Total hip arthroplasty (THA) is the gold standard treatment for end-stage degenerative hip osteoarthritis, but Cleveland Clinic orthopaedic surgeon Peter Brooks, MD, FRCSC, would like to see that change, at least for one subset of the population – younger, active males.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dr. Brooks is a staff physician in the Orthopaedic & Rheumatologic Center at Cleveland Clinic Indian River Hospital in Vero Beach, Florida, and the senior author of the first large single-surgeon report of long-term outcomes for metal-on-metal (MoM) hip resurfacing in the United States.
“Hip resurfacing was developed as an alternative to hip replacement with younger patients in mind, as they are more likely to outlive their first implant,” explains Dr. Brooks. “This approach preserves more bone and allows for easy hip replacement down the road.”
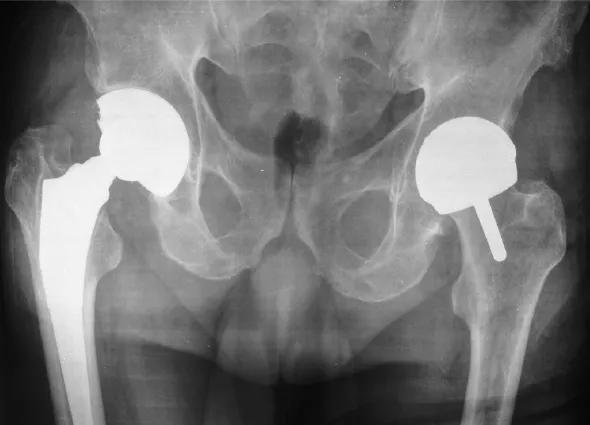
While THA involves removing the entire femoral head and neck and replacing it with a ceramic head and long metal stem set deep into the femur, hip resurfacing requires removing only a few millimeters of bone from the femoral head. It is then covered with a metallic cap attached to a smaller stem drilled into the bone.
“I liken the resurfacing procedure to putting a hat on instead of cutting off the head,” says Dr. Brooks. “For the right patient, it is a much better option.”
Dr. Brooks has performed more than 4,600 resurfacing procedures since MoM hip resurfacing was approved by the FDA in 2006, making him one of the highest volume practitioners in the United States. Most of his cases were performed in Ohio, where he was a staff physician in the Center for Adult Reconstruction in the Department of Orthopaedic Surgery at Cleveland Clinic’s Euclid Hospital and Chief of Surgery, prior to his move to Florida in 2022.
In a MoM hip resurfacing study published in The Journal of Arthroplasty, researchers at Cleveland Clinic determined implant survivorship, analyzed patient-reported outcomes measures, and gauged patient satisfaction. The study included 350 patients (389 hips) who underwent hip resurfacing from September 2006 through November 2009 and were followed a minimum of 10 years. Dr. Brooks performed the hip resurfacings using a modified anterolateral approach with traditional instrumentation.
Advertisement
The median patient age was 53 years, and 258 were male (73%). Out of 389 hips resurfaced, 377 (96.9%) did not require revision surgery. Implant survivorship was 99% among males and 90.9% among females.
“The relationship between sex and survivorship we observed is mirrored in larger multicenter and international studies and the reason this device was withdrawn for females in 2015,” says Dr. Brooks, noting females accounted for 27% of the study population but represented 75% of revisions. “Though implant survivorship is not unreasonable, today I very rarely perform hip resurfacing for female patients.”
Further, of the 350 study participants, 330 (369 hips, 94.8%) reported being satisfied with their surgery. Males had a higher proportion of satisfaction scores and a higher modified Harris Hip Score, which is used to measure pain and functional status following THA. “Our study supports the role of metal-on-metal hip resurfacing as an attractive alternative to total hip arthroplasty for active, younger males,” he says.
In addition to high implant survivorship rates, Dr. Brooks points to other clinical advantages of hip resurfacing over THA. These include lower dislocation rates, less leg length inequality, and more natural biomechanical loading of the femur. “Dislocation is the most common reason for hip replacement revision, but we had zero cases in our resurfacing cohort,” says Dr. Brooks.
Citing another institutional study that looked at midterm outcomes of MoM hip resurfacing versus modern, non-MoM cementless THA in younger patients, Dr. Brooks notes that young males do better with resurfacing than with total hip replacement in terms of both implant survivorship and function.
Advertisement
“With hip resurfacing, our patients are permitted to return to full, unrestricted activities after one year, which is one of the most attractive features of the procedure,” says Dr. Brooks. “Even professional athletes have been able to return to their careers after resurfacing, which does not happen with total hip replacement.”
He also points to the ability to perform easier femoral side revisions, without the need for long stem devices, as another advantage of this approach. “There is an adapter that allows the surgeon to keep a resurfacing socket while changing to a total hip stem, so the second surgery may be even less than a primary total hip,” he adds.
According to Dr. Brooks, one of the more surprising benefits of hip resurfacing is decreased long-term mortality. In a separate study published in the journal Annals of Translational Medicine, Dr. Brooks’ team demonstrated that patients 55 and younger who undergo hip resurfacing have a significantly lower mortality rate than those undergoing THA (1.6% vs. 8.9%).
“The reason behind this mortality benefit is unclear, but it is consistent with previously published large database studies,” says Dr. Brooks.
For example, in a retrospective cohort study out of England, patients with hip osteoarthritis undergoing MoM hip resurfacing had a reduced 10-year mortality rate compared with those undergoing both cemented and uncemented total hip replacement.
“Resurfacing patients are able return to regular physical activities and achieve a more normal stride length and faster walking speeds, which may be a factor at work,” offers Dr. Brooks. “Other studies have demonstrated the occurrence of cerebral microembolisms during THA but not during hip resurfacing, which could be another potential contributor.”
Advertisement
Based on his extensive experience performing hip resurfacings, Dr. Brooks offers up a number of key takeaways about the procedure:
Advertisement
Advertisement

Nonthermal technique reduces bleeding and perforation risk

Standardizing a minimally invasive approach for Barrett’s Esophagus and Esophageal Cancer

PSMA-targeted therapy for metastatic prostate cancer now offered at Cleveland Clinic Weston Hospital

Nationally recognized urologic oncologist offers vision for growth, innovation, and excellence

Noninvasive modality gains ground in United States for patients with early-to-moderate disease

Cleveland Clinic Weston Hospital’s collaborative model elevates care for complex lung diseases

Interventional pulmonologists at Cleveland Clinic Indian River Hospital use robotic technology to reach small peripheral lung nodules

Trained in the use of multiple focal therapies for prostate cancer, Dr. Jamil Syed recommends HIFU for certain patients with intermediate-risk prostate cancer, especially individuals with small, well-defined tumors localized to the lateral and posterior regions of the gland.