Multivariable models help estimate risk of postoperative declines in cognition and mood
Podcast content: This podcast is available to listen to online.
Listen to podcast online (https://www.buzzsprout.com/2243576/13534516)
While temporal lobe resection is effective at reducing or eliminating seizures in patients with medication-resistant temporal lobe epilepsy, some people experience postoperative declines in cognition or new or worsened depressive symptoms. Prediction models developed at Cleveland Clinic can assist clinicians in identifying who may be at risk for these changes following surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The goal is to provide more information so patients can consider the risks and the benefits of epilepsy surgery and have realistic expectations regarding their outcomes,” says Robyn Busch, PhD, ABPP-CN, a clinical neuropsychologist with Cleveland Clinic’s Epilepsy Center. “If we identify those patients who may be at higher risk for changes in cognition or mood following surgery, clinicians can provide more comprehensive preoperative counseling and follow them more closely during the postoperative period.”
Dr. Busch discusses the development and use of the predictive models in the latest episode of Cleveland Clinic’s Neuro Pathways podcast, including the following:
Click the podcast player above to listen to the 16-minute episode now, or read on for a short edited excerpt. Check out more Neuro Pathways episodes at clevelandclinic.org/neuropodcast or wherever you get your podcasts.
This activity has been approved for AMA PRA Category 1 Credit™. After listening to the podcast, you can claim your credit here.
Podcast host Glen Stevens, DO, PhD: What are your long-term goals for these prediction models?
Advertisement
Dr. Busch: We’d like to continue to update and refine the models over time in order to increase their predictive accuracy. The predictive accuracy is pretty good in most of them, and certainly much better than chance, but I think we can continue to do better, particularly if we use more complex predictors from the preoperative workup/evaluation — information such as EEG and MRI. And we are working on that now.
We’d also like to develop models to estimate not only the presence of postoperative decline but also the magnitude of that decline and how it might impact functioning for the patient. And then ultimately what we would like to do is develop and validate a suite of prediction models on the same patient cohorts in order to simultaneously predict all outcomes that are relevant and meaningful to patients, such as the chance of seizure freedom along with the potential risks of cognitive and mood changes.
Dr. Stevens: What do these prediction models mean for the future of epilepsy surgery and clinical decision-making for physicians and patients?
Dr. Busch: The goal of this research really is to help clinicians consolidate identified risk factors for cognitive and mood outcomes, which are often contradictory. And using these models, the goal is to have high predictive accuracy in order to assist clinicians in accurately counseling their patients regarding the potential risks and benefits of epilepsy surgery to aid clinical and surgical decision-making, and ideally to permit early identification of those small subset of patients who may require closer postoperative monitoring. Ultimately, our hope is that these types of studies will pave the way toward precision medicine approaches in the treatment of epilepsy.
Advertisement
Advertisement

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Patients with epilepsy should be screened for sleep issues

Sustained remission of seizures and neurocognitive dysfunction subsequently maintained with cannabidiol monotherapy
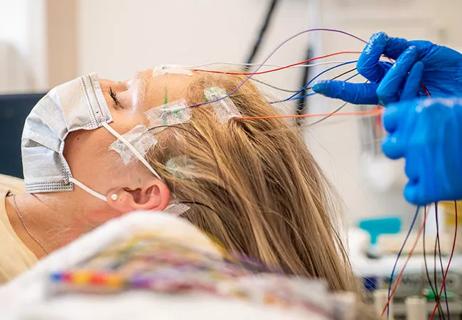
Model relies on analysis of peri-ictal scalp EEG data, promising wide applicability

Investigational gene approaches offer hope for a therapeutically challenging condition
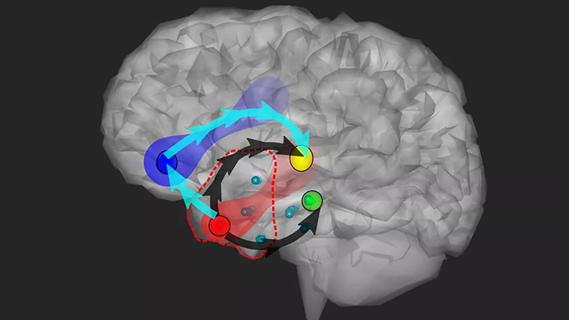
Study combines intracranial electrophysiology and SPECT to elucidate the role of hypoperfusion

Characterizing genetic architecture of clinical subtypes may accelerate targeted therapy

Data-driven methods may improve seizure localization and refine surgical decision-making