survival in patients with HPV-positive oropharyngeal cancers is also seen in those with HPV-positive SCC without a known primary site, regardless of the type of treatment. We presented preliminary findings at the 8th International Conference on Head and Neck Cancer.
We are also working with researchers in Cleveland Clinic’s Genomic Medicine Institute to investigate factors that promote oral cancers. Most cancers of the oral cavity are SCCs. Many of them may be related to the bacterial flora that is present in the patient’s mouth.
We are currently conducting an NIH-funded study that correlates certain bacterial populations in the mouth and their association with oral cancers. Our early findings, including a study published in Human Molecular Genetics, suggest that further investigation of bacterial populations in oral cancers is warranted in order to improve cancer diagnosis, treatment and prognosis. Our results also suggest a potential role for salivary screening as a measure of risk for oral cancers.
The two studies mentioned above, as well as others that are ongoing in the Head & Neck Institute, relied greatly on the availability of two databases that we developed.
One database, which was started in 1994, contains potentially useful demographic information about patients with tumors of the upper aerodigestive tract. We hope these data may yield clues to the development of these cancers.
The other database, which was started in 2009, is a tissue repository where we save tumor tissue, saliva, blood and normal tissue obtained from patients with head and neck SCCs and retrieve this material for use in studies. The tissue repository is key to the future investigation of cancers, which will become increasingly sophisticated as the roles of genetics and microbiology move to the forefront of cancer research.
As evidence of the multidisciplinary approach increasingly demanded to advance head and neck cancer research, the repository was developed with the help of Cleveland Clinic’s Genomic Medicine Institute and Department of Plastic Surgery.

Timing and type of side effects differ greatly from chemotherapy

Dedicated multidisciplinary teams support 84 ultra-rare cancers

Sessions explore treatment advances and multidisciplinary care
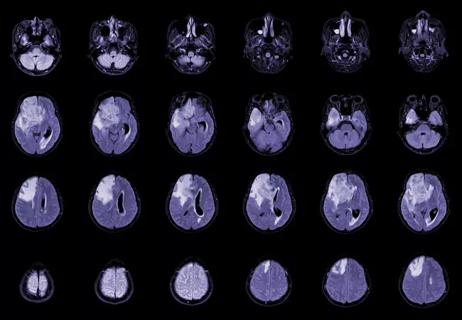
New research from Cleveland Clinic helps explain why these tumors are so refractory to treatment, and suggests new therapeutic avenues
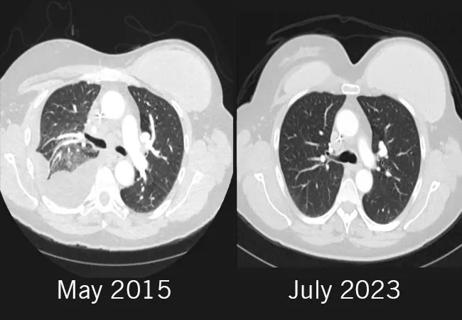
Combination of olaparib and carboplatin results in complete durable response for a patient with BRCA2 and “BRCAness” mutations
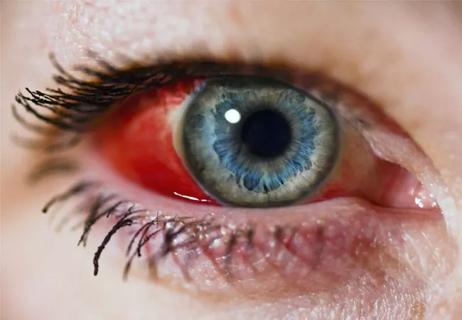
Early communication between oncologists and ophthalmologist warranted

Case-based course delves into latest treatment approaches

Long-term relationship building and engagement key to gaining community trust