Viewpoints from Steven Wexner, MD, PhD (Hon)
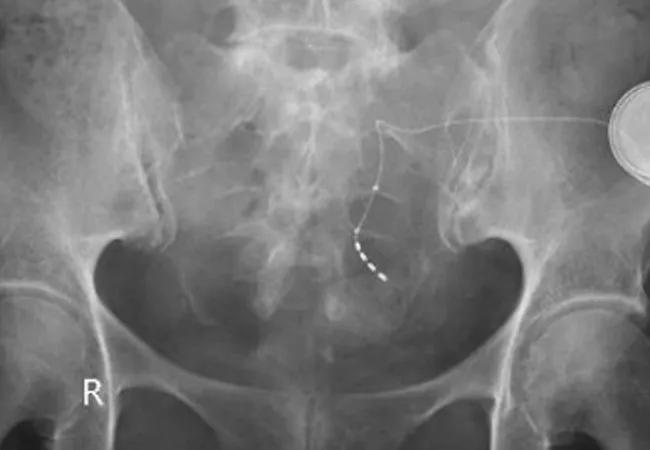
The number of treatment options for fecal incontinence enjoyed a brief spike when stimulated graciloplasty (Wexner et al, Baeten et al), the artificial bowel sphincter (Edden et al, Hong et al), and the magnetic anal sphincter Wexner et al were commercially available. That number of options has now been reduced to include only radiofrequency (Ruiz et al) and injectables (Wexner) along with sacral neuromodulation (Wexner et al, Wexner et al).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Outside of the United States, posterior tibial nerve stimulation (Horrocks et al, Wexner) may be utilized but has limited efficacy. The benefits of sacral neuromodulation have been confirmed in patients with sphincter defects, following sphincter repair and with pudendal neuropathy. Less well-established is the potential benefit of sacral neuromodulation in patients who have had rectal resections with neorectal reconstructions (Mizrahi et al).
In order to help fill our void in knowledge about the potential benefits of sacral neuromodulation in this setting, Mege and coworkers from France identified 16 patients who underwent sacral neuromodulation for neorectal reconstruction following coloanal anastomosis, colorectal anastomosis, or ileal pouch and anastomosis.
The authors found significant decreases in the number of stools per day, the number of fecal incontinent episodes, urgency, the low anterior resection (LAR) score and the Wexner (Cleveland Clinic) Incontinence Score1 following sacral neuromodulation in the six patients in whom a restorative proctocolectomy with ileal pouch anal anastomosis had been performed. They also identified significant decreases in all of these variables, except urgency, in the eight patients in whom a coloanal anastomosis was performed.
Some of the improvements were quite dramatic, such as the Wexner Incontinence Score decreasing from a median of 15 before to a median of 1.5 after sacral neuromodulation in patients following IPAA. Similarly, there was a decrease in the median Wexner incontinence score from 14.5 to 5.5 in patients in whom a coloanal or colorectal anastomosis was performed. Comparable decreases in the LARS score were from a median of 34 to a median of 12 and a median of 33 to a median of 9, respectively.
Advertisement
As we had recently demonstrated in our own publication (Mizrahi et al), this therapy does have a role in patients who have had rectal extirpation followed by neorectal reconstruction. However, the French series did reveal a more significant improvement with success rates of 75 percent based upon intent to treat analysis and 86 percent of patients in whom the pulse generator was placed.
I congratulate the authors on this impressive addition to the literature and on their compelling data, which support, at the very least, a trial of percutaneous nerve evaluation ― perhaps with a tined lead ― in patients who have undergone either coloanal, colorectal or ileoanal anastomosis.
Reference:
1. Jorge JMN, Wexner S. Anatomy and physiology of the rectum and anus. Eur J Surg 1997;163:723-731.
Advertisement
Advertisement

Multidisciplinary framework ensures safe weight loss, prevents sarcopenia and enhances adherence

Study reveals key differences between antibiotics, but treatment decisions should still consider patient factors

Key points highlight the critical role of surveillance, as well as opportunities for further advancement in genetic counseling

Potentially cost-effective addition to standard GERD management in post-transplant patients

Findings could help clinicians make more informed decisions about medication recommendations

Insights from Dr. de Buck on his background, colorectal surgery and the future of IBD care

Retrospective analysis looks at data from more than 5000 patients across 40 years

Surgical intervention linked to increased lifespan and reduced complications