Study finds laparoscopic RYGB may be a reasonable alternative to traditional fundoplication
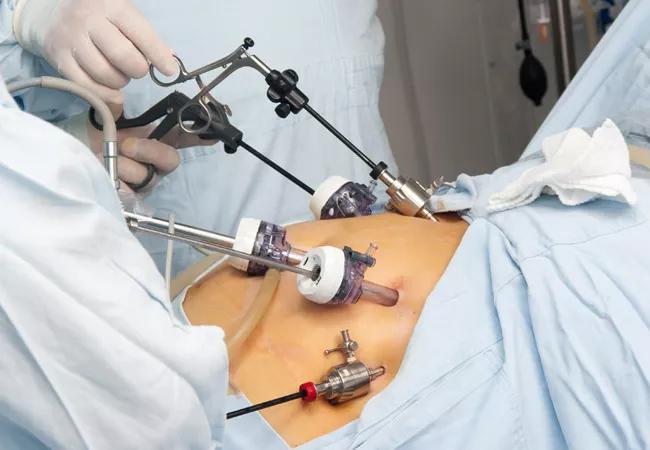
Gastroesophageal reflux (GERD) is a common complaint of patients with the rare autoimmune disease systemic sclerosis (scleroderma). According to Matthew Kroh, MD, Chairman of the Digestive Disease Institute, Cleveland Clinic Abu Dhabi, United Arab Emirates, “the typical surgical approaches to treatment of reflux for these patients may not have the same effectiveness in this population. Careful consideration must be made before surgical intervention to prevent untoward complications and give patients the best results.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dr. Kroh and his colleagues conducted a retrospective study comparing Roux-en-Y gastric bypass (RYGB) to the more traditional technique of fundoplication in patients with scleroderma. “We hypothesized that laparoscopic RYGB might be the best reconstruction technique to decrease both acid and bile exposure to the esophagus, especially in the setting of diminished esophageal function,” he says. The study was published in Surgical Endoscopy.
The investigators evaluated 14 patients with scleroderma who had undergone fundoplication (N = 7) or RYGB (N = 7) for GERD between 2004 and 2016. Patients had a mean age of 54 years and most (11 of the 14) were female. Seventy-one percent of the 14 patients had dysphagia, 86 percent had heartburn and 64 percent had regurgitation prior to surgical intervention. Preoperative mean body mass index (BMI) in the fundoplication group was 24 kg/m2 versus 28 kg/m2 in the RYGB group. Since the procedures were performed, patients in the RYGB group were followed for a median of 19 months versus 97 months for the fundoplication group.
Postoperatively, GERD symptoms improved or resolved in all five patients followed in the RYGB group and in only three of the six patients followed in the fundoplication group, he says, and immunosuppressant use was lessened among more patients in the RYGB group than the fundoplication group. The mean BMI in the RYGB group was reduced to < 24 kg/m2 but remained the same in the fundoplication group. This was not surprising given that RYGB has a well-proven track record for reducing weight in obese patients, as well as effectively treating GERD in very-overweight people. There was no 30-day mortality in either group.
Advertisement
Dr. Kroh suggests that laparoscopic RYGB is a good alternative to fundoplication because it diverts acid and bile away from the esophagus, and doesn’t create a valve, as Nissen fundoplication does, which can potentially cause an impediment to esophageal emptying. Laparoscopic RYGB also separates parietal cells that produce acid and eliminates bile reflux. Traditional fundoplication creates a barrier to decrease reflux of these contents, but also creates a valve that may contribute to poor swallowing in patients with systemic sclerosis.
Both procedures are typically performed laparoscopically, and therefore have benefits of less pain and faster recovery. In addition to eliminating bile reflux and significantly decreasing acid reflux, laparoscopic RYGB maintains a low-pressure zone at the gastroesophageal junction. “This is critically important in patients with systemic sclerosis, who often have impaired esophageal emptying,” according to Dr. Kroh. “The low-pressure zone allows for adequate emptying of the esophagus and may minimize symptoms of difficulty swallowing. This is the advantage of applying this technique to patients with systemic sclerosis and previously has not been described in a larger number of patients, as was done in our study.”
Speaking to the limitations of the study, he notes that although this was a small, retrospective series, it represents the largest characterization of results for this patient population in the literature. “We plan to continue our prospective database and publish additional results on more patients and at further intervals from surgical intervention in the future,” he says.
Advertisement
This and other accruing data may allow for laparoscopic RYGB to be the preferred approach for these patients, to decrease acid and bile reflux and preserve esophageal function. “Often, these patients do not undergo surgical intervention, despite severe symptoms and injury to the esophagus and lungs,” says Dr. Kroh. “With laparoscopic RYGB, however, patients with systemic sclerosis may now have a surgical option to improve the quality of their lives.”
Advertisement
Advertisement

Multidisciplinary framework ensures safe weight loss, prevents sarcopenia and enhances adherence

Study reveals key differences between antibiotics, but treatment decisions should still consider patient factors

Key points highlight the critical role of surveillance, as well as opportunities for further advancement in genetic counseling

Potentially cost-effective addition to standard GERD management in post-transplant patients

Findings could help clinicians make more informed decisions about medication recommendations

Insights from Dr. de Buck on his background, colorectal surgery and the future of IBD care

Retrospective analysis looks at data from more than 5000 patients across 40 years

Surgical intervention linked to increased lifespan and reduced complications