Infants born between 35 and 37 weeks are still at risk of complications
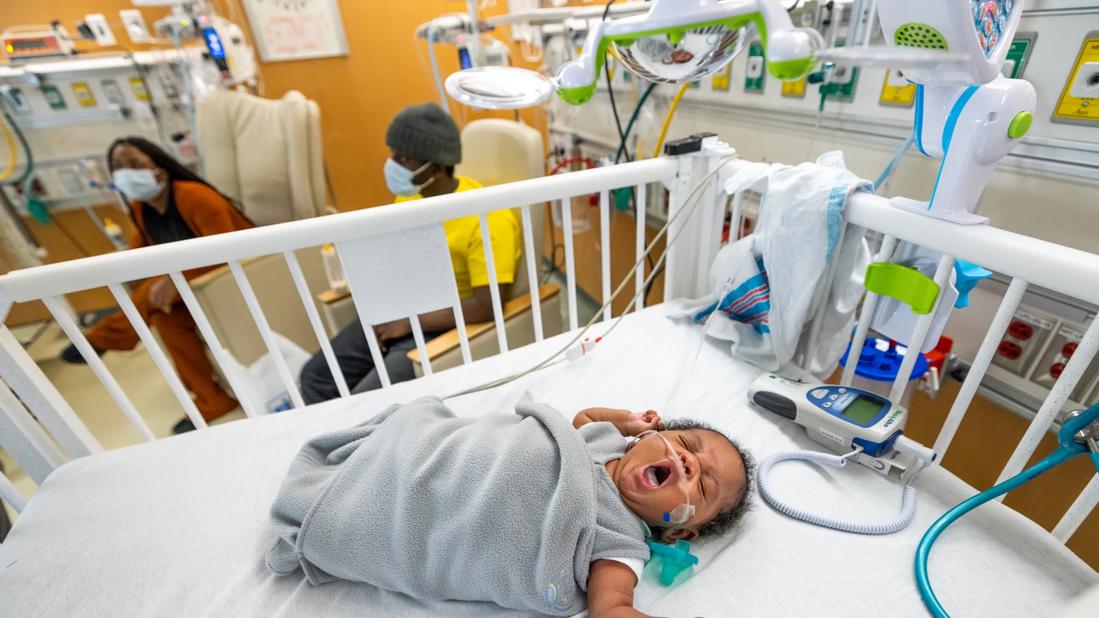
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/911a1a55-06f7-48f1-802a-73c93ee27121/CCC_3660083_02-27-23_1267_AMO-jpg)
650×450-Late-Preterm-Birth-Baby
Worldwide, the incidence of late preterm deliveries has been increasing. Late preterm newborns – those born between 340/7 and 366/7 weeks of gestation – comprised approximately 70% of preterm deliveries in the United States in 2018. These late preterm infants are sometimes overlooked due to their size and maturity, but those last few weeks in utero are crucial for organ development. Common medical issues for late preterm infants include respiratory distress, temperature instability, hypoglycemia, hyperbilirubinemia, apnea and feeding difficulties.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Studies show that late preterm infants are at increased risk of mortality – not only in the first month or so, but in the whole first year when compared to infants born at full term,” says Sreenivas Karnati, MD, a neonatologist with Cleveland Clinic Children’s.
“Although mortality risk is much higher in extremely premature infants, those born late preterm have a 3-7x higher risk of death in the first year than term infants. One issue with these studies it that they don’t always pinpoint the specific cause of mortality, though congenital malformations, infection and respiratory distress are likely culprits,” Dr. Karnati explains.1-3
Each year, approximately 10,000 infants are born in Cleveland Clinic birthing centers. Of these, about 1,000 infants are born preterm, and about 650-700 of those are born late preterm.
At Cleveland Clinic Children’s, infants born at < 35 weeks gestation are admitted to the special care nursery automatically, and are discharged home when it is deemed safe, according to Dr. Karnati. Neonates born between 35-37 weeks gestation, who have no other issues, are admitted to the newborn nursery for observation.
During this hospital stay, lactation consultants address feeding problems and a multidisciplinary group of caregivers provide education to parents about possible complications, emphasizing the importance of prompt follow-up. The first visit to the pediatrician is scheduled prior to discharge.
“A lot of brain development occurs during the third trimester of pregnancy, and studies show that, at 34-35 weeks’ gestation, the brain is only two-thirds the size of term infants in terms of structure and maturity,” continues Dr. Karnati. “This puts these babies at higher risk for cerebral palsy or developmental delays.”4-6
Advertisement
For these reasons, he says, it is important for pediatricians to identify patients born late preterm and keep a close eye on their development.
Pediatricians are key players in the care of these infants. They should educate parents about what to watch for, and take action at the first sign of any developmental delay. Interventions such as physical therapy, speech therapy and occupational therapy can be quite helpful when undertaken early in life.
Studies suggest that later preterm infants are at very high risk for hypothermia, hypoglycemia and jaundice, and increased odds of readmission.7-11 Although these infants may be safely discharged home, it is extremely important that they are seen by a pediatrician within the first 48-72 after discharge. This visit helps pediatricians monitor weight gain and look for signs of jaundice or temperature dysregulation.
“Overall, these babies do fairly well, but they need to be watched closely by their parents and pediatricians for the first few years. Vigilance in outpatient clinics should help pediatricians to identify early signs of any developmental delays and promptly refer to appropriate therapies,” concludes Dr. Karnati.
Advertisement
Advertisement
Life-changing gene therapy is currently under FDA review
How evolving medical therapies and more precise patient selection are reshaping the role of intestinal transplantation
Cleveland Clinic specialist discusses the new clinical practice guideline
Introducing Prajwal Rajappa, MD, MS, Director of Pediatric Precision Oncology
The one-stop THRIVE clinic addresses renal, psychosocial, educational and other challenges alongside cardiac surveillance
Study found lower rates of nausea, vomiting and healthcare use through 12 months of follow-up
What to know about the condition, and 5 strategies to improve patient care
Biologic therapy and advances in monitoring may ease treatment and follow-up for families