Bridge to transplant after acetaminophen overdose
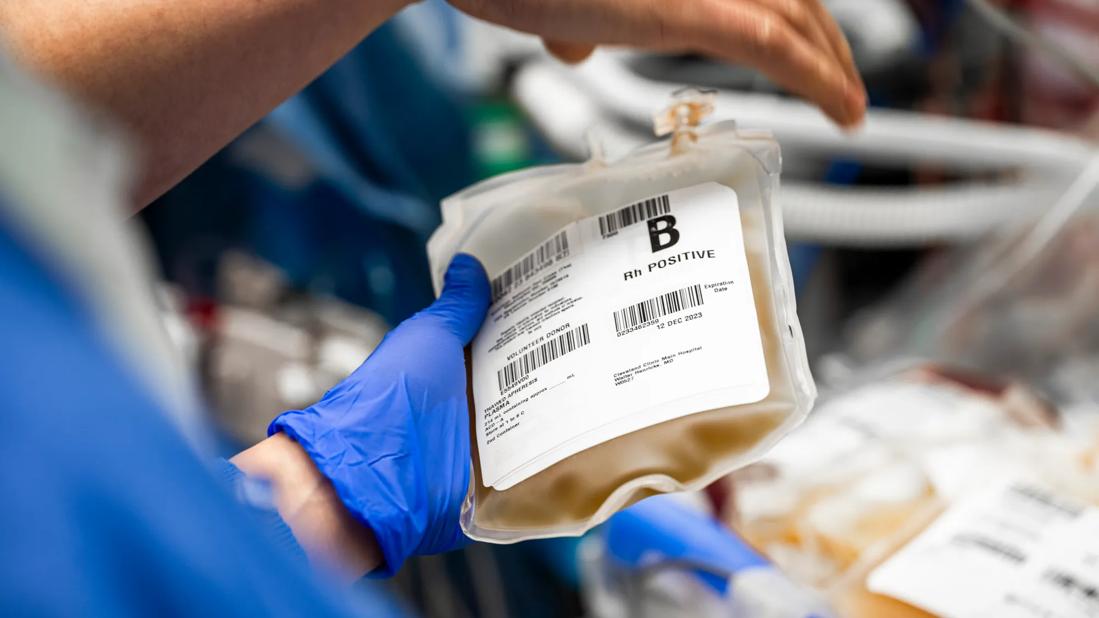
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/78fce8f4-e571-4cb9-95f8-80d8427201af/CCC_4470815_12-08-23_353_MLC-jpg)
650×450-Plasma
In June 2020, a 27-year-old woman developed a case of COVID-19; her main symptoms were stomach pain, nausea and diarrhea. To relieve the pain, she took so much acetaminophen that she had an overdose and developed fulminant liver failure.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
She was gravely ill and hospitalized at Cleveland Clinic in the COVID ICU. She was intubated and treated for symptoms of liver failure, which included cerebral edema.
To normalize her blood pressure, she was treated with high-dose vasopressors. The liver failure also caused a cytokine storm, which stressed her heart and kidneys. She was in need of a liver transplant but was considered too high risk. “Every moment, she was getting worse and further from being able to get a liver transplant,” says Kristin Ricci, MD, a transfusion medicine specialist and Medical Director of the apheresis unit at Cleveland Clinic.
Cleveland Clinic is one of only a few medical centers worldwide able to perform high-volume plasma exchange. During the procedure, a patient’s plasma is removed with an apheresis instrument and is replaced with plasma from healthy donors. Unlike standard plasma exchange treatments, which treat a patient’s plasma once, high-volume plasma exchange treats it three to four times. This patient was the first at Cleveland Clinic treated with this approach; the goal was to stabilize her health so she could get a transplant.
The procedure was a team effort involving intensive care, hepatology, anesthesiology, liver transplant, nursing, apheresis, laboratory medicine and blood bank teams. “High-volume plasma exchange requires great resources and coordination. Many different groups used their strengths to save this patient’s life — Cleveland Clinic culture at its best,” says Dr. Ricci.
Advertisement
After the procedure, the patient became more hemodynamically stable, her vasopressor requirements decreased and many of her liver labs normalized. The procedure also removes inflammatory cytokines, so the storm subsided. Because of these major improvements, the patient was listed for a liver transplant.
The liver transplant team, led by Giuseppe D’Amico, MD, and Jacek Cywinski, MD, was ready to perform the transplant. The next day, the patient received a second high-volume plasma exchange which showed continued improvement in clinical status and labs. The transplant was performed that evening by a team that included more than 40 caregivers.
The patient had an uneventful recovery and has been discharged home and is doing well. “The high-volume plasma exchange was a game changer that saved her life. This technique completely changed the management strategy for this patient. We are excited about starting a program to use high-volume plasma exchange for acute liver failure,” says Cristiano Quintini, MD, Program Director and Surgical Director of the Liver Transplantation Program.
Advertisement
Advertisement
Reframing cancer survivorship
New guidelines empower clinicians with practical diagnostic framework
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation