Physicians shares insights about screening, supportive care and potential therapies in development
Lysosomal storage diseases (LSDs) comprise a heterogeneous group of more than 50 rare hereditary disorders that are characterized by enzyme dysregulation. The severity and onset of disease ranges, but lysosomal deficiency in the cellular environment leads to a buildup of substrate in cells, which may result in multiorgan dysfunction and possibly death.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Lysosomes contain digestive enzymes that break down proteins and fats inside cells. “They are the digestive system of our cells,” explains pediatric hematologist-oncologist Rabi Hanna, MD, in an episode of the podcast series Cancer Advances. “If there is a deficiency, a specific substrate accumulates in the different cells, and it can lead to variable manifestations, which can be quite severe.”
Dr. Hanna, who is also Chair of the Department of Pediatric Hematology, Oncology and Bone Marrow Transplantation at Cleveland Clinic Children’s, leads the LSD program along with Angelika Erwin, MD, PhD, a medical geneticist in Cleveland Clinic’s Center for Personalized Genetic Healthcare.
The physicians note that while individual types of LSDs are collectively rare, the overall incidence of LSDs is about 1 in 7,700 births. While there are no curative therapies, for several LSDs, enzyme replacement therapy (ERT) and other treatment modalities can improve patients’ survival and quality of life.
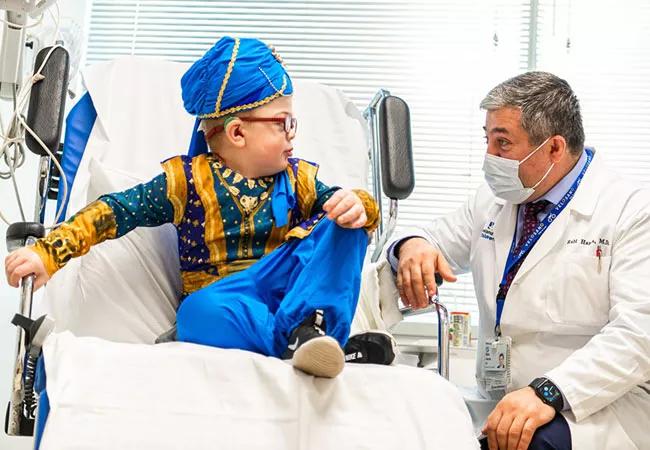
Such is the case for a 6 year old living with Hunter syndrome, also known as mucopolysaccharidosis type II (MPS II), part of the mucopolysaccharidosis disease subgroup of LSD. He has been receiving weekly intravenous ERT since the age of 3 months. While ERT can effectively manage some symptoms in patients with Hunter syndrome, it is not thought to prevent or improve cognitive impairment, because the enzymes do not cross the blood-brain barrier. However, researchers are actively evaluating an approach designed to deliver a manmade enzyme directly to the spinal cord.
Advertisement
A clinical trial led by a team at Ann & Robert H. Lurie Children’s Hospital of Chicago, of which Cleveland Clinic is a participating site, is currently assessing the long-term safety and clinical outcomes of the drug idursulfase, administered monthly via an intrathecal drug delivery device, while patients continue weekly intravenous infusions of the drug.
Though data from the trial have not yet been published, Dr. Hanna says the enrolled patients at Cleveland Clinic – there are two total – are “doing very well.”
In addition to ERT, hematopoietic stem cell transplantation (HSCT) and bone marrow transplantation (BMT) have demonstrated good outcomes for patients, particularly from a cognitive standpoint, when intervention is early. Hematopoietic cells have the ability to produce the enzyme that is deficient in this disorder and prevent further progression. However, in certain types of LSDs where symptom onset may occur later, such as adrenoleukodystrophy, the therapeutic benefit of BMT may be limited.
Additional treatment modalities include substrate reduction therapy and pharmacological chaperones, and there are several more potential therapies currently in development, including:
The physicians are hopeful that earlier screening and risk detection will lead to earlier interventions and better outcomes. Ohio recently joined several other states that include certain LSDs — mucopolysaccharidosis type I (MPS I), Krabbe’s leukodystrophy and glycogen storage disease Type II (Pompe disease) — in newborn screening.
Advertisement
Dr. Erwin sees many patients in her clinic who are suspicious for LSDs following the newborn screening. “We confirm the diagnosis with biochemical and molecular testing and also educate the family about recurrence risk or identify additional family members,” she says in the podcast episode.
“Almost all of those conditions have recessive inheritance. So we don’t often see a family history, but then there are a few that have X-linked inheritance. And so we may detect other family members, either a parent or a sibling, or other family members in those X-linked disorders who also require treatment and medical management.”
The multidisciplinary nature of the disease has led to cross-institute collaborations when it comes to certain disease manifestations.
“Without exception, every single disorder affects multiple different organ systems. And so those patients have a multitude of medical needs and all of them are followed by several subspecialists,” says Dr. Erwin.
She says this connected network takes the burden off the patient to make sure their physicians are on the same page. The team communicates with each other, and also with community providers for patients who aren’t within driving distance to make sure infusion treatments are available to them locally.
Ultimately, because there is no curative treatment for LSDs, Dr. Hanna says their goal is to prevent further pathological damage and provide the best supportive care allowing these patients to develop physically and cognitively. “If the damage is stopped, you can hopefully allow these patients to benefit from physical, speech and occupational therapy, so they can lead their most fulfilling life.”
Advertisement
To listen to the entire interview with Drs. Hanna and Erwin, visit clevelandclinic.org/podcasts/cancer-advances/lysosomal-storage-disease-program.
Advertisement
Advertisement

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes

Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve