Patient age and baseline platelet count are considerable influences

Although platelet-rich plasma (PRP) is becoming more common in the treatment of osteoarthritis, soft tissue injuries, tendinopathies and muscle tears, it needs more development and optimization, says Nicolas S. Piuzzi, MD, Director of Cleveland Clinic Adult Reconstruction Research.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
One of the biggest challenges in using PRP is that its composition usually is not known or not reported, he notes.
“If you don’t know the composition of what you injected, it’s hard to assess why it worked or why it failed,” says Dr. Piuzzi.
At the Hospital Italiano de Buenos Aires in Argentina, measuring the baseline composition of PRP for each patient is standard of care. As such, Dr. Piuzzi collaborated with Luciano Rossi, MD, PhD, and other researchers at Hospital Italiano de Buenos Aires to analyze the center’s patient database, attempting to better understand relationships between demographic factors and PRP. The resulting study was published in Arthroscopy, Sports Medicine, and Rehabilitation.
“The goal of this study was to shed more light on the use of PRP and how it varies by the patient and numerous factors,” says Dr. Piuzzi. “This study is a step toward developing a more consistent, reproducible technique to improve how we provide PRP to patients.”
The researchers identified 357 patients treated with 403 PRP injections between January 2019 and December 2021 and evaluated the effects of age, sex, body mass index (BMI) and baseline blood count on PRP composition. They also looked at the variability of PRP composition in patients who received two PRP treatments at separate times.
The study’s key finding was that PRP composition varies considerably.
“It varies between patients and even within the same patient,” says Dr. Piuzzi. “The final concentration of platelets varies significantly depending on when it is prepared. Variation is not always a bad thing, but it’s something to acknowledge, and it’s something that we need to bring into the workflow.”
Advertisement
The greatest influences on final PRP composition were age and baseline platelet count, according to the study. BMI, sex and the remaining components of the baseline blood count (erythrocyte count, hematocrit, hemoglobin level, mean corpuscular volume and leukocyte formula) did not significantly affect final PRP composition.
Patients older than age 60 had the lowest number of platelets. Patients younger than age 40 had the highest number.
“For each decade that a patient aged, there was a decrease of approximately 33,000 platelets,” says Dr. Piuzzi.
Additionally, the PRP platelet count increased almost fourfold for each unit increase in baseline blood platelet count, he notes. Compared with women, men had a lower PRP platelet count, but it wasn’t a significant difference.
“Knowing we have all these variations, even if you had a patient who had a good outcome with PRP at one point, you would need to know the number of platelets and the preparation protocol used so you could attempt to replicate the outcome with a subsequent treatment,” says Dr. Piuzzi.
Of the 357 patients in the study, 34 received a second dose of PRP 15 days after the first injection. These doses showed substantial differences in mean number of platelets, with nearly 40% more platelets in the second treatment (890,018 vs. 1,244,467).
“PRP treatments at different times could yield different results, not only because of the condition being treated but also because of a difference in PRP composition,” says Dr. Piuzzi.
Though the study’s results were what Dr. Piuzzi and his team expected, “it’s nice to put numbers and hard data to it so that it is something we can build on,” he says. “When applying PRP, we need more data-driven approaches, and we need to measure what we’re doing. Otherwise, we’re just going blindly.”
Advertisement
The study’s results have created a benchmark that Dr. Piuzzi hopes can help develop more quality research.
“The next step is to correlate these findings with clinical outcomes to be able to identify thresholds and quality release criteria,” he says.
Advertisement
Advertisement

A tailored approach combining injections, therapy and preventive care is improving outcomes for patients with elbow OA
Center will coordinate, interpret and archive imaging data for all multicenter trials conducted by the foundation’s Osteoarthritis Clinical Trial Network

Cleveland Clinic radiation oncologists aim to bring the noninvasive approach back to the U.S., where use has declined
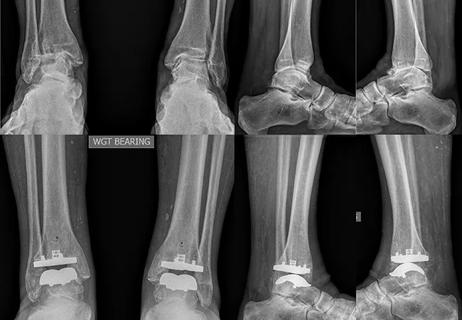
Arthrodesis is not the only surgical option
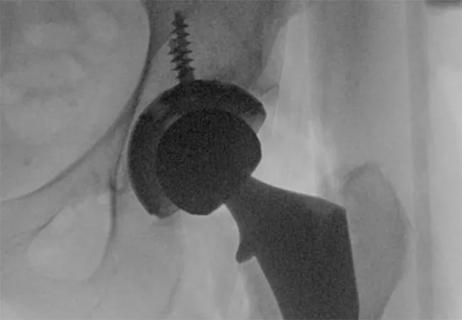
How it actually compares to posterior and lateral approaches

When procedure is performed by high-volume surgeons, outcomes are comparable to total knee replacement
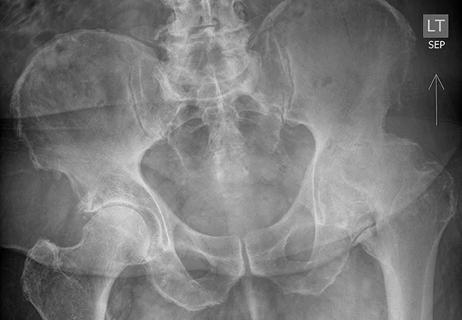
Offers adequate exposure of normal and abnormal anatomy
New program bridges orthopaedics and endocrinology