Three key messages for patients

Ralph Turner, Executive Director of Patient Support Services (PSS) at Cleveland Clinic, likens a hospital enterprise to a solar system. Operations (which includes Patient Support, Environmental and Protective Services) form the outer orbit that supports all other services. Ancillary services are next in, circling the medical caregivers, who in turn orbit around the patients and families at the center.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In a similar vein, Gordon Snow, Chief of Protective Services, describes the goal of his department as, “providing world class service so others can provide world class care.” This is accomplished only by creating a safety shield around patients, visitors and caregivers at Cleveland Clinic’s main campus near downtown Cleveland, as well as the dozens of health system facilities throughout the Northeast Ohio region. (This article focuses primarily on main campus efforts.)
Mike Visniesky, Senior Director of Environmental Services (EVS) speaks of his mission to protect patients with an impermeable microbial barrier.
In the past few years, all three leaders have moved Cleveland Clinic’s Operations scores to top percentile rankings among peer enterprises. Each uses finely-tuned analytics to measure their departments’ progress, reviewing these with their teams daily in performance feedback loops. Each employs a servant leadership philosophy that fosters buy-in to rigorous training, goal-setting and a sense of mission among their staff.
The net effect? Operations sends three messages to patients, families and caregivers: We will care for you, we will care about you, and while you are at your most vulnerable, we will help you maintain as much control as possible.
In Protective Services, caring means greater integration with everyone on and around the main campus. “With the uptick in security threats over recent years, in all public realms, we are doing more to ensure that our police officers and security staff are visible partners in the ED, on the floors and in the parking lots, and more interactive with staff and patients,” Mr. Snow explains.
Advertisement
Mr. Snow’s group is serious about the mantra “If you see something, say something.” “We make it easy to raise concerns. It’s not necessary to go through a chain of command. If I’m the only one they think of at the moment, they have my number, and can call me. I’ll answer!”
Mr. Visniesky’s EVS group cares for patients so well that the Joint Commission, in their 2018 surveys, could not find a single flaw. He credits this to a relentless drive to eliminate variances in cleaning/disinfection practices, no compromises on checklists or SOP adherence, and daily huddles to review performance.
Mr. Turner’s PSS group has found a new way to protect from delivery of meals that are incorrect or even dangerous, as in the case of a food allergy. In one cardiac unit, a new full-service, fresh food concept is being piloted, wherein the patient calls in their order and a staff member checks their medical record while they are on the phone to assure their meal is safe for them. This improves on the ticket system where food restrictions are flagged later in the process.
“Family members and patients have a lot of angst about being at the hospital. Some arrive at the main campus parking lot after a long drive or flight, as early as 4 to 5 a.m. When a shuttle driver, security guard or a red coat picks up on this, they offer an ear and some comfort or help to a mom juggling bags and a baby,” Mr. Snow says. “We are flooded with letters constantly, telling us how comforting it was to have the police present when they are going to their vehicle or having shuttle folks looking out for them as they go back and forth from the hospital to their hotel room at 1 or 2 in the morning.”
Advertisement
Police and security officers are so integrated with patient care that officers are asked for by name, especially by young patients. “Particularly with our sickest children, we often try to do a little something for them that brightens their day,” Mr. Snow explains. “We recently conducted a swearing-in ceremony for a little boy, giving him his police officer certificate, badge and a CPD ball cap.” He adds, “Feeling helpless to change the outcome, at least you can change this day for this child.”
Caring about patients also means Environmental Services staff aren’t the silent “cleaning crew” they once were. “We train our caregivers to approach the patient, make eye contact and talk with them rather than at them about what they will be doing and why cleaning the way they do is important,” Mr. Visniesky relates. His staff receives training on first impressions and emotional intelligence. “We practice not only what we say, but how we say it.
Dashed expectations make people feel helpless. “Patients can have the best surgical procedure, the best care, and all of a sudden they get the wrong food order and their whole episode of care goes down the tubes,” Mr. Turner explains. “Their food order is sometimes the one thing they can control. So if we can deliver the meal they ordered, hot and delicious, it really makes a difference!”
Mr. Snow’s team boosts caregivers’ control over challenging behavioral situations by training staff in de-escalation techniques. Equally important, they make sure caregivers know they are not expected to tolerate or handle abusive or threatening situations. “That is why we are here,” he says.
Advertisement
The net effect of Operations staff doing their jobs is sometimes clearest when a patient is discharged. Familiar faces may appear as the patient transport employee wheels them down to the exit, a shuttle driver may take one family member to a car in the parking lot while a valet brings a vehicle to pick up the patient and others. A security guard waves goodbye. The last impressions these “operations caregivers” make may color patient experience as much as the success of the procedure or treatment itself.
“You can’t ignore this and provide world class care,” Mr. Snow reflects.
Advertisement
Advertisement

Advanced software streamlines charting, supports deeper patient connections

How holding simulations in clinical settings can improve workflow and identify latent operational threats

Interactive Zen Quest experience helps promote relaxing behaviors

Cleveland Clinic and IBM leaders share insights, concerns, optimism about impacts
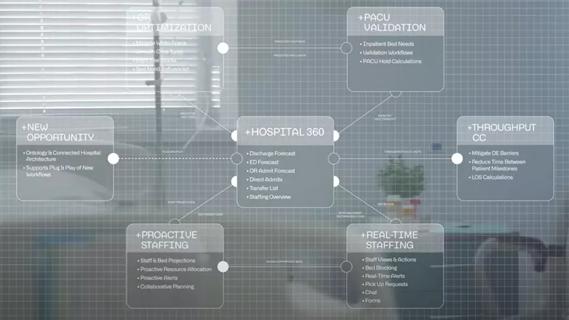
Cleveland Clinic partners with Palantir to create logistical command center

A Q&A with organizational development researcher Gina Thoebes

Cleveland Clinic transformation leader led development of benchmarking tool with NAHQ

Raed Dweik, MD, on change management and the importance of communication