Screening asymptomatic high-risk patients is key
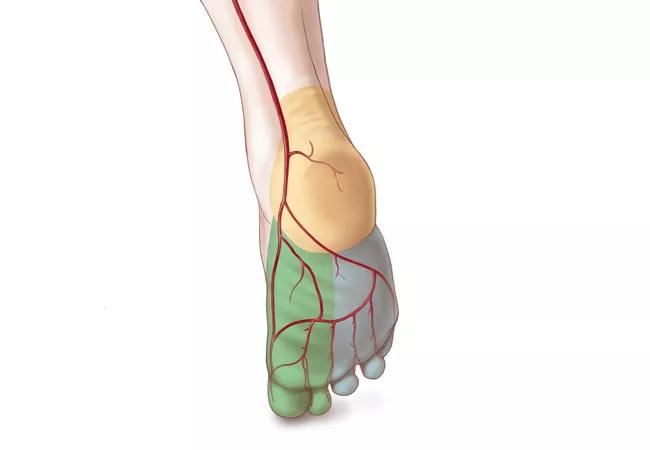
Most physicians are able to diagnose peripheral arterial disease (PAD) in the presence of critical limb ischemia, but many don’t look for PAD in asymptomatic patients, even those at high risk for the disease. That’s a dangerous oversight, say Cleveland Clinic vascular medicine specialists.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Two-thirds of PAD patients also have coronary artery disease or cerebrovascular disease. It’s not uncommon for PAD to be the first presentation of cardiovascular disease (CVD),” says Joseph Campbell, MD, a physician in Cleveland Clinic’s Section of Vascular Medicine and Section of Invasive and Interventional Cardiology.
“Early identification of these patients is critical,” he adds, “as it allows for prompt initiation of treatment aimed at reducing the incidence of long-term cardiovascular and limb events.”
Treatment may consist of initiating aspirin, high-intensity statin therapy and other medications as needed, such as antihypertension and antidiabetes agents. Patients should also be counseled on smoking cessation and other lifestyle factors.
“When initiated early in the disease course, these interventions may save a limb and prevent a heart attack or stroke down the road,” says Dr. Campbell.
PAD may not be on a physician’s radar when the patient is asymptomatic or has an atypical symptom, such as leg fatigue. This can lead to the underdiagnosis of PAD, as a high proportion of patients present in this manner.
Dr. Campbell advises physicians to be alert for changes in functional status as well. “Individuals with PAD may not be functioning as well as age-matched peers,” he says. “They may have slowed down or become more sedentary.”
Identifying patients at high risk for PAD on the basis of risk factors — including older age (≥ 65), diabetes in younger patients, hypertension, dyslipidemia, history of smoking, history of atherosclerotic disease in other vascular beds or family history of PAD — should prompt physicians to consider screening for PAD.
Advertisement
“Personally, I think all patients with risk factors for PAD should have a thorough vascular exam, whether they are symptomatic or not,” says Dr. Campbell. He notes that the exam should include palpation of lower extremity pulses, auscultation for femoral bruits, inspection of the feet and measurement of bilateral blood pressures. “Screening in an accredited vascular lab starting with an ankle-brachial index (ABI) can then be done in patients who have an abnormal exam or are considered at high risk for PAD,” he adds.
Similarly, patients diagnosed with any form of CVD are at high risk for PAD. Fortunately, placing these patients on appropriate medications and lifestyle changes can often prevent a cardiac or cerebrovascular event. “The goal is less to encourage intervention than to make sure we do everything possible to ensure these patients are reducing their risk factors to lower their global cardiovascular burden,” he says.
While the ABI is the accepted screening modality for PAD, Dr. Campbell cautions that results may be misleading: “Thirty percent of ABI results in the presence of critical limb ischemia will be normal or near-normal. For this reason, high-risk patients should be referred to a vascular specialist for a more detailed exam.”
He points out that screenings done in a vascular lab are more reliable. “We use other measures, including toe-brachial index and evaluation of arterial waveforms,” he says. “Nuances in these tests may help us achieve an accurate diagnosis.”
Any patient with abnormal noninvasive test results or tissue loss, regardless of symptomatic status, should be referred to a vascular specialist for prompt initiation of interventions aimed at reducing morbidity and mortality.
Advertisement
Dr. Campbell notes that while vascular medicine physicians are the ideal specialists to diagnose and manage PAD patients, the complex nature of the disease generally calls for a team of physicians to ensure appropriate care. Such a team may include cardiologists, vascular surgeons, podiatrists, endocrinologists, wound-care specialists, infectious disease specialists and nephrologists.
“The point is that treating PAD is not a one-man show,” he explains. “These patients have multiple comorbidities that cannot be effectively managed in a 10- to 15-minute office visit.”
Dr. Campbell invites primary care physicians and specialists alike to reach out for advice in managing these patients. “When in doubt, pick up the phone and express your concerns,” he advises. “I would rather have someone call me to be reassured they are doing the right thing than miss an early diagnosis and opportunity to help a patient.”
Dr. Campbell can be reached at 216.444.9836.
Advertisement
Advertisement

Emerging evidence suggests a patient-specific approach

Not if they meet at least one criterion for presumptive evidence of immunity

Essential prescribing tips for patients with sulfonamide allergies

Confounding symptoms and a complex medical history prove diagnostically challenging

An updated review of risk factors, management and treatment considerations
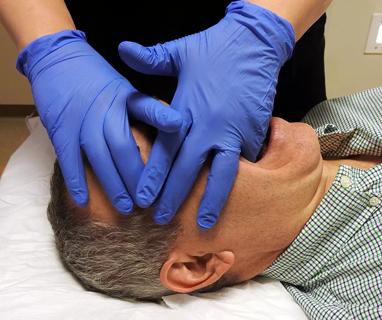
OMT may be right for some with Graves’ eye disease

Perserverance may depend on several specifics, including medication type, insurance coverage and medium-term weight loss

Abstinence from combustibles, dependence on vaping