Reducing nasal injuries keeps treatment flowing
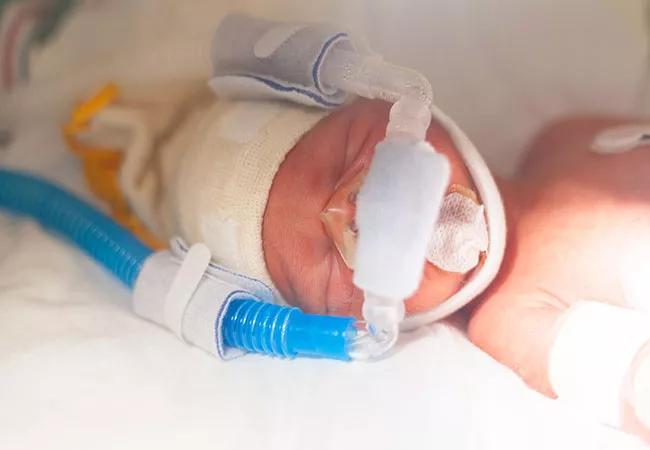
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/276267b4-5794-48aa-b256-a97981695009/650x450-Nasal-Injuries-NICU-babies_jpg)
650×450-Nasal-Injuries-NICU-babies
Nasal continuous positive airway pressure (CPAP) helps premature infants breathe until their lungs mature. But injuries to their noses caused by CPAP prongs can sometimes force doctors to change nasal interface and terminate CPAP support too soon, which can lead to chronic lung disease (CLD). Hany Aly, MD, Chair of Neonatology at Cleveland Clinic Children’s, has shown that auditing the CPAP interface application and nursing checklist completion at the bedside can reduce nasal injuries and allow patients to continue receiving the gold standard of care.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Our NICU CLD rate is already low, but we want to do everything we can to prevent as many of these injures as possible,” he says. “We’ve shown that one more check to make sure we’re doing everything right makes a difference in the lives of these very tiny patients.”
While CPAP interfaces for NICU patients aren’t that much different than those for adults, using them correctly requires more precision. “The nose of a premature baby is small, and putting small prongs inside a small nose is not an easy task. If they’re placed just one millimeter too deep, it can cause real damage,” he says.
Not only does the size of a premature baby’s nose present a challenge, but the skin does too: it’s very fragile. “If you poke the nose with hard plastic, that can destroy the skin and cause ulcers in the nose, then you usually have to stop using CPAP support on those patients,” Dr. Aly says. Such nasal injuries are common: a 2018 British Journal of Medicine survey found that nasal injury rates ranged from 20% to 100%, with higher rates for babies with gestational age less than 30 weeks.
Nasal injuries are staged as follows: redness of the skin (stage I), skin abrasion (stage II), and ulcers (stage III). These injuries hamper care. Alternative ways of helping premature infants breathe exist, but they’re less effective, says Dr. Aly.
Cleveland Clinic’s rate of CLD was already one of the lowest in the country, according to Dr. Aly, when his team implemented a checklist to ensure the CPAP nasal interface is perfectly adjusted for each infant. Every nurse on every shift for every infant on CPAP support performs each task on the checklist, which includes items like making sure the humidifier water level is correct, neck roll is the proper size and in the correct position, and that nasal prongs are positioned correctly (i.e., not touching the columella or deviating to the side).
Advertisement
While the checklists proved effective at the outset, Dr. Aly found that the checklist tasks were only being completed in the correct order about 40% of the time. “Whenever you try something new, it works well, and everyone sticks to the program. But it’s easy for things to slide over time. People tend to get loose with the rules and not follow them exactly,” he says. He also found that nasal prongs were positioned incorrectly for nearly 30% of patients.
To combat these issue, Dr. Aly’s team instituted a Process Confirmation Task Force, which audited the checklist process to ensure adherence and completion. As part of the process, a nurse conducts “random non-scheduled visits to check on colleagues and make sure checklists are being filled out,” he says. For an audit to be considered complete, every single item must be done in the order they appear on the checklist. The program started in September 2019. By October, checklist adherence rates were over 60%.
Since the audits began, rates of stage II skin injuries have fallen from 0.42 per 100 of CPAP days in the first quarter of 2019 to less than 0.2 per 100 of CPAP days in the first quarter of 2020. All stage II injuries resolved with no sequelae. There were no cases of stage III nasal injuries. Rates of CLD have also fallen from 30%-40% in 2017-2018 before the audit program to ≤ 8% and after the audit program initiation. The goal is to be less than 10%
While not every case of CLD is caused by failure of CPAP administration, making sure a nasal injury doesn’t hamper a baby’s journey to breathing independently is a critical goal. “We want to help them on their way to going home, so that new families start their lives together,” Dr. Aly concludes.
Advertisement
Advertisement
Life-changing gene therapy is currently under FDA review
How evolving medical therapies and more precise patient selection are reshaping the role of intestinal transplantation
Cleveland Clinic specialist discusses the new clinical practice guideline
Introducing Prajwal Rajappa, MD, MS, Director of Pediatric Precision Oncology
The one-stop THRIVE clinic addresses renal, psychosocial, educational and other challenges alongside cardiac surveillance
Study found lower rates of nausea, vomiting and healthcare use through 12 months of follow-up
What to know about the condition, and 5 strategies to improve patient care
Biologic therapy and advances in monitoring may ease treatment and follow-up for families