New tools, education and communication achieve goal
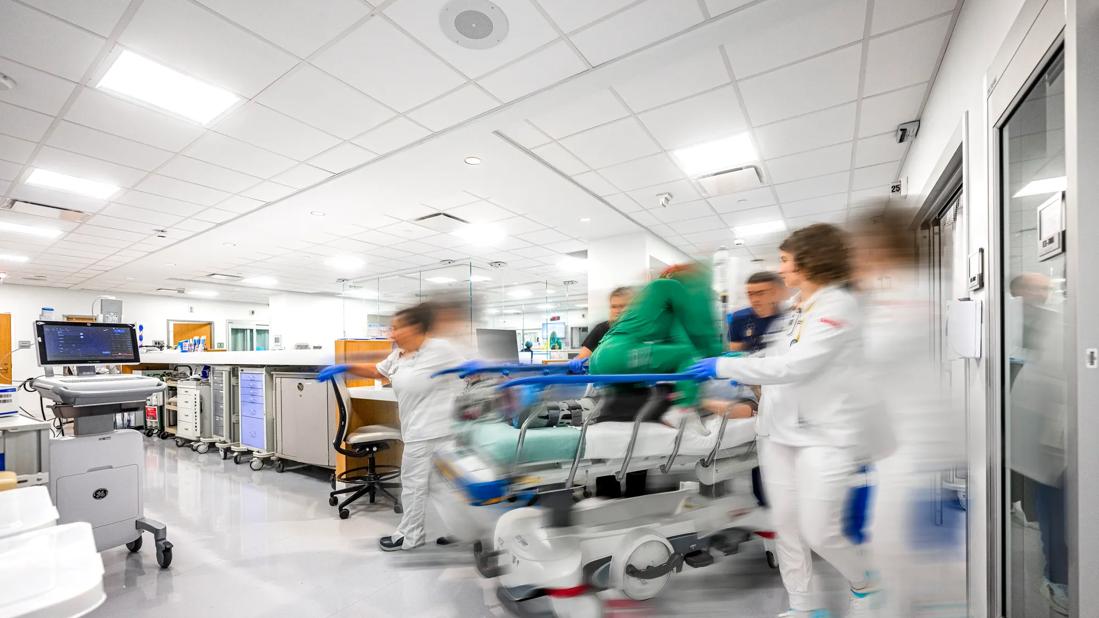
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c62e0196-dfd9-4f3f-ad12-e8224fac3043/PHI_6281008_06-09-25_070_MLC_3)
CPR
In-hospital cardiopulmonary arrests (CPA) are a public health concern nationwide, with approximately 292,000 adult CPAs in the United States each year, according to a study in the American Heart Association’s Circulation journal. During the third quarter of 2019, the rate of in-hospital cardiopulmonary arrests (CPA) at Cleveland Clinic South Pointe Hospital was 4.89 per 1,000 patient days. The hospital’s interdisciplinary Code Blue Committee, which includes several nurses, reviewed the summary report of all CPAs.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“We realized that we called more code blues than rapid responses, and there were a lot of codes with initial rhythm as pulseless electrical activity,” says Nancy Hodge, MSN, RN, assistant nurse manager of the ICU and a member of the Code Blue Committee. “How could we prevent this from happening?”
The committee devised a multipronged approach to decrease the rate of in-hospital cardiopulmonary arrests, which featured the following:
The new one-page debriefing tool captures all the information required for reporting in the database for code blue reviews. Caregivers indicate whether they called a code blue, rapid response or concurrent event, and whether it was documented in the safety event reporting system. The tool also includes information on airway access, vascular access and chest compressions. “We check off items to see what we missed or could have done better, as well as what we did great,” says Hodge.
Advertisement
In addition, the committee created green labels identifying each role – code supervisor, CPR and medication nurse – that caregivers assume when they enter the room. This helps ensure that everyone in the crowded room knows their job and the role of others.
Advertisement
L – Give the Location of the event
E – Specify whether the Event is a code blue or rapid response
A – Indicate if the patient is an Adult or child
N – Provide a Number to call back
After implementing these strategies, the in-hospital CPA rate at South Pointe Hospital decreased to 3.29 per 1,000 patient days during the third quarter of 2020 and 2.19 during the fourth quarter. The Code Blue Committee continues to review all codes and look for opportunities for improvement. Hodge and Eklich also continue to educate nurses, making presentations to newly hired nurses and the New Graduate Council.
Advertisement
Advertisement
Program helps caregivers prepare for the unique pressures of the ICU
Multidisciplinary simulations provide realistic emergency training to help achieve optimal patient outcomes
How critical care expertise, rapid decision-making and patient advocacy are shaping perioperative care
Survey identifies opportunities for further training and ongoing moral support
Nursing quality experts help drive policies and practices designed to meet the highest clinical standards
Innovative workforce strategy transforms nursing careers through education, flexibility and ongoing support
Caregivers reflect on shared purpose, evolving practice and the enduring heart of the nursing profession
Nurse manager turns a patient safety concern into a data-driven effort to improve protocols and inspire innovation