Cleveland Clinic takes an integrated approach to formulary management

An active and engaged pharmacy and therapeutics (P&T) committee is a crucial component of any hospital or multihospital health system.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It serves as a forum for reviewing and selecting medications for a hospital or health system’s formulary, which defines what medications can be used by its clinical practitioners and outlines medication use policies. The P&T committee makes evidence-based decisions that support the goal of providing optimal patient care while minimizing risks and costs to both the system and the patient.
Over the last decade, Cleveland Clinic has strategically restructured its P&T and formulary management process. Previously, individual P&T committees existed at each hospital within the system and made decisions regarding their own formularies. In 2010, it implemented one unified formulary and one medical staff P&T committee to have authority over formulary decisions for the whole system.
In addition to a main campus, the Cleveland Clinic health system (CCHS) today comprises 11 regional hospitals and employs more than 3,900 physicians. Having one standardized formulary that applies to all of them is helpful from both a patient safety and a healthcare professional engagement standpoint, says Drug Use Policy and Formulary Management Director Mandy Leonard, Pharm.D, BCPS.
“When you have physicians and nurses and pharmacists rotating within the system, there’s less confusion if it’s standardized,” she says. “We should be able to take care of patients the same way whether they’re at main campus or a regional hospital.”
It also presents the opportunity for a health system to implement cost savings initiatives across the board, such as transitioning some brand-name medications to generics, converting to alternative therapies and removing certain medication from the formulary.
Advertisement
Implementation of a unified system also streamlined the creation of drug records in Cleveland Clinic’s electronic health record and standardized dosing, administration and concentrations.
A priority when developing the new committee structure was making sure that the needs of both the health system as a whole as well as its individual hospitals were considered in the P&T process. This was necessary to ensure that formulary decisions would be widely accepted once they were made.
Dr. Leonard and other contributors outlined this process, as well as learnings from creating a multihospital P&T committee, in a 2018 paper published in the American Journal of Health-System Pharmacy.
The new process, as detailed in the paper, utilizes a CCHS medical staff P&T committee that makes final decisions, as well as numerous specialty panels that make recommendations to the committee regarding drugs used within their specialties, such as hematology or neuroscience or transplant.
Each specialty panel is co-chaired by one physician from the main campus and one from a regional hospital, and includes additional medical staff and pharmacy specialists in that subspecialty from across the health system.
These panels meet quarterly to review and make recommendations on formulary requests and other medication-related issues. Members of the pharmacy department prepare an evaluation monograph for each drug that includes analysis of its:
Advertisement
The analysis is presented to the appropriate panel, which then makes a recommendation as to whether a drug should be added to the formulary.
“Then, at the end of every quarter, we take all of the recommendations that come from these specialty panels to the larger CCHS medical staff P&T committee,” Dr. Leonard explains.
The chairs of each specialty panel also sit on the medical staff P&T committee, as do P&T committee chairs from each regional hospital. Other members of the committee include the chief pharmacy officer, the medication safety officer, the system director of formulary management and a nursing representative. Members can attended the quarterly meetings in-person or virtually.
The committee votes on whether add each drug to the formulary, reject it or add it with restrictions. The whole process for a drug review takes about three to six months.
Before revising the P&T process a decade ago, Cleveland Clinic conducted a gap analysis of all of the formularies within its system. It found that 80% of line items were the same at main campus and regional hospitals, although there were differences in restrictions among some of the items.
Any major changes to the formulary that were needed to bridge those gaps were spaced out over a period of several years, giving sites a reasonable amount of time to adjust their practices.
Local P&T committees at each hospital are responsible for implementing decisions of the medical staff P&T committee in their facilities. They also perform additional duties such as reviewing medication errors, adverse drug reactions, and policies and procedures.
Advertisement
Individual hospitals’ committees can’t make exceptions to decisions made by the CCHS medical staff P&T committee, but they can add additional restrictions based on their specific needs. For example, a regional hospital could choose not to stock a medication that is added to the formulary because it is not relevant to the patient population served by that hospital.
What has made the integration successful? First of all, “There’s a great relationship between the medical staff and the pharmacists,” Dr. Leonard says. This is key because physicians and pharmacists are at the front lines of upholding changes to the formulary.
It’s also helpful to have an appointed member of the pharmacy department who oversees the P&T process by coordinating and managing formulary requests, reviews, meeting agendas and minutes, and summaries of decisions.
Another consideration is to create a standardized timeline for drug reviews that gives requestors an idea of what to expect, since it may take longer for a health system to review a request than it would for an individual hospital to do so.
“We have about nine years of history now with this process – with new drugs and generic drugs and working as a system – and I’m really proud of that,” Dr. Leonard says. “We can really move things and integrate and standardized things very well.”
Advertisement
Advertisement

Advanced software streamlines charting, supports deeper patient connections

How holding simulations in clinical settings can improve workflow and identify latent operational threats

Interactive Zen Quest experience helps promote relaxing behaviors

Cleveland Clinic and IBM leaders share insights, concerns, optimism about impacts
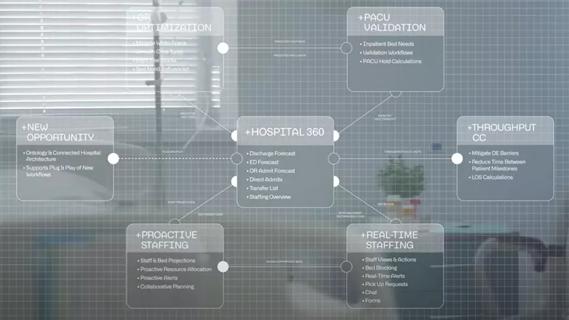
Cleveland Clinic partners with Palantir to create logistical command center

A Q&A with organizational development researcher Gina Thoebes

Cleveland Clinic transformation leader led development of benchmarking tool with NAHQ

Raed Dweik, MD, on change management and the importance of communication