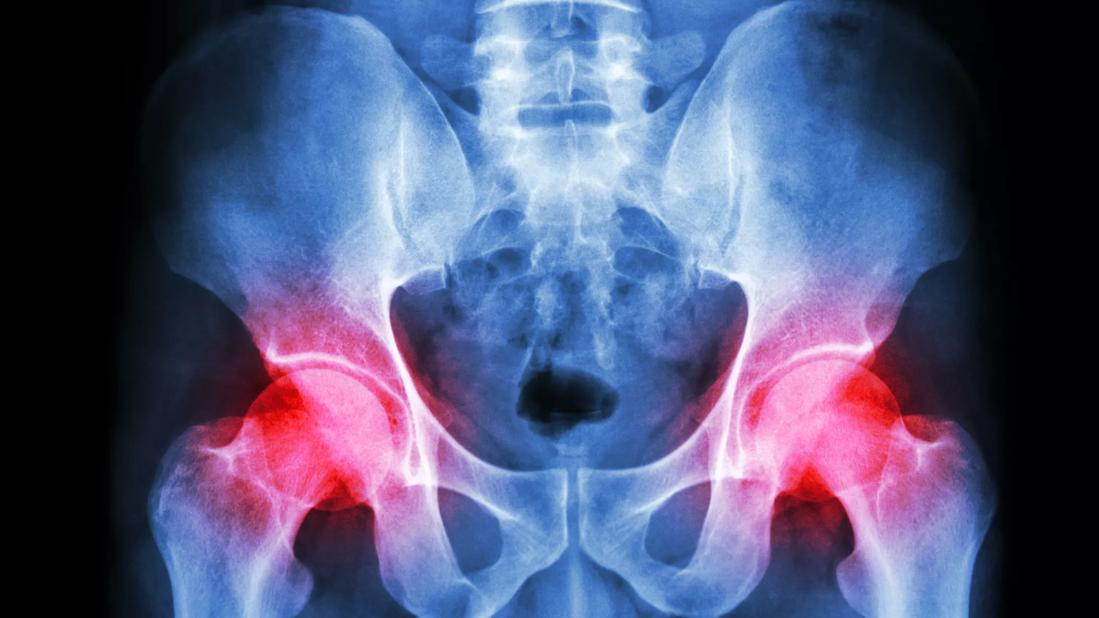
Hip abductor tendinopathy is a common cause of lateral hip pain, one that is often misdiagnosed and mismanaged, according to Michael Dakkak, DO, a fellowship-trained sports medicine physician with Cleveland Clinic Weston Hospital.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“There is a growing array of ultrasound-guided, nonsurgical treatment options for hip abductor tendinopathy, but many eligible patients will not have access to them without an accurate diagnosis,” says Dr. Dakkak.
The multitude of lateral hip pain etiologies and their coexistence can make diagnosing these conditions challenging. These include hip osteoarthritis, radiating pain from lumbar spine stenosis, trochanteric bursitis, and external coxa saltans (snapping hip syndrome), among others. Most common, however, are abductor tendon lesions and insertional tendinopathy involving the gluteus medius, gluteus minimus and tensor fasciae latae.
Tendinopathy encompasses both tendinitis, the inflammation of a tendon, and tendinosis, the degeneration of collagen fibers in a tendon. Initial treatment of these tendon pathologies may include non-steroidal anti-inflammatory medications, activity modification, physical therapy, and corticosteroid injections.
“Unfortunately, patients presenting with hip pain often receive a differential diagnosis that can result in a case of tendinosis being treated as tendinitis, which may result in suboptimal outcomes with conservative management alone,” cautions Dr. Dakkak.
Following a detailed patient history and physical examination, imaging is the next step in the clinical evaluation of patients with hip pain. Radiography is first used to rule out osteoarthritis and other bone-related conditions, while an MRI is diagnostic for identifying abductor tendon tears. The latter is typically only pursued following a course of conservative treatment.
Advertisement
Researchers with Cleveland Clinic’s Sports Medicine Center in Ohio recently completed research on the reliability of musculoskeletal ultrasound for classifying tendinopathies as inflammatory, degenerative, and inflammatory on degenerative.
“Today musculoskeletal ultrasound is an essential tool for diagnosing tendinopathies as it can be used to identify disorganized and misaligned tendon fibers and tears that may benefit from advanced nonsurgical treatments,” says Dr. Dakkak, who participated in tendinopathy research as a sports medicine fellow at Cleveland Clinic under the mentorship of Jason Genin, DO, a medical orthopedics and sports medicine physician with Cleveland Clinic’s Orthopaedic and Rheumatologic Institute.
Once an accurate tendinopathy diagnosis is made, musculoskeletal ultrasound is also used to deliver therapeutic injections and minimally invasive treatments. “For inflammatory tendinopathy, we use ultrasound-guidance to ensure accuracy and precision of percutaneous corticosteroid injections adjacent and superficial to the affected tendon,” says Dr. Dakkak, noting this approach is not appropriate when degenerative tendinopathy is present.
In cases of tendinosis, he employs other ultrasound-guided, needle-based procedures to promote good inflammation and remove degenerative tissue. These include platelet-rich plasma (PRP) therapy, bone marrow aspirate concentrate (BMAC) injections, and minimally invasive tenotomy. Dr. Dakkak is also the first sports medicine specialist in Florida to use a newly patented device for the removal of diseased tendon tissue that leaves healthy tissue intact.
Advertisement
“The image-guided hydroresection procedure uses a dual-lumen, 12-gauge needle to administer 14,000 psi of saline to break up and simultaneously aspirate the tendinopathic tissue,” explains Dr. Dakkak. “It requires just a small incision and no stitches or use of crutches following the procedure.”
Patients then undergo 6 to 8 weeks of physical therapy to optimize tensile capacity of the tendon, strengthen supporting muscles, and restore joint function, he adds.
Advertisement
Advertisement

Nonthermal technique reduces bleeding and perforation risk

Standardizing a minimally invasive approach for Barrett’s Esophagus and Esophageal Cancer

PSMA-targeted therapy for metastatic prostate cancer now offered at Cleveland Clinic Weston Hospital

Nationally recognized urologic oncologist offers vision for growth, innovation, and excellence

Noninvasive modality gains ground in United States for patients with early-to-moderate disease

Cleveland Clinic Weston Hospital’s collaborative model elevates care for complex lung diseases

Interventional pulmonologists at Cleveland Clinic Indian River Hospital use robotic technology to reach small peripheral lung nodules

Trained in the use of multiple focal therapies for prostate cancer, Dr. Jamil Syed recommends HIFU for certain patients with intermediate-risk prostate cancer, especially individuals with small, well-defined tumors localized to the lateral and posterior regions of the gland.