Locations:
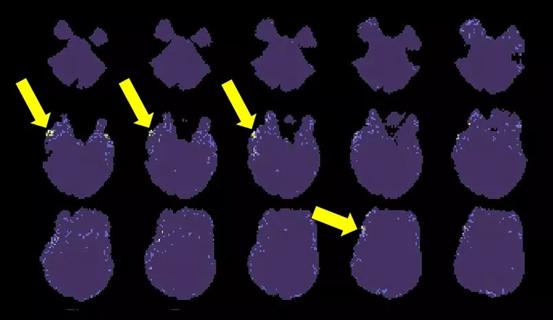
Ultrahigh field strength increases detection sensitivity and temporal resolution
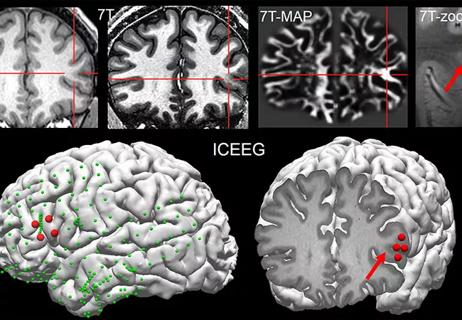
Data suggest substantial findings beyond lower field strengths
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Advertisement