Report details early outcomes of novel procedure
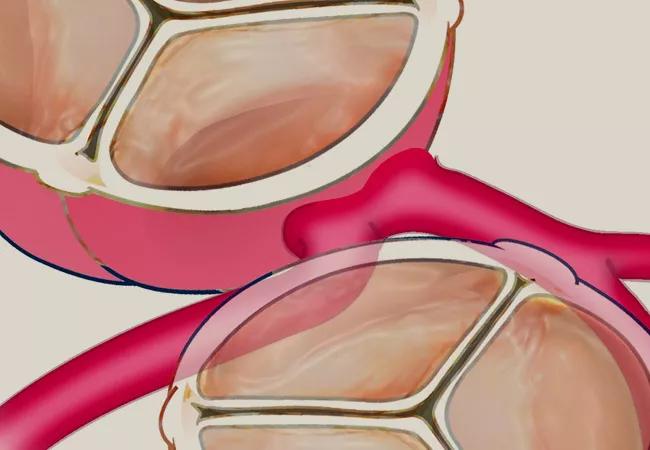
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3e0e4cf0-03ea-4c38-af0b-a1a76be6b673/19-HRT-452-AAOCA-CQD-Hero_jpg)
19-HRT-452-AAOCA-CQD-Hero
Cleveland Clinic cardiothoracic surgeon Hani K. Najm, MD has developed the first surgical technique to successfully repair a transseptal anomalous left coronary artery arising from the right coronary sinus.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
It’s a rare defect, but a potentially lethal one. Anomalous aortic origin of coronary arteries (AAOCA) has a reported incidence of just 0.1% to 0.3% of the population, but can lead to sudden cardiac death in otherwise healthy young people.
Anomalous aortic origin of left main coronary artery (AAOLCA) arising from the right coronary sinus is less prevalent (0.02% to 0.08%) than when it arises from the left coronary sinus, but the former carries an even greater risk of sudden cardiac death.
Among four distinct AAOLCA subtypes, the transseptal anomaly is the most challenging to repair. Here, the left main coronary artery (LMCA) turns sharply and dips into the basal interventricular septum behind the right ventricular outflow tract (RVOT), emerging to the epicardial surface on the lateral aspect of the pulmonary annulus before bifurcation into left anterior descending and left circumflex arteries.
Until now, coronary artery bypass grafting (CABG) has been the only approach taken, but it often fails. Instead, Dr. Najm developed a technique that involves complete unroofing of the AAOLCA and separating it from the compressive effects of the muscular RVOT, aided by multimodal provocative testing.
“I developed this technique because CABG doesn’t work due to competitive flow. The graft won’t survive. In this technique, we actually unroof this anomalous course of the left coronary artery through its entire course within the ventricular septum and bridge it with pericardium so it doesn’t get obstructed any more,” he explains.
Advertisement
In 2019, Dr. Najm published a single case report in which the unroofing approach relieved chest pain and provided unobstructed coronary flow in a 40-year-old woman with the transseptal AAOLCA anomaly.
Now, Dr. Najm and colleagues from the Cleveland Clinic teamed up to report success with an additional seven consecutive patients, ranging in age from 12 to 62. Four were female. All but the one child had angina-like symptoms. Two patients had undergone prior CABG. In all of the patients, the AAOLCA with transseptal course was confirmed by computed tomography angiography as the initial test.
Four of the patients underwent cardiac catheterization with intravascular ultrasound (IVUS) and indexed fractional flow reserve (iFFR) that confirmed a flow-limiting lesion. Importantly, three of those four had negative provocative noninvasive testing for ischemia, despite typical angina symptoms.
Six of the seven patients had normal left ventricular ejection fraction. Three patients had dobutamine stress echocardiography or positron emission tomography (PET) demonstrating anterolateral ischemia, and one patient had normal stress PET.
The median postoperative hospital stay was four days. None of the patients died or experienced major complications over a median follow up of nine months. Postoperative evaluation showed anatomically patent unroofed AAOLCA with improved flow (iFFR 0.90 versus 0.59 at baseline, P = 0.05).
In one patient, modest reductions in iFFR were seen postoperatively despite the absence of symptoms, while additional imaging with both perfusion PET and stress echocardiography were reassuring. This highlights the need for multimodal evaluation, Dr. Najm and colleagues note in the paper.
Advertisement
Today, all of the patients are in New York Heart Association functional class 1 with excellent exercise tolerance.
Dr. Najm and colleagues have performed at least eight more successful unroofing repairs of this defect since. Surgeons from around the world have contacted him to ask about the technique and to report that they’re using it. “People should be able to do it if they follow what I detailed in the first and second paper. It’s not really complex,” he says.
Dr. Najm credits Cleveland Clinic with providing “the environment and the support for innovative surgical techniques. The teamwork and the reliability of the team, both in the OR and the aftercare, allows surgeons to innovate. We always continue to push for improved technique and improved care.”
Featured image: Illustration depicts anomalous aortic origin of coronary arteries (AAOCA) involving the left coronary artery (AAOLCA).
Advertisement
Advertisement
What to know about the condition, and 5 strategies to improve patient care
Biologic therapy and advances in monitoring may ease treatment and follow-up for families
Minimally invasive options for conditions that may otherwise require surgery or referral to adult centers
AHA statement provides the latest comprehensive, evidence-based information
Helping clinicians manage cancer treatment in patients with complex biology
Infants with > 30° of cervical tightness were also more likely to be younger at evaluation
Findings hold lessons for future pandemics
One pediatric urologist’s quest to improve the status quo