White paper and Digital Health Summit outline key perspectives, goals
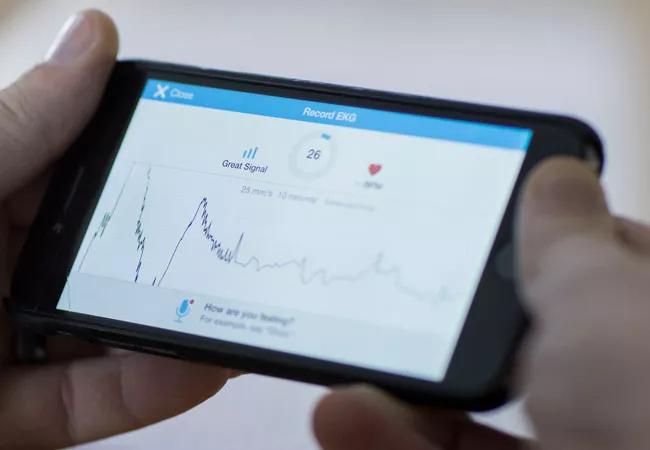
The most striking trend about recent cardiac electrophysiology (EP) practice may be the unprecedented proliferation of digital data across multiple fronts. There are ceaseless data feeds from physician-facing technologies like the electronic health record (EHR), cardiac implantable electronic devices (CIEDs) and medical-grade heart monitors. There’s the explosion in patient-facing devices such as wearable biometric monitors. And there are ever more opportunities for physician-patient digital interactions, such as telemedicine and patient portals.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Yet the mountains of resulting data are not all ending up in the same places or residing with the same stakeholders. This conundrum has prompted the Heart Rhythm Society (HRS) to issue the first high-profile call to action for transparent sharing of digital health data, which the group did at its first Digital Health Summit on May 8 at its annual scientific sessions and in a white paper co-authored by Cleveland Clinic electrophysiologist Khaldoun Tarakji, MD, MPH, that’s being published in the journal Heart Rhythm.
“Realizing the promise of digital health will mean ensuring that all stakeholders — especially patients — have complete, secure and transparent access to their data,” says Dr. Tarakji, a member of the HRS Digital Health Working Group, which drafted the white paper and led the Digital Health Summit. “These efforts we’re undertaking are meant to profile the present state of digital health data access and the perspectives of key stakeholder groups as well as to urge heart rhythm clinicians to help lead development of best practices in digital health data sharing.”
The working group’s efforts were informed by a one-day “think tank” in August 2018 that assembled patients, healthcare professionals and leaders from the device and pharmaceutical industries for their perspectives on a range of developments in digital health data. FDA representatives also weighed in through separate discussions with the working group.
The white paper lays out the perspectives of several stakeholder groups — including patients (both those with CIEDs and those using wearable consumer biometric devices), the cardiac EP clinical team, regulators and industry — as well as key considerations around adoption of digital health tools by the medical team and opportunities for integrating digital health into clinical research.
Advertisement
The paper concludes with a helpful summary of key points from each perspective and section. Highlights include the following:
The authors of the white paper note that several important questions — including privacy, security and reimbursement around consumer wearable technologies — were beyond the scope of this initial document and remain for another day. They also make clear that the document will require updating as fast-evolving digital health technologies advance and as experience mounts.
Advertisement
“The manuscript proposes interim solutions such as using EHR patient portals,” the authors write. “These interim steps should not be considered acceptable end points.”
“There’s a growing expectation among patients and the general public for transparent and secure access to health data,” observes Dr. Tarakji. “Through this white paper and summit, the cardiac electrophysiology community is helping ensure that access will be provided in a way that reduces inefficiencies and makes medicine more personalized for patients.”
Advertisement
Advertisement

How Cleveland Clinic is using and testing TMVR systems and approaches

NIH-funded comparative trial will complete enrollment soon

How Cleveland Clinic is helping shape the evolution of M-TEER for secondary and primary MR

Optimal management requires an experienced center

Safety and efficacy are comparable to open repair across 2,600+ cases at Cleveland Clinic

Why and how Cleveland Clinic achieves repair in 99% of patients

Multimodal evaluations reveal more anatomic details to inform treatment

Insights on ex vivo lung perfusion, dual-organ transplant, cardiac comorbidities and more