Microsurgery technique may provide relief to patients
Patients who develop lymphedema following breast and other types of cancer treatment experience limitations on their activities, limb discomfort, cosmetic deformity and increased susceptibility to infection. In the past, the primary way to treat the condition has been a time-consuming daily regimen designed to reduce swelling and prevent lymphedema from getting worse. Now, specialists at Cleveland Clinic are performing complex lymphaticovenous bypass (LVB), which is providing patients some improvement of their lymphedema. In this Q&A, plastic surgeon, and Director of the Cleveland Clinic Microsurgery and Breast Reconstruction Fellowship, Graham Schwarz MD, provides an overview of the procedure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A: Patients with lymphedema after cancer treatment typically have a proximal obstruction in lymphatic flow resulting in inflammatory fluid accumulation which progressively damages tissue in the arms or legs. With LVB, we connect healthy lymphatics and veins allowing us to bypass the obstruction so that lymph fluid can move directly into the venous system.
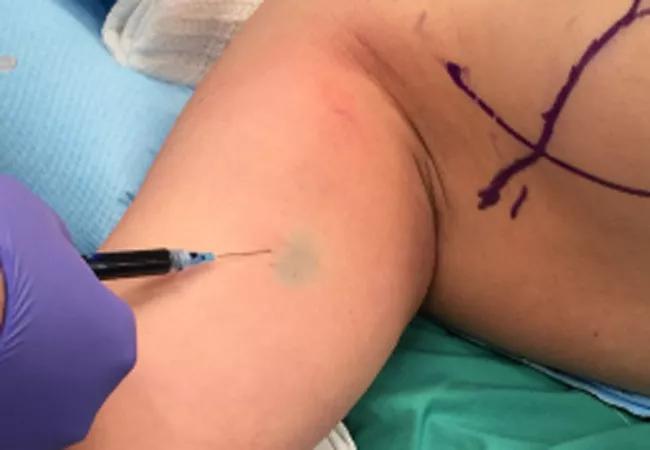
First, we perform a lymphangiogram by injecting a fluorescent dye — usually indocyanine green or ICG — into the extremity affected by lymphedema. A Near-Infrared Camera detects the dye and enables us to perform lymphatic mapping to identify operative targets for connecting lymph vessels to veins. We locate viable non-diseased channels at different intervals along the extremity and make incisions at these locations. Using a supermicrosurgery technique, we then perform submillimeter lymphaticovenular anastomoses. After the connections are made, we again use a lymphiangiogram and tracer dyes to confirm that the connections are patent.
A: Well-selected patients can experience a 30 percent or greater reduction in limb size. Another benefit is a reduced need for constant and intensive compression regimens. Before the procedure, patients may spend three or more hours a day wrapping their arm or using a pump to keep the lymphedema from getting worse. After the procedure, patients may be able to significantly reduce time devoted to preventive activities.
A: In VLNT, we borrow lymph nodes from another part of the body and use them in an area affected by lymphedema to restore or improve lymphatic drainage. With LVB we don’t borrow lymph nodes. We are strictly rerouting the plumbing in the lymphatic system by creating new connections to get around blockages.
Advertisement
A: With LVB, we are not creating a donor site by borrowing lymph nodes from another area of the body, which eliminates some of the risk of complications. Also, the connections that we make during LVB are very close to the surface of the skin, so it is a less invasive procedure. Patients who have a bypass can usually go home the same day or the next day. With VLNT, patients may be in the hospital for two to three days.
A: Patients in the early stages of lymphedema who do not have a lot of skin and subcutaneous tissue changes are good candidates for LVB. The bypass procedure also appears to work better in patients with upper extremity lymphedema rather than leg lymphedema. Gravity causes blood to pool in the venous system, so it takes more work for the lower pressure lymphatic flow to overcome vein back flow pressure in the legs. Functioning valves are important to maintaining forward flow against gravity, and those who have leaking valves in the venous system will not have an effective result.
When we are treating patients with lymphedema, we prepare them in advance for both LVB and VLNT. Then we decide which procedure is best based on what we find through preoperative testing, lymphangiography and mapping that we conduct in the OR.
Some patients benefit from a staged approach to surgical lymphedema treatment, while others may benefit from combining surgical approaches in a single operative setting. For example, we might perform a series of LVBs in the lower arm, and one to 1.5 years later, the patient may return for additional bypass or lymph node transfer in the upper arm depending on their individual pattern of disease and localized response to treatment.
Advertisement
A: This is another big difference between LVB and VLNT. With LVB, patients may see a reduction in swelling in two to six months. With VLNT, they may not see results for up to a year and a half.
A: We hope that as we fine-tune our techniques and refine our understanding of their effects on lymphedema progression we can further individualize treatment. Our goal is to improve the quality of life of patients who live with this condition. Prevention is another important area, and we currently have a study underway that explores whether performing LVB on high-risk patients concurrent with cancer surgery will decrease the risk of developing lymphedema.
Advertisement
Advertisement

Combining advanced imaging with targeted therapy in prostate cancer and neuroendocrine tumors

Early results show strong clinical benefit rates

The shifting role of cell therapy and steroids in the relapsed/refractory setting

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors