A discussion with Laurence Kennedy, MD, FRCP
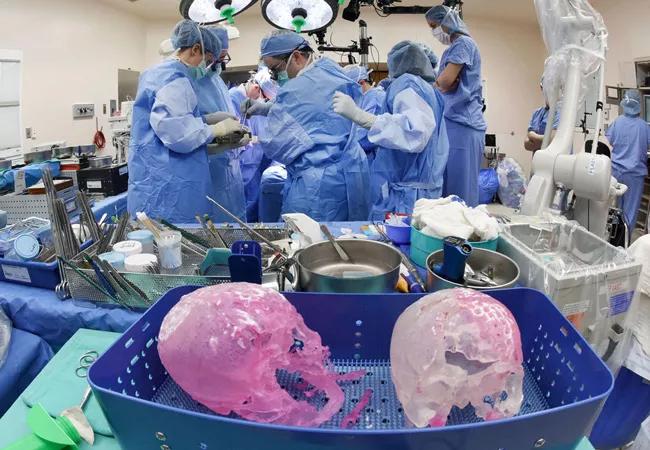
The recovery of Katie Stubblefield, a young woman who received a total face transplant at Cleveland Clinic in May 2017, continues to intrigue the medical community. Transplanted at age 21, Katie became the world’s youngest face transplant recipient.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The procedure, which took 31 hours, required detailed planning and cooperation of a large team of Cleveland Clinic experts that included surgeons, endocrinologists, anesthesiologists, ophthalmologists, psychiatrists, infectious disease specialists, dentists, physical, occupational and speech therapists, and nurses.
Laurence (Ned) Kennedy, MD, FRCP, Chairman of Cleveland Clinic’s Endocrinology, Diabetes, and Metabolism Department oversaw Katie’s endocrinological care during her stay at the clinic. In this Consult QD article, he discusses the challenges his endocrinology team faced before and after the procedure.
“When Katie was transferred to Cleveland Clinic she was already receiving high doses of steroids, which makes it difficult to assess pituitary gland function,” he says. “We were told that the injury had damaged her pituitary gland and that her thirst mechanism was impaired, so we had to work on the assumption that she had no pituitary function. Therefore, she was treated with hydrocortisone, levothyroxine and desmopressin.”
Dr. Kennedy explains that patients who lack a normal thirst mechanism and are passing large amounts of urine, like Katie, are at risk of having abnormal serum sodium levels. Therefore, their sodium levels need to be closely monitored to prevent overtreatment or undertreatment with a synthetic antidiuretic hormone — desmopressin (DDAVP).
“In the many months leading up to the surgery, Katie was treated with DDAVP,” says Dr. Kennedy. Throughout that time, his team relied “on a great deal of cooperation and care from her parents who assisted with close monitoring of serum sodium levels.”
Advertisement
The next challenge in Katie’s care was managing diabetes insipidus and her fluids during the surgical procedure, which took 31 hours.
“If diabetes insipidus is not recognized and adequately dealt with, the patient is in grave danger of getting severe electrolyte abnormalities, either excessive hypernatremia or severe hyponatremia,” says Dr. Kennedy, emphasizing that the main credit for Katie’s endocrinological management during surgery goes to Dr. Khawla Ali, an endocrine fellow at Cleveland Clinic.
“Dr. Ali and my younger colleagues spent several weeks researching the literature to devise a treatment regimen that would ensure that Katie’s fluid and electrolyte balances remained stable throughout the surgery,” he says. “This entailed treatment with antidiuretic hormone and frequent monitoring of serum sodium levels. Dr. Ali was in the operating room throughout the procedure and served as the ever-present source of knowledge for the surgeons.”
Dr. Kennedy explains that Katie’s current postoperative endocrinological care entails regular follow-up visits at the clinic where the functioning of her pituitary and thyroid glands is monitored.
“She is still receiving thyroid hormone, steroids in the form of prednisone and DDAVP,” he says. “Steroids will be needed in the long-term, while DDAVP will be continued as long as we suspect she has diabetes insipidus. There have been recent signs that some pituitary function may be returning, so although she is also receiving thyroid hormone we are keeping the situation under review.”
Advertisement
With Katie out of the clinic and doing well, Dr. Kennedy reflects on the importance of teamwork and planning in managing complex cases such as hers.
“The planning for surgery took many months, with input from a team of specialists formed by Brian Gastman, MD, upon Katie’s arrival to the clinic.”
According to Dr. Kennedy, the length of Katie’s stay at the clinic and the unpredictable nature of some of the crises that arose during that time, required tight cooperation within his team of endocrinologists as well as between his team and the other specialists involved in her care.
“It was simply impossible for one endocrinologist to be responsible for all of her care, so many of my colleagues touched her care at one time or another. We were all aware of the complexity of Katie’s case and I am very proud of the teamwork within our department that helped to ensure a good outcome,” he concludes.
Advertisement
Advertisement

Pheochromocytoma case underscores the value in considering atypical presentations

Advocacy group underscores need for multidisciplinary expertise

A reconcilable divorce

A review of the latest evidence about purported side effects

High-volume surgery center can make a difference

Advancements in equipment and technology drive the use of HCL therapy for pregnant women with T1D

Patients spent less time in the hospital and no tumors were missed

A new study shows that an AI-enabled bundled system of sensors and coaching reduced A1C with fewer medications