How our first century has impacted cardiovascular practice
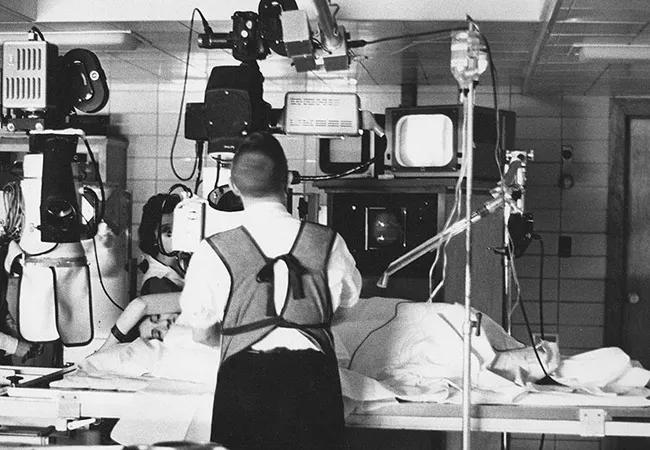
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/019a0b9c-1657-4a8a-883f-c77fec3922bb/20-HVI-2034261_early-coronary-angiography_650x450_jpg)
20-HVI-2034261_early-coronary-angiography_650x450
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
One hundred years ago this month, Cleveland Clinic was founded as a group practice — a novel concept at the time — by four Ohio physicians. Their aim was to deliver healthcare modeled on the team-based approach to care they had experienced as part of military medical units during World War I.
Their mission has endured for a century now, transforming the modest practice they started in 1921 into one of the world’s great medical centers. In no realm has that mission proved as fruitful as it has in cardiovascular care.
Although Cleveland Clinic was not known for particular expertise in cardiovascular care during its first few decades, that began to change with the landmark development of coronary angiography by cardiologist F. Mason Sones, MD, in 1958. This and Sones’ subsequent pioneering work here in cardiac catheterization paved the way for many of the advancements in myocardial revascularization that followed in the next two decades.
Chief among them was the development of coronary artery bypass grafting (CABG) as a planned, consistent approach to the treatment of coronary artery disease. That effort was led by Cleveland Clinic cardiac surgeon Rene Favoloro, MD, who in 1967 completed the first successful attempt at coronary vein grafting with an interposed saphenous vein graft. By the early 1970s, Cleveland Clinic surgeons led by Floyd Loop, MD, standardized the use of internal thoracic artery (ITA) grafts in CABG, ultimately establishing ITA grafting as the standard of care in a landmark 1986 New England Journal of Medicine study.
Advertisement
The impact of the rise of CABG on all of U.S. healthcare is hard to overstate. Together with the creation of Medicare a few years earlier, it fueled explosive growth in hospitals in the last few decades of the 20th century, creating the infrastructure of modern U.S. healthcare.
CABG was also the first treatment that served to draw large numbers of international patients to Cleveland Clinic. Soon the health system’s reputation for unparalleled expertise expanded to other cardiovascular services, making Cleveland Clinic a destination for complex patients and setting the stage for its run as a top-ranked U.S. center for cardiology and heart surgery by U.S. News & World Report.
Other innovations contributed to that status, from early development of stopped-heart surgery by Donald Effler, MD, in the mid-1950s, to creation of the world’s first computerized data registry for cardiac diagnosis and treatment in 1972, to the first minimally invasive mitral valve operations led by Toby Cosgrove, MD, in the mid-1990s, among others. Cleveland Clinic surgeons and cardiologists also played pioneering roles in the development of everything from heart transplantation to intravascular ultrasound to transcatheter aortic valve replacement.
The reputation built by these advancements has made cardiovascular services singularly essential to Cleveland Clinic’s success and growth over its first century. At the same time, our Miller Family Heart, Vascular & Thoracic Institute could not have achieved what it has without the excellence, support and multidisciplinary collaboration of the overall Cleveland Clinic enterprise. That enterprise has been guided at every turn by the mission of the four Cleveland Clinic founders: caring for life, researching for health and educating those who serve.
Advertisement
This three-part mission will remain the light that guides us into Cleveland Clinic’s second century, as providers everywhere grapple with growing case complexity and demands for greater efficiency as healthcare financing further evolves. Our Heart, Vascular & Thoracic Institute will continue its tradition of adaptation and innovation to meet new patient needs, conduct practice-shaping investigations and train tomorrow’s master clinicians — all in the service of high-value care with untouchable patient outcomes. We thank you for your enduring confidence and collaboration.
Dr. Svensson, a cardiothoracic surgeon, is Chair of Cleveland Clinic’s Sydell and Arnold Miller Family Heart, Vascular & Thoracic Institute.
Advertisement
Advertisement
Post hoc analysis of CLEAR Outcomes trial bolsters its case as a statin alternative
Large retrospective analysis may prompt prospective studies
How to talk about lifetime risk, treatment goals, Lp(a) testing, statin skepticism and more
A scannable recap of recent volumes and clinical metrics from Cleveland Clinic
Cleveland Clinic reports first U.S. series focused on use in this challenging setting
Large series confirms early and long-term survival advantages over partial pericardial resection
AVANT GUARD trial extends first-line role for ablation beyond paroxysmal atrial fibrillation
Maintain a high index of clinical suspicion and consider the underlying etiology