Meticulous planning made this two-stage repair of an infant's heart successful
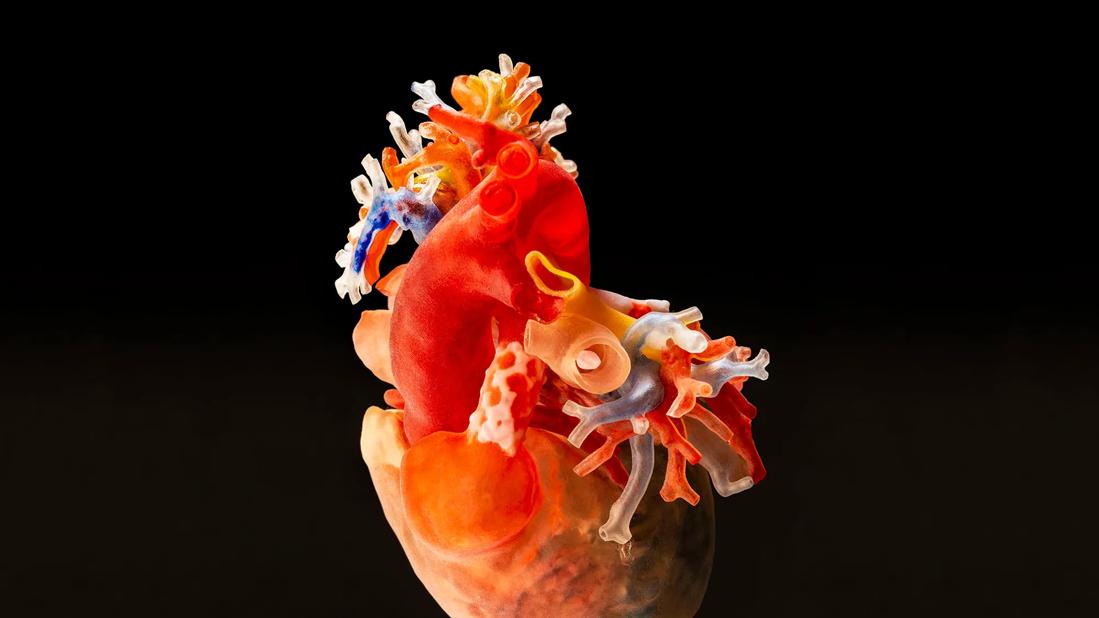
A highly detailed three-dimensional model of a newborn girl’s severely malformed and defective heart enabled Cleveland Clinic Children’s surgeons to plan and execute a challenging two-stage repair.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The infant was born with a rare cardiac abnormality (diagnosed in utero) called dextrocardia with heterotaxy syndrome, in which the heart is located in the right side of the chest rather than the left and its base-apex axis is oriented rightward.
As with many heterotaxy cases, the patient had a number of other heart defects: an absent pulmonary valve, a septal defect, and a single common atrioventricular valve in the center of the heart instead of two separate valves.
But there was a bright side to her case. The girl had a small but functional left ventricle, and Hani Najm, MD, Chair of Pediatric and Congenital Heart Surgery at Cleveland Clinic, felt this gave him options.
“Generally, these types of patients end up with a univentricular heart,” he says. “Initially, the heart’s circulation is rerouted such that the superior vena cava (SVC) drains into the right pulmonary artery. Then later on, around ages 3 to 5 years, the inferior vena cava (IVC) is also diverted into the pulmonary artery. The heart then pumps blood only to the body, not to the lungs [which receive passive blood flow]. But in this case, we didn’t want to throw out that small left ventricle. It was small but good enough to pump blood to the lungs.”
Why was it so important to involve the left ventricle? Univentricular hearts put a great deal of strain on the IVC and can result in a range of serious side effects that can damage the lungs, the liver and the gut. Plus, Dr. Najm says, the procedure always eventually fails.
Advertisement
So he decided to perform two surgeries on the infant. The first occurred six days after her birth, when Dr. Najm and his colleagues rerouted the blood flow to her working right ventricle as a bridge to eventually correcting the other issues with the problematic left side of her heart. “This gave her good blood-oxygen saturation,” Dr. Najm says.
When the child was 9 months old, he performed the second, more complex surgery: a biventricular conversion that included a Glenn anastomosis, which is designed to allow blood flow to the lungs. The first part of the operation connected the SVC directly to the pulmonary artery so that blood from the upper half of the girl’s body would flow directly to her lungs instead of being pumped there from the left ventricle.
The second part of the operation involved diverting blood from the IVC to the small left ventricle — what’s known as an arterial switch, because the IVC usually feeds the right ventricle — and creating a left-ventricle-to-pulmonary-artery connection. That allowed the girl’s left ventricle to pump blood from the lower part of her body into the lungs and her right ventricle to pump oxygenated blood back to her body.
Because the girl would be one of the youngest patients to undergo this procedure, and because her heart contained several unusual anatomical problems, the team generated a three-dimensional (3-D) printed replica of her heart — derived from a CT scan — to aid preparation for the intricate surgical repairs.
Children born with these problems are said to have “unseptatable” hearts, Dr. Najm says, “but we’re saying with the use of 3-D printing, we can septate them. Why? Because when you have a replica of the heart in your hand as a surgeon, you can see more clearly how to pursue these difficult cases. I would look at the patient’s 3-D heart for hours before deciding — with reasonable confidence — that these novel procedures were feasible. It is an invaluable tool when planning complex repairs.”
Advertisement
Fully recovered from the complex cardiac surgeries, the child is now an energetic 1-year-old. The only additional surgeries she will need, Dr. Najm says, are operations to replace the conduit between her left and right ventricles. Such operations, he says, are fairly routine.
Advertisement
Advertisement

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes

Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve