Advertisement
Nurse researches possible option to boost disposal rates

The role of prescription opioids in the escalating opioid crisis is well known throughout the healthcare community. Overdose deaths involving prescription opioids were five times higher in 2017 than 1999, according to the Centers for Disease Control and Prevention. What is less obvious is the solution.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“When this crisis was coming to light, I was intrigued by solutions we could implement to help combat the opioid crisis, which is growing exponentially,” says Antoinette Zito, MSN, RN, CPAN, a perioperative educator at Cleveland Clinic Hillcrest Hospital and a member of the healthcare system’s opioid task force. “I decided to apply the scientific method and really see if we could find a solution.” She launched a research study to determine if implementation of a program for safe medication disposal in a perioperative unit would encourage patients to properly dispose of unused opioids.
Opioids are dispensed to manage postoperative pain after same-day surgery. While they are effective in treating pain, patients may retain unused prescriptions even after the pain has ebbed. Retained prescription opioids may be diverted to other users or inappropriately used for a purpose not associated with postoperative pain, thereby contributing to opioid misuse.
A couple years ago, Zito attended a national conference where she discovered commercially available drug disposal bags that contain activated charcoal that bonds to and deactivates the active agent in a prescription drug. The bags seemed like a better option to typical disposal options, including periodic community drug take-back events, police department drop-off bins and flushing drugs down the toilet.
“We designed a study to find out if patients would use the drug disposal bags we gave them and would get rid of their unused opioids,” says Zito. She conducted the study under the mentorship of Nancy Albert, PhD, CCNS, CHFN, CCRN, NE-BC, FAHA, FHFSA, FAAN, Associate Chief Nursing Officer of Cleveland Clinic’s Office of Nursing Research and Innovation.
The goal of the study was two-fold:
The study was a two-group experimental design with 30-day follow-up involving same-day surgery adult patients who received prescription opioid orders. Participants were randomized to usual care or usual care plus an opioid disposal bag with instructions for use given pre-discharge. Out of the 249 patients enrolled in the study, 115 received usual care and 134 received usual care plus the drug disposal bag.
Advertisement
The between-group disposal rate of unused opioids was collected using a questionnaire via telephone calls with Zito, 30 ± 10 days postsurgical procedure. They were measured by objective communication with patients or significant others living with the patients. Factors of interest included demographics, marital status, insurance type, surgical characteristics, use of opioids preoperatively and pain characteristics. Outcome and other factors were retrieved from electronic medical records and an administrative database.
“When I started calling people, we thought we would have two groups: people who threw away their opioid medication and people who used them all,” says Zito. “We didn’t anticipate that people would admit to saving them. Approximately 68% of patients saved all their medications.” Between the patients who saved their medications and those who used the full prescription, there were very few patients available who used the disposal bags (intervention group) or disposed of unused opioid agents in another manner (intervention or usual care group). Groups were evenly matched in terms of using all medications or saving their prescriptions.
Although overall disposal rates were low, says Zito, disposal rates were higher in the group that received drug disposal bags. In addition, diagnosis category and perceived postoperative pain were associated with disposal of unused opioid medication.
“We still need to learn the best method of disposal,” concludes Zito. “The disposal bag does help, but only for less than 10% of all patients, since the rate of wanting to dispose of unused opioid medications was very low. More research is needed.” It might be that patients in our geographical area are different than in other communities or that patients who agreed to participate in research are different or had different types of surgeries than those that did not participate. In addition, more research is necessary to learn the leading factors associated with opioid retention or disposal once the need for using the medications has passed. Finally, it will be important to learn if the cost of the disposal bags is justified.
Advertisement
Advertisement

Fellow critical care nurses welcome additional support and expertise
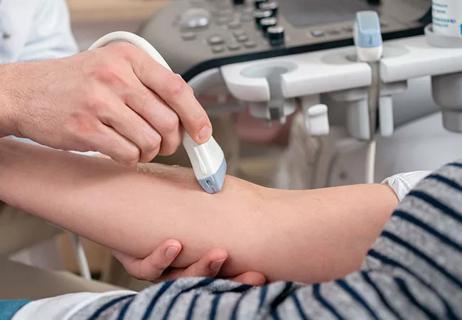
Study shows ultrasound can be valuable tool for improving patient satisfaction by reducing failed IV insertions

New system uses vital signs to predict need for further intervention

Findings reveal personal and professional factors that influence nurses’ interest in medical research

Nurse scientists bridge divide between bench and bedside

Individual and population factors play a role
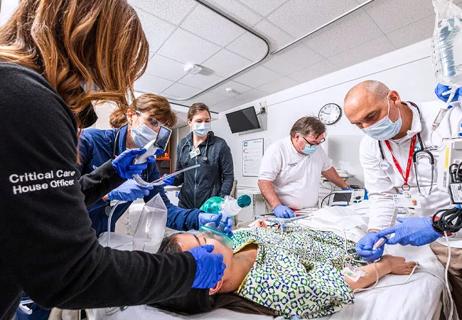
Study looks at cardiopulmonary arrest and activation rates

Video education and nurse-led reinforcement help with fall risk awareness