An algorithm, expert team and research lead to upgrades
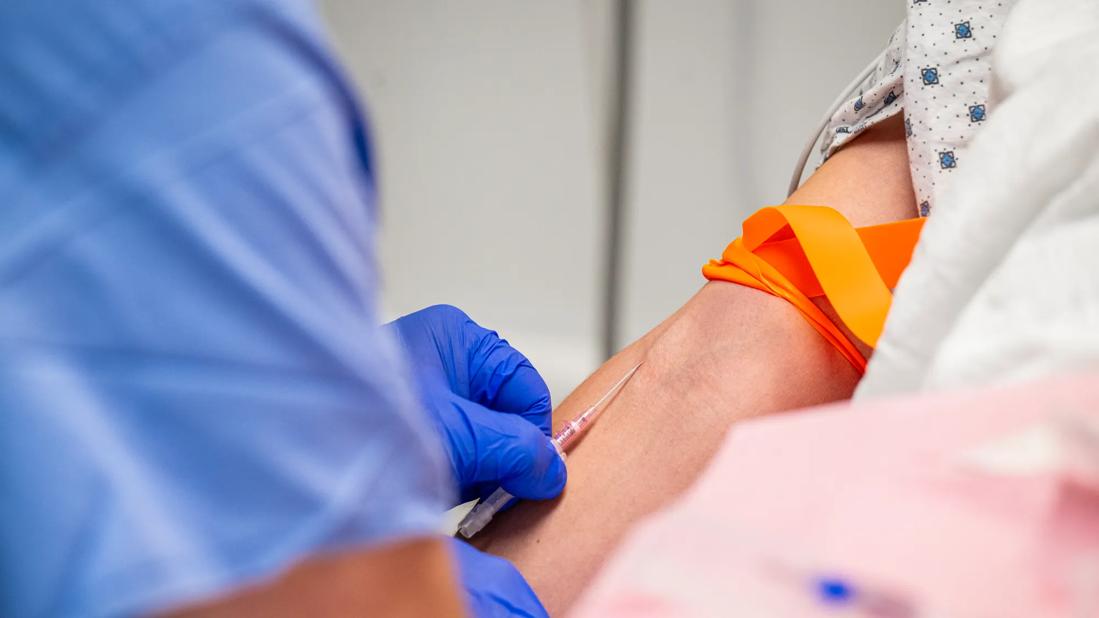
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/43b9c9cf-b85d-4ff2-9bbd-b3a7ff68b45c/CHP_3884959_08-23-23_045_SCG-jpg)
pediatric vascular access algorithm
Evidence-based practice is the bedrock of Cleveland Clinic nursing. One prime example is the healthcare system’s commitment to improving pediatric IV starts, which has evolved over time thanks to the efforts of Jane Hartman, MSN, APRN, PNP-BC.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
When Hartman began working as a clinical nurse specialist at Cleveland Clinic Children’s nearly a decade ago, she developed an algorithm to increase first-attempt IV starts and decrease the overall number of IV attempts. Since then, she has conducted three research studies associated with the algorithm, which have led to improvements in practice and development of a pediatric vascular access team.
Hartman was named the 2021 Janet Pettit Scholar by the Association for Vascular Access (AVA) for scholarly excellence in the field of pediatric vascular access. She will receive the award and make a presentation at the AVA 2021 Annual Scientific Meeting in Orlando, Fla., in mid-September.
Hartman created the Pediatric Peripheral Vascular Access Algorithm (PPVAA) in collaboration with colleague John Baker, DNP, MBA, RN, NEA-BC, now Vice President of Nursing and Operations at Cleveland Clinic Akron General Lodi Hospital. “The algorithm helps people think of vascular access as a process instead of a task,” explained Hartman in a 2016 ConsultQD article on the PPVAA. “It sets you up to do the right thing for both the nurse and patient.”
Hartman then conducted a two-cohort nonequivalent group study to compare differences in IV access before and after implementation of the PPVAA. “We found that it did decrease the number of overall attempts, but it did not significantly increase the number of first-attempt success, which was one of our goals,” she says.
Based on the findings, which were published in the Journal of Pediatric Nursing, Cleveland Clinic Children’s created a pediatric vascular access team in 2015. “We recognized that we needed experts who were certified in vascular access,” says Hartman. She serves as the clinical facilitator for the team, which began with three full-time members with different backgrounds: a pediatric inpatient nurse, a neonatal ICU nurse and an outpatient infusion nurse.
Advertisement
The team members have all earned their Vascular Access Board Certification (VA-BC) and can place peripheral IVs and peripherally inserted central catheter (PICC) lines. “They are a consulting service and the go-to source for pediatric vascular access in the Children’s hospital,” says Hartman.
Once the Pediatric Vascular Access Team was in place, Hartman conducted another research study. “We compared usual care, usual care plus the algorithm and usual care plus the algorithm and the vascular access team,” says Hartman. The results, which were published in January 2020 in the Journal of Pediatric Health Care, showed first attempt and overall IV success were higher and number of first attempts and staff required per encounter decreased with the vascular access team.
The team works 12 hours a day, Monday through Saturday. “We noticed that on weekends and nights we were still having some issues with pediatric vascular access, so we did a continuous improvement project with residents from our hospitalist team, our pediatric ICU, pediatric anesthesia and the vascular access team,” says Hartman. The project led to development of an after-hours, on-call system. Caregivers page pediatric ICU physicians/nurse practitioners or certified registered nurse anesthetists if they require vascular access assistance.
Every hospital within the Cleveland Clinic Health System has access to the algorithm, which features a scoring tool. A study led by Hartman confirmed the validity and reliability of the six-item Pediatric Intravenous Difficulty Score and results were published in the Fall 2020 issue of the Journal of the Association for Vascular Access.
Advertisement
Hartman’s work on the PPVAA earned her first place in Cleveland Clinic Nursing Institute’s 2020 Innovation Inventory Award. (Hartman received the 2021 Outstanding Innovation in Medical Device for another one of her creations, the High-Line™ IV tubing solution.)
She is proud of these accomplishments, as well as being named the Janet Pettit Scholar, one of only seven to date. “I’ve been a pediatric nurse for 41 years, and this award is a validation of a really wonderful career,” she says. “It’s such an honor.”
Advertisement
Advertisement
How meaningful relationships, psychological safety and everyday recognition can help sustain caregivers
Veteran nurse shares how perseverance and support can fuel impactful ideas
Interdisciplinary initiative leverages technology, documentation and diagnostic clarity to prevent skin breakdown
Program helps caregivers prepare for the unique pressures of the ICU
Multidisciplinary simulations provide realistic emergency training to help achieve optimal patient outcomes
How critical care expertise, rapid decision-making and patient advocacy are shaping perioperative care
Survey identifies opportunities for further training and ongoing moral support
Nursing quality experts help drive policies and practices designed to meet the highest clinical standards