'Weight may accelerate aging of brain’ studies show
By Brigid Titgemeier, MS, RDN, LD
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
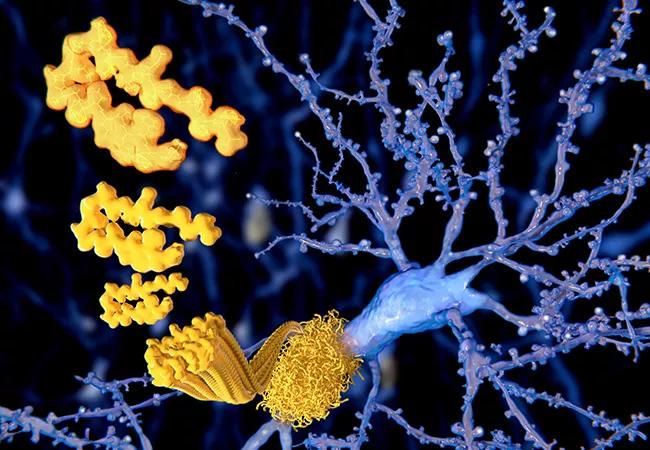
In functional medicine, Alzheimer’s disease is often referred to as type 3 diabetes because studies show that glucose intolerance leads to an increased risk of developing Alzheimer’s disease and vascular dementia. Elevations in blood sugar levels may negatively affect memory and brain function, even in non-diabetic patients.
A 2013 cross-sectional study that included 141 non-diabetic individuals found that elevations in long-term hemoglobin A1c and short-term blood glucose were associated with lower cognitive performance in all three memory tasks conducted: delayed recall, learning ability and consolidation. When analyzing the hippocampus, they found that lower levels of fasting glucose were associated with higher hippocampal volume and improved hippocampal barrier density.
The researchers observed these changes even in the absence of type 2 diabetes, emphasizing that cognitive decline may begin sooner than expected and that blood sugar stabilization should be discussed with patients before reaching a hemoglobin A1c above 5.5 percent. Excessive added sugar, refined grains and processed foods are main culprits of high blood sugar levels, type 2 diabetes and cognitive decline, yet many individuals are unaware of that connection. Patients should be educated on the impact that diet and exercise can have on reducing their risk for type 2 diabetes and dementia before reaching the point of a diagnosis.
Of course improving dietary habits and engaging in physical activity decrease risk of obesity, which may also be associated with cognitive decline. A 2005 longitudinal population-based study found that being overweight or obese led to a respective 35 percent and 74 percent increased risk of dementia later in life. The risk of dementia was independent of other comorbid conditions.
Additional evidence suggests that weight may accelerate aging of the brain. A 2016 cross-section study indicates there’s an association between obesity and age-related brain structure changes. The researchers compared the white matter volume between brains of lean and overweight/obese individuals and found an increase in brain age of 10 years associated with increased adiposity. In other words, obese individuals who were 50 years old appeared to have brain-related aging comparable to a 60 year old lean individual. Interestingly the differences in white matter were observed in brains that were 40 years and older, indicating that the brain may be particularly vulnerable to increased adiposity in middle age years.
Elevated blood sugar and excess weight are two common measurements of a person’s metabolic health and may also indicate risk of brain aging or cognitive decline. While genetics plays a role in risk of Alzheimer’s disease, the impact of environmental and lifestyle factors should not be dismissed. In order to help patients better manage their blood sugar levels, shed excess weight and sharpen their brains, it’s important to discuss the powerful role of lifestyle modifications as early as possible.
In functional medicine, we work with patients to help them improve their diet and incorporate more anti-inflammatory foods into their meals to reduce the risk of cognitive decline, improve markers of glucose metabolism and promote weight loss. Patients need to be made aware of the powerful connection that exists between lifestyle choices and risk of dementia.

A first-of-its-kind study

Meet M. Elaine Husni, MD, MPH

Nutritional pharmacology can have profound effects

Research, value-based care and looking at outcomes

Functional Medicine spurs lifestyle changes that target source of pain

Case study illustrates effectiveness of functional medicine

What it takes to get certified
Rapid advances in science call for clinical integration