Results of a comprehensive review of research and outcomes
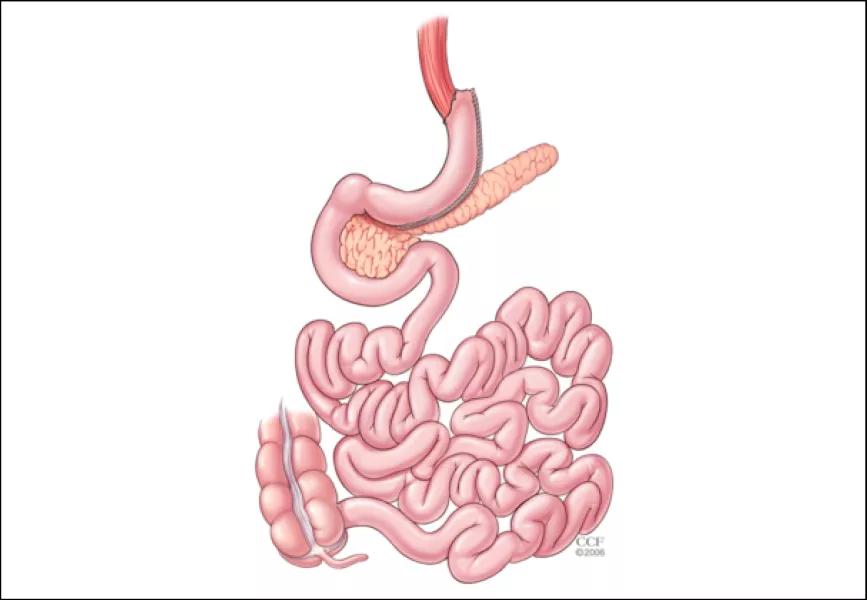
Emerging data reveals sleeve gastrectomy (SG) may be safer and provide some additional metabolic advantages over Roux-en-Y gastric bypass (RYGB), according to a comprehensive review this year of available research and outcomes data by bariatric surgeon Ali Aminian, MD.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dr. Aminian’s findings appear in the August 2018 issue of Trends in Endocrinology & Metabolism.
“SG and RYGB are similar treatments and both are effective, durable and very safe,” Dr. Aminian emphasizes. The two procedures account for more than 95 percent of primary bariatric procedures in the United States. However, until recently, RYGB was the more dominant surgery.
In 2011, the estimated number of RYGB procedures performed in the U.S. was almost two times the number of SG cases. Five years later, in 2016, the number of SG cases was three times higher than RYGB.
“There are obvious reasons for the rapid growth of SG,” notes Dr. Arminian. “SG involves only partial excision of the stomach without rerouting of the gastrointestinal tract. It is a less technically demanding procedure with few postoperative complications and long-term nutritional problems, compared to the more complex gastrointestinal diversionary procedure.”
Dr. Aminian acknowledges expressed concerns about the metabolic effects and durability of outcomes after SG, but points to three recent randomized clinical trials, including the pivotal STAMPEDE trial, which provide evidence of the efficacy and durability of SG.
“Both RYGB and SG are proven to be safe,” says Dr. Aminian. “The frequency of postoperative adverse events is relatively similar, although observational studies have shown fewer early and late complications after SG,” he says. “Lack of gastrointestinal anastomosis, intact pylorus and unaltered gut absorption contribute to the excellent safety profile of SG.”
Dr. Aminian adds that there are very rare, but potentially life-threatening complications including internal herniation, anastomotic marginal ulceration and hyperinsulinemic hypoglycemia, which mainly occur after RYGB, but not after SG.
“Worth noting is that while RYGB usually improves gastroesophageal reflux disease (GERD), postoperative worsening or development of GERD is more commonly seen after SG,” says Dr. Aminian. “GERD, in most cases, can be effectively managed with medical therapy,” he adds. “In rare cases, post-SG patients with severe GERD would benefit from conversion of their SG to RYGB.”
Dr. Aminian’s review also suggests relatively comparable outcomes with respect to diabetes. Both procedures significantly improve mild diabetes, and both have similar efficacy in achieving diabetes remission with severe diabetes. “There is an intermediate group, however, in which RYGB would be significantly more effective than SG in the treatment of diabetes,” Dr. Aminian notes.
Both procedures appear to be similarly effective in long-term weight loss, reducing blood pressure, improving lipid panel effects and increasing HDL levels, although one published prospective study showed SG can improve HDL function.
A growing body of evidence shows SG improves non-alcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH), more so than RYGB, but more evidence is needed to confirm these findings.
Recent studies have also suggested that RYGB is associated with increases in plasma trimethylamine-N-oxide (TMAO) levels, potentially a result of the significant shift in gut microbiota composition after RYGB. There is no evidence that TMAO levels increase after SG.
“It’s conceivable that lower TMAO levels after SG may have protective cardiovascular and metabolic effects,” says Dr. Aminian. “Interestingly, RYGB and SG alter the composition of gut microbiota differently, and distinct patterns in gut microbiota may contribute to contrasting changes in TMAO levels after surgery,” he adds. Further study is needed to assess the long-term clinical importance of this finding.
Furthermore, in the STAMPEDE trial, SG was shown to contribute to a significant decrease from baseline in the albuminuria.
“All considered, SG appears to be a safer procedure with distinct metabolic advantages, including favorable impact on the TMAO pathway, HDL function, diabetes, NAFLD/NASH, albuminuria, body weight and overall quality of life,” Dr. Aminian concludes. “More mechanistic and clinical research will better delineate metabolic impacts of SG, but current evidence supports the upsurge we’re seeing in SG procedures.”
Radiofrequency ablation significantly reduces symptom severity, shrinks nodules

Maternal-fetal medicine specialists, endocrinologists and educators team up

Giving young patients a hand as they take charge of their own health

Case illustrates how easily condition can mimic preeclampsia
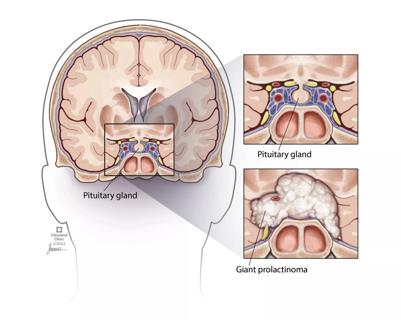
Analysis examines surgical resection of rare pituitary tumors
Screening and medication key to better outcomes
Spinal cord stimulation can help those who are optimized for success
Incidence, outcomes and management