Nurses describe challenges and joys of caring for hospital’s most vulnerable patients
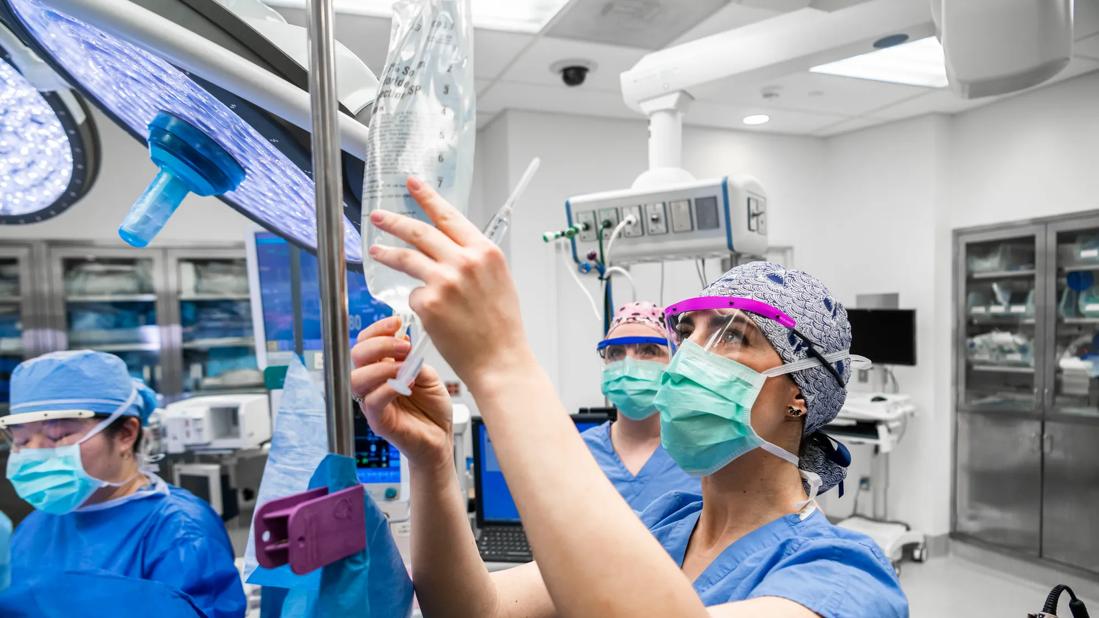
Founded nearly 55 years ago, Cleveland Clinic’s School of Nurse Anesthesia was one of the first educational programs in the U.S. to formally train caregivers to work in the specialty. Originally established to fulfill a burgeoning need for qualified nurse anesthetists, the school has continued to meet this growing demand by educating scores of scholars every year on the most current evidence-based techniques for managing complex surgical patients.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
About 75% of the certified registered nurse anesthetists (CRNAs) working at Cleveland Clinic’s main campus graduated from the healthcare system’s School of Nurse Anesthesia, as did approximately half of the CRNAs who practice at Cleveland Clinic’s regional hospitals.
“Our program continues to meet a growing workforce need,” says Angela Milosh, DNP, CRNA, FAANA, Program Director for the school, which is a shared collaboration with the Frances Payne Bolton School of Nursing at Case Western Reserve University. “CRNAs are in great demand largely because of the high acuity of the patients they serve, and we continually try to do our part by preparing our students to provide exceptional care.”
A CRNA herself, Milosh is a graduate of Cleveland Clinic’s School of Nurse Anesthesia and has practiced at the healthcare system’s main campus for more than 20 years.
“The nurse anesthesia curriculum is a rigorous, full-time-plus undertaking,” she says. “It is academically and clinically challenging because you are working with patients with complex needs who are undergoing complex procedures.”
Through the years, the program has evolved from a diploma course to a nationally recognized and accredited doctoral curriculum. Graduates receive a diploma in nurse anesthesia from the Cleveland Clinic Foundation and a Doctor of Nursing Practice degree from Case Western Reserve University. To be accepted into the program, candidates must have a bachelor’s degree in nursing, be a licensed registered nurse and have at least one year of critical care nursing experience.
Advertisement
Approximately 20 to 25 students enroll in the 36-month program each year, all of whom are required to complete more than 700 didactic and 3,000 clinical hours during the course of their education. There have been 550 graduates since the school was founded in 1969.
Milosh, who currently works with adult surgical patients, explains, “It is competitive, but that’s one of the things that makes our program special. We recruit the highest-quality critical care nurses we can find.”
Among the personal qualifications that can help a CRNA student succeed, Milosh adds that candidates must be prepared to transition into a new role within the healthcare organization and shift from being a working professional to a learner. This can be particularly challenging for some, she says, because CRNA students must give up full-time work to meet the demands of their classes and clinicals.
“Embracing a growth mindset doesn’t come naturally for everyone,” she notes. “When you’ve already been working as a caregiver, it’s not always easy to move into an unfamiliar environment where you’re expected to learn new skills. But once a candidate makes that mental shift, the sky’s the limit in what they can achieve. Watching that growth is one of the most fulfilling parts of my role.”
Ashley Austin, DNP, CRNA, Assistant Program Director for Cleveland Clinic’s School of Nurse Anesthesia, is a graduate of the program as well. When asked what she would tell someone who is considering further training as a CRNA, she says, “The arduous journey to becoming a CRNA is well worth it, and the opportunities are endless.”
Advertisement
Austin, who practices in the pediatric anesthesiology department, also advises potential CRNAs to seek out a mentor. A mentor can assist caregivers successfully navigate the CRNA career path and provide ongoing, career-long support, she says.
Because the CRNA’s job is to administer pain management and anesthesia, they are often the last face a patient sees in the operating room. That responsibility demands that CRNAs be emotionally intelligent and have a strong affinity for patient advocacy, says Milosh, and that includes being willing to speak up when necessary.
“Nurse anesthetists have a responsibility to approach their patients with empathy while providing safe, competent and ethical care – and teaching them how to do that is our chief goal,” she explains.
Working as a CRNA has its share of challenges and rewards – and for Milosh, those experiences are often one and the same. “In many cases, we are the only option the patient has left, so our objective is to get them through their surgery as safely as we can,” she explains. “And when we succeed, it is truly the most rewarding experience imaginable. We are problem-solvers by nature, so seeing a patient come through a procedure successfully is incredibly satisfying.”
As a pediatric CRNA, Austin adds that it can sometimes be difficult to compartmentalize her emotions when it’s time to head home. “Our work can be heavy, especially when a child’s well-being is at stake,” she says. “Although it can be hard to leave your feelings at the hospital when your shift ends, that internal conflict is a reminder of the critical role we play in patients’ lives. It is an honor to be present with families when they are going through difficult times, and I take that responsibility very seriously.”
Advertisement
For more information on becoming a CRNA, visit the School of Nurse Anesthesia online or email CRNAschool@ccf.org.
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader