Study links worse presurgical pain, function and mental health with dissatisfaction one year after surgery
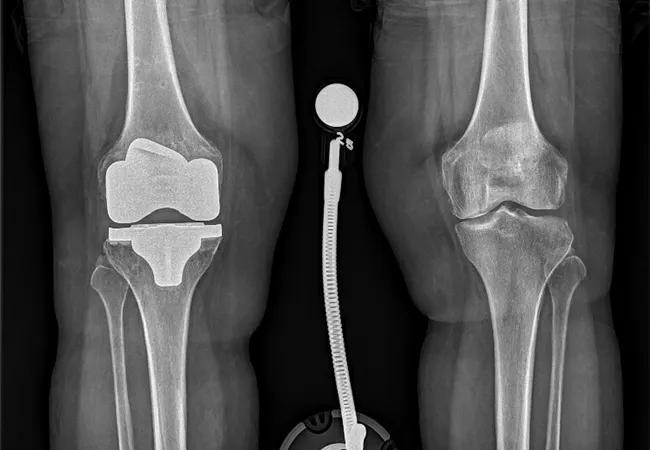
Approximately 1 in 5 patients who had total knee arthroplasty report dissatisfaction with the procedure. A new study has uncovered potential drivers of that dissatisfaction: the patient’s presurgical knee pain, knee function and mental health.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Instead of studying these factors individually, researchers studied them in combination and developed patient phenotypes that could help predict an individual’s outcome of total knee arthroplasty.
“We found that a patient’s outcome often depends on where the patient starts,” says the study’s senior author, Nicolas S. Piuzzi, MD, Director of Adult Joint Reconstruction Research in Cleveland Clinic’s Department of Orthopaedic Surgery. “Patients who reported worse pain, function and mental health scores before surgery had a 1-in-4 chance of being dissatisfied with total knee replacement. Those who started out with better scores had only a 1-in-15 chance.”
These findings may help facilitate a new personalized approach to total knee replacement, he says.
The study, recently published in The Journal of Arthroplasty, was presented at the American Academy of Orthopaedic Surgeons’ 2022 meeting and the Orthopaedic Research Society 2022 meeting, where it received a Strategies in Clinical Research Section Award for outstanding quality and scientific achievement.
Researchers studied more than 5,000 patients with osteoarthritis who had knee arthroplasty at Cleveland Clinic from 2016 to 2019. Approximately 16% of patients (N = 862) reported the state of their knee as “not acceptable” on the Patient Acceptable Symptom State (PASS) questionnaire one year after surgery. Researchers found that:
Advertisement
Overall, 22.7% of patients with lower self-reported pain, physical function and mental health scores before surgery said their symptoms were “not acceptable” one year after surgery. The same was true for only 10.9% of patients who self-reported better pain, physical function and mental health scores before surgery.
In addition, patients with lower physical function and mental health scores before surgery were more likely to have a prolonged hospital stay after surgery and not be discharged to home. However, patient-reported data was not associated with higher risk of 90-day readmission or reoperation within one year.
“These data can help guide us on how to counsel patients considering arthroplasty and may even guide us in providing interventions to help higher risk patients improve their chance of success after surgery,” says Dr. Piuzzi. “A cookie-cutter approach, in which everyone gets the same orthopaedic care, is not always preferable. We can tailor the experience for each patient by incorporating patient-reported data.”
Different care paths could be designed for different patient-risk levels, he says, adding that patients should know in advance if their chance of satisfaction after surgery is 90% or 70%.
“That’s a big difference,” he says. “Setting expectations also can help improve satisfaction, especially for patients who may require extra care or take a little longer to achieve full results.”
Seasoned surgeons already may be advising patients based on experience and anecdotal evidence. However, Dr. Piuzzi’s study may enable a data-driven approach that empowers patients to compare themselves to other patients and make evidence-based decisions about their care.
Advertisement
Results of the study also present new considerations in arthroplasty. For example, should patients have surgery sooner, before their KOOS, KOOS-PS or VR-12 MCS scores begin to drop? Should mental health be addressed regularly by orthopaedic providers?
“Mental health was a major driver of total knee outcomes,” says Dr. Piuzzi. “It would make sense for surgeons to talk about mental health as commonly and comfortably as we talk about a broken bone or arthritis. If a patient has been suffering with pain and poor physical function for years, it obviously could affect their mental well-being.”
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment