A closer look at select programs and services

In pediatric rehabilitation, big wins come from small moments: eating one bite of food, pointing to a toy or getting into the pool. Cleveland Clinic Children’s Hospital for Rehabilitation (CCCHR) offers an array of inpatient and outpatient services for children with chronic and complex medical challenges.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Teams of physical, behavioral, occupational, speech and recreational therapists work together to deliver individualized care. Each program is different, but their overarching goals are the same: provide children with the tools to return confidently and comfortably to their lives.
The newest of Cleveland Clinic’s therapy services groups, Tiny Dancers, was launched in early 2022 by physical therapist Kelsey Michels. Michels says the program is an opportunity for the children, many of whom are diagnosed with movement disorders, incoordination or hypotonia, to practice balance, coordination and rhythmic training while also learning the basics of ballet.
“They don’t realize how hard they’re working while they’re moving to music,” says Michels. The eight-week program culminates in a recital, showcasing their newly learned ballet dance and combinations across the floor as well as a renewed sense of confidence and pride.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/89ddc89d-a8f9-4a06-8797-d206b323faf7/CHP_3300542_10-17-22_026_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/880126c5-b991-4984-9748-e313076101de/CHP_3300542_10-17-22_067_LDJ-1-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/6649cefe-69bc-4751-8ad8-00926d4290d9/Picture3-1_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/4d9012e6-8def-4912-a1b0-30a203365a86/Picture2-1_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/08181f7e-a0ce-45bd-8f51-8d10187d69b6/Picture1-1_jpg)
Physical therapist Brandy Plas created Gym Class Heroes with a specific patient population in mind: older children who are not participating in sports and have aged out of some of the physical activity programs better suited for younger kids. On the first day of class, physical therapists obtain the kids’ 6-minute walk test to measure overall endurance, manual muscle grade for core strength and other standardized fitness tests. They get these metrics again on the last day and typically note significant physical improvements over the program’s eight weeks.
Plas says parents and guardians have voiced gratitude for the transformation they’ve noticed in their child, many of whom had previously shied away from exercise but now look forward to it and want to incorporate it into their home life.
Advertisement
“It’s rewarding for them and us to see their progress and growth and gain a sense of community.”

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/cd4ee910-2ab7-40fb-94cd-d14112cfc3b4/CHP_3307405_10-04-22_094_RN-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/dba71927-9b37-45dd-a227-7b1a158cfe1e/CHP_3307405_10-04-22_010_RN-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d6b702b7-5762-43e0-9f9d-12c51e0eea9d/CHP_3307405_10-04-22_029_RN-scaled_jpg)
The constraint-induced movement therapy program is an intensive occupational therapy program for children with weakness to one side of the body that can result from a brain injury from stroke or seizures, brachial plexus injury or injury to the nerve. Children attend the program several hours a day, five days a week, for three weeks.
The therapy technique is achieved by casting the child’s nonaffected arm, encouraging them to rely on their weaker side to complete basic tasks like self-feeding and brushing their teeth. The ultimate goal is for them to use their affected arm as much as possible.
“There is a strong focus on repetition and grasping patterns. It helps forge new neuropathways in a child’s brain to strengthen their body and, specifically, their nondominant arm,” says Rebecca Burdick, the program’s occupational therapist. Outcomes differ for each child, but most children generally increase their strength, range of motion and fine motor skills.
“Usually, in the beginning, when they try to pick up small objects, they’re using their whole hand, but by the end, they’re able to demonstrate control, using just their pincer grasp,” says Burdick. Families have come from all over the country — including central Pennsylvania, Chicago, Florida and Oklahoma — just to access this program.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/26b06904-06bc-427d-b98d-d4017ceedcf9/CHP_3310858_09-29-22_069_AMO-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/fa08acdf-69d9-4976-b652-2c917005dc2e/CHP_3310858_09-29-22_029_AMO-Edit-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1011fe35-aeea-4d5d-b4bb-4e83128bf21d/CHP_3310858_09-29-22_001_AMO-scaled_jpg)
There are many possible causes for feeding disorders, explains pediatric occupational therapist Nicole Gipson, who specializes in feeding therapy. Cleveland Clinic Children’s outpatient feeding program treats children from infancy to 20 years old. After the patient’s feeding skills are evaluated, the therapist works with the patient and family to develop an age-appropriate goal plan.
Advertisement
“To improve the ability to safely and fully participate in mealtime, we may need to target a patient’s strength, and coordination and also incorporate interventions that facilitate sensory processing skills,” explains Gipson.
In some cases, goals are addressed outside of the mealtime as well, such as providing opportunities for sensory play and adapting activities related to daily living. Although plans differ based on the child and their level of need, Gipson says it comes down to “meeting the patient and family where they are.” Completing goals could take a month, or it could take years. But the goal is the same: eating in a timely, efficient, healthy and age-appropriate way.
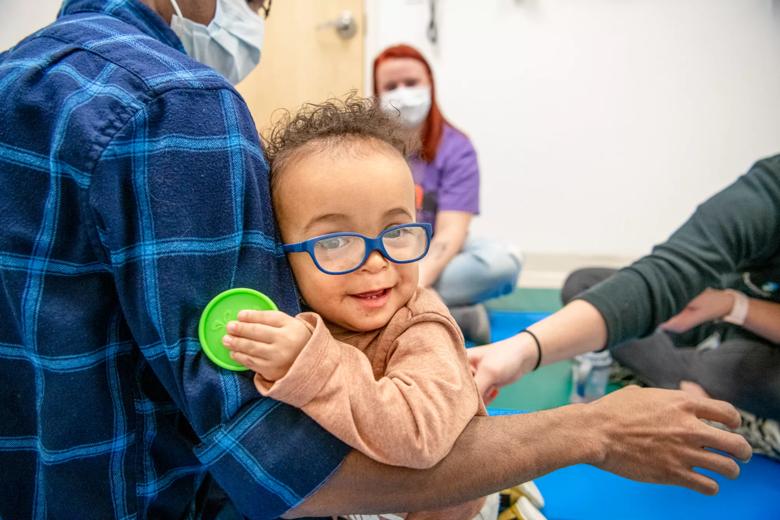
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/dff210a0-e696-4785-9530-434a1d9cec62/CHP_3320659_10-27-22_079_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3b14673d-aa45-4c29-a93b-29e058af035e/CHP_3320659_10-27-22_051_LDJ-scaled_jpg)
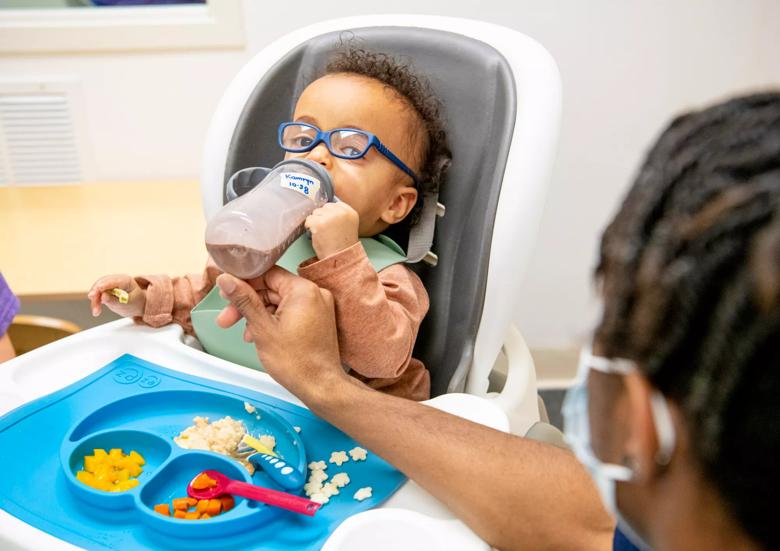
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/515f408b-dd5a-4e56-a61a-0bed19c8a0e1/CHP_3320659_10-27-22_016_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/daac07b9-94de-43de-bf0d-7f2061e44d1f/CHP_3320659_10-27-22_003_LDJ-scaled_jpg)
Aquatic therapy can be a form of physical, occupational, speech, recreational therapy or some combination of all. For some kids, water, with its natural reduction of gravity force, is the optimal environment for muscle strengthening, improving balance, and developing endurance. Aquatic therapy plays a significant role in acute rehabilitation and pain rehabilitation programs, as the kids enrolled use the program five days a week, and is also available for outpatient care.
Lisa Leonard, an inpatient therapy clinical manager at Cleveland Clinic Children’s and speech-language pathologist by training, and her team work closely with children involved in aquatic therapy, many of whom have brain injury, stroke, encephalopathies or cerebral palsy. She and her colleagues have helped countless children with their range of motion, strength and physical function in the water, improving their ambulation on land.
Advertisement
She says helping children regain their function or progress toward their goal of doing so — and seeing them have fun while doing it — makes her work worthwhile.
“We know some of these children will have challenges ahead of them, but we’re not looking at what they can’t do. Instead, we’re always focusing on what we can do to help them be more independent,” says Leonard.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b1224af4-ba04-4f5a-a3bd-36bbf84a4e31/CHP_3405517_11-16-22_0113_AMO-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/88cdb41a-88e7-44a3-b1b0-73a3c96d0992/CHP_3405517_11-16-22_0300_AMO-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7e36f79d-3d26-4d34-9b1c-a9b69ddb1361/CHP_3405517_11-16-22_0594_AMO-Edit-scaled_jpg)
Caregivers in the Seating and Mobility Clinic work closely with children and their families to design custom mobility solutions. Insurance constraints mean there is a five-year commitment to the frame itself, so the team works to ensure the child’s needs are met — and will continue to be as they grow.
Meghan Price, an occupational therapist at Cleveland Clinic Children’s, is integral to this process. “Our job is to assess a child’s positioning and mobility needs, educate the child and their family about equipment options that are available, and assist with trialing, ordering and obtaining the appropriate equipment,” she says. And options abound: from a power-assist system or customized manual options to a power chair, head array system and more.
Types of positioning and mobility outcomes vary depending on the child. Price explains that independence can sometimes be achieved through modifications to their mobility system. For example, a successful outcome in a patient with significant scoliosis is a system that can support upright trunk or head control that allows the child to use their hands, eat, swallow, and have more functional breathing patterns. Or a successful outcome could be mobility for the first time through the support of a wheeled system.
Advertisement
“Ultimately, access to increased independence and involvement with daily activities, that the child wouldn’t otherwise be able to participate in, is one of our main areas of focus,” concludes Price.
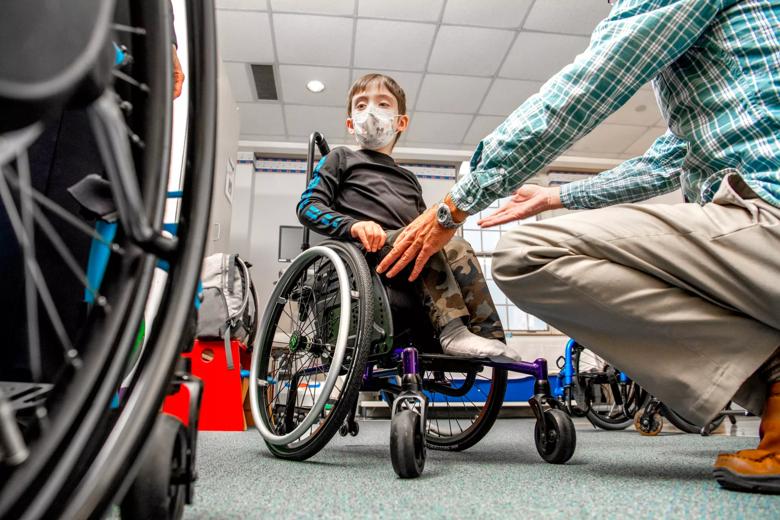
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ce68509f-9d91-4488-b4ca-d40c7c20dcf4/CHP_3449908_11-30-22_006_LDJ-scaled_jpg)
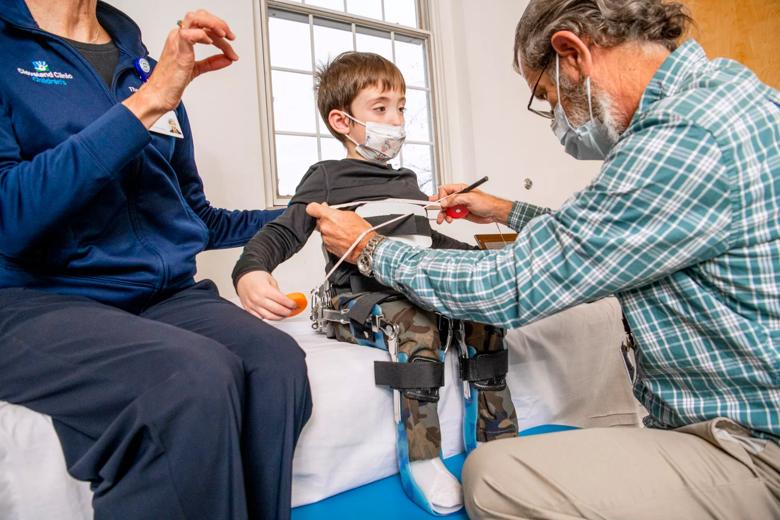
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/bbfb1edd-0603-4c38-b85d-d7fe186beb50/CHP_3449908_11-30-22_020_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/dc2730ee-7971-417a-9394-3da6b02cc8b9/CHP_3449908_11-30-22_059_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b0a4a59e-5c52-42c3-89d3-4862025aa5f4/CHP_3449908_11-30-22_035_LDJ-scaled_jpg)
Though outpatient autism services is housed under Cleveland Clinic Children’s Center for Autism — and not Pediatric Rehabilitative Services — it shares the same spirit as the other outpatient programs offered by CCCHR. It’s an early intervention program, so program staff treat kids from their diagnosis through age 8.
Chiara Graver, Supervisor for Outpatient Services at the Center for Autism, explains that though treatment plans are individualized, goals are achieved in one-on-one and group-based settings for children at similar skill levels. “Our services are very play-based—from color, number, and letter learning activities and also imaginary play, which can be a challenge for kids with autism,” says Graver. She says they also practice making requests of peers and therapists. In addition, breaks for gross motor sessions help children practice transitioning skills and participate in group activities and free play — all experiences that would happen in a school setting.
“We get a lot of patients who have been recently diagnosed or who have had limited exposure to therapeutic services or school, and so many of them begin with limited communication and play skills,” she says. “So, the little things, like using a finger to point to something — when they weren’t previously able to — is so rewarding.”

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/32ffe3a8-4006-4d60-bab8-50358a82b0f2/CHP_3605358_02-10-23_018_LDJ-scaled_jpg)
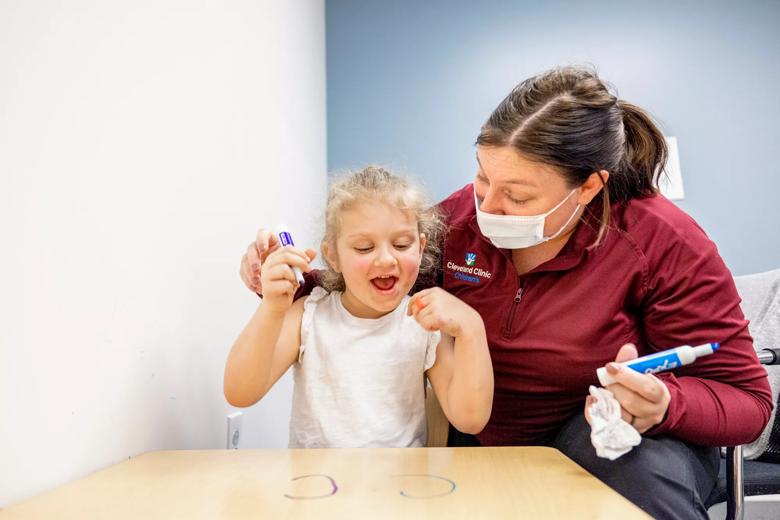
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/cffa4cfe-8c70-43ea-b253-f1e3f2794c50/CHP_3605358_02-10-23_048_LDJ_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/02a26e6f-c06e-4ec9-9619-d199c13b4093/CHP_3605358_02-10-23_073_LDJ_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0dece3f8-9115-48ee-a241-e8dae4c09740/CHP_3605358_02-10-23_116_LDJ_jpg)
There are different pathways to inpatient rehabilitation: functional change due to trauma-based events, spinal cord injuries related to trauma or disease, neurologic diseases, and more. “But most of the time,” says Lainie Holman, MD, Chair of Pediatric Physical Medicine and Rehabilitation at CCCHR, “these are children who were functioning normally, and for whatever reason, they aren’t anymore.” Inpatient rehab can help. It involves three to five hours of therapy a day for up to 12 weeks, particularly in complex spinal cord or brain injury cases.
The inpatient rehab team meets weekly to discuss each patient and the barriers preventing them from a safe return home.
“Each child is different and has individual goals, but when we determine they are going to be safe at home and only need therapy a few times a week, then we work toward discharge,” explains Dr. Holman. In addition, the team works closely to connect patients and their families with support and resources for reentry to school and the community.
“Some children walk right out, but, more often, they don’t, and our team is here to help them navigate these new challenges,” notes Dr. Holman.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8c50dc71-6fba-44fe-84b1-02619b26eb0b/CHP_3459275_12-7-22_004_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/dfbf9ae2-7d2e-4940-b3ab-ddfff649fa84/CHP_3459275_12-7-22_009_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/753ee7d0-e399-4185-82ed-b38c2a2d240a/CHP_3459275_12-7-22_020_LDJ-scaled_jpg)

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1f6a6468-d1d5-48a8-b9c2-ed569d89765b/CHP_3459275_12-7-22_065_LDJ-scaled_jpg)
Photography by Lisa DeJong, Annie O’Neill and Reen Nemeth
Advertisement

Strong bonds and momentous milestones fuel life-changing work

Exploring the role of caregiver education and objective feedback on speech and language outcomes

Various AR approaches affect symptom frequency and duration differently

Physicians in the field should tout an array of accomplishments to achieve well-deserved recognition

How lyric writing, song production is helping patients ‘reclaim their power’

Findings hold lessons for future pandemics

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials