Helping patients with cancer struggling with depression, anxiety and other mental health issues
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2241774/13511832)
Living with cancer takes an emotional toll. Yet access to care in the field of psycho-oncology, which focuses on mental healthcare in patients who have cancer, can be challenging. There aren’t a lot of training programs tailored to psycho-oncology, and the pathophysiology and pharmacology in this patient population are complex.
In a recent episode of Cleveland Clinic’s Cancer Advances podcast, Kaleena Chilcote, MD, Director of Psycho-Oncology at Cleveland Clinic’s Taussig Cancer Center, discusses how she and her colleagues support patients with cancer.
“We see patients with new mental health symptoms, but we also see patients who have chronic struggles with their mental health. So, it’s a good mix of people,” says Dr. Chilcote. “Our most common referrals come from symptoms of depression, anxiety or sleep disturbances.”
Dr. Chilcote delves into:
Click the podcast player above to listen to the episode now, or read on for a short edited excerpt. Check out more Cancer Advances episodes at clevelandclinic.org/podcasts/cancer-advances or wherever you get your podcasts.
Podcast host Dale Shepard, MD, PhD: Why psycho-oncology, and how does that really impact a patient’s journey through cancer?
Advertisement
Dr. Chilcote: Mental health struggles in cancer are incredibly common. We know, in general, probably 25% of patients who have cancer, at any given point in time, meet criteria for a depressive disorder. That’s a lot of people. And it’s probably a similar number when we look at anxiety. Insomnia, it’s probably even higher than that. So, it’s a huge part of the population that we serve.
We also know that cancer can exacerbate struggles that people are already having. And we know that when we struggle with our mental health, it can significantly impact our cancer care and perhaps our cancer outcomes. Just using depression as an example, we know that people who have cancer and also have depression at the same time are likely to make different choices with their treatments. They’ve done good studies, like with breast cancer, where they show patients who have depression and breast cancer are less likely to participate in adjuvant chemotherapy compared to someone who does not have depression but has the exact same cancer features.
We know that people engage with their teams in different ways when they have depression. They’re more likely to call frequently for appointments in between those that are scheduled or to go to their local emergency department to request hospitalizations for symptom management. Depression increases all those things.
And depression also increases cancer-related outcomes, maybe for reasons we don’t always understand. But very specific studies have shown things like, someone who has depression and has a stem cell transplant is more likely to develop chronic graft-versus-host than someone who does not have depression. And we know even just mortality in general is higher in patients with comorbid depression as they go through their cancer journey.
Advertisement
So, there are very clear reasons we as physicians should be paying attention to this, and why hospital administrators are starting to pay more attention to this as well.
Advertisement
Advertisement

Key themes and insights into the family-caregiver experience

First-of-its-kind clinic for immune-related adverse events supports oncologists in managing severe side effects
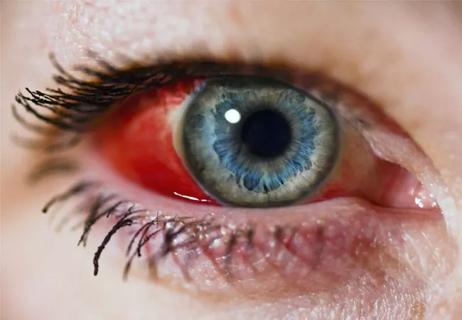
Early communication between oncologists and ophthalmologist warranted

Variables affect nuances of the conversation

Driving advances in cancer care
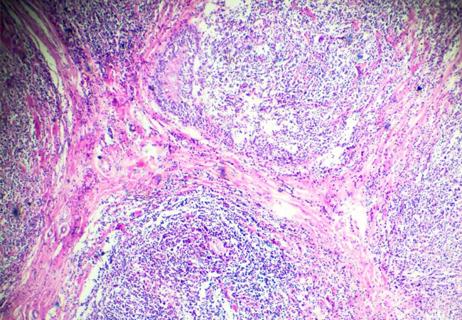
Challenges emerge with application of interim PET scans

Complex, bidirectional interactions exist between cancer, therapy, toxicities and eating behaviors

How ‘Let’s Get Moving!’ is improving physical activity in children undergoing cancer treatment