JACC review makes the case and outlines how to ensure oversight
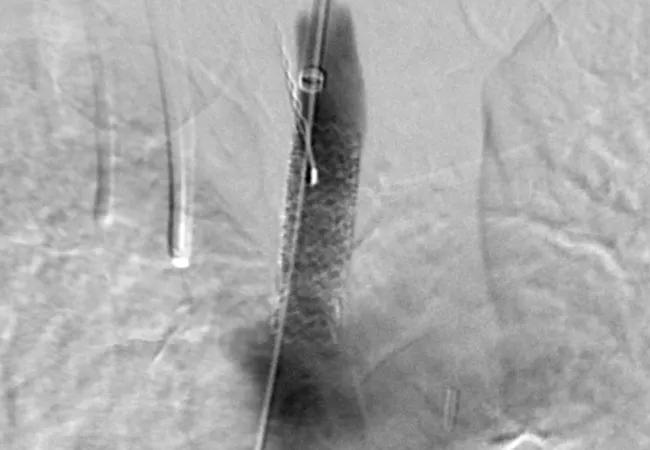
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c911ea74-37e6-4dc3-af16-a224f2ffd097/20-HVI-1868665-carotid-artery-stenting_jpg)
20-HVI-1868665-carotid-artery-stenting
Current evidence supports Centers for Medicare & Medicaid Services (CMS) reimbursement for endovascular treatment of asymptomatic carotid artery stenosis in appropriate patients if it can be regulated through standardized training, data collection and reporting. So contends a multicenter group of cardiovascular clinicians in a recent review in the Journal of the American College of Cardiology featured as a “JACC review topic of the week.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Carotid artery stenting in asymptomatic patients is probably the most extensively studied vascular procedure that has not yet gained coverage status in the United States,” says review co-author Sean Lyden, MD, Chair of Vascular Surgery at Cleveland Clinic. “Over the past several years, significant new data have emerged on endovascular therapy in this population. We developed this review to summarize the state of carotid artery stenting in this setting and offer recommendations on next steps for its application and coverage in patient care.”
The authors supplement their coverage recommendation by suggesting three methods of ensuring that carotid artery stenting (CAS) is appropriately provided to asymptomatic patients by a properly prepared workforce:
“Participation in such a registry could be linked to reimbursement, much like what is now done for coronary artery bypass grafting and other procedures,” observes Dr. Lyden.
Advertisement
The authors support their endorsement with a review of the evolution of CAS in recent years. Points they touch upon include the following:
Advertisement
“Asymptomatic internal carotid artery stenosis is likely to loom ever larger as a contributor to stroke as the U.S. population continues to age,” notes Cleveland Clinic interventional cardiologist Christopher Bajzer, MD, who was not involved in writing the JACC review. “These authors are to be commended for endorsing CMS coverage of carotid artery stenting as an additional option we can turn to in appropriate cases of significant asymptomatic stenosis. As the tools for stenting in this setting continue to become safer, limiting access to these tools becomes less defensible.”
The full review is available here.
Advertisement
Advertisement
Large retrospective analysis may prompt prospective studies
How to talk about lifetime risk, treatment goals, Lp(a) testing, statin skepticism and more
A scannable recap of recent volumes and clinical metrics from Cleveland Clinic
Cleveland Clinic reports first U.S. series focused on use in this challenging setting
Large series confirms early and long-term survival advantages over partial pericardial resection
AVANT GUARD trial extends first-line role for ablation beyond paroxysmal atrial fibrillation
Maintain a high index of clinical suspicion and consider the underlying etiology
Protocol adoption at Cleveland Clinic sharply raised share of transferred patients getting timely PCI