Cleveland Clinic nurse educators streamline preparedness training
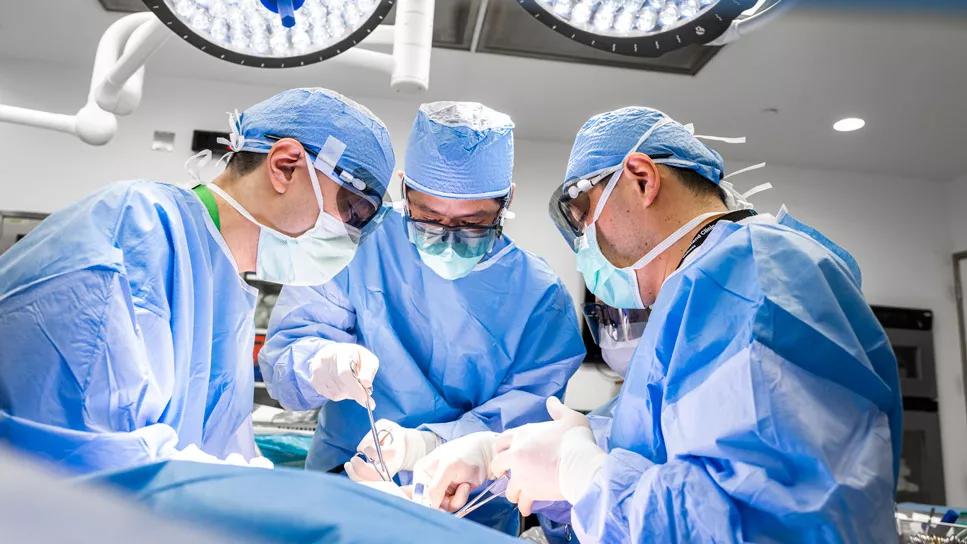
Cardiac tamponade is the rapid accumulation of fluid in the areas surrounding the heart or chest cavity, creating a life-threatening arrhythmia and loss of blood pressure. It doesn’t happen often, but when it does, it may be necessary to perform an emergent bedside sternotomy, an open-chest procedure to remove excess fluid and restore a normal heart rhythm. Nurses may be called upon to act with only minutes to spare when this happens, and those with little OR experience can find themselves thrust into unfamiliar territory: preparing for a surgical procedure.
Bedside emergent sternotomy is what Cleveland Clinic nurse educators call a high-risk, low-frequency event, so training is needed to equip nurses with the competence and confidence to perform well if it happens on their shift. While the procedure takes place more frequently in cardiac ICUs and step-down units, it can happen anywhere in the hospital, so it pays for nurses to have a plan, says Diane Horabik, MSN, RN, a Cleveland Clinic Nursing Professional Development Specialist.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
To that end, Horabik and colleagues Migdalia Serrano-Smith, MSN, RN, VA-BC and Stephanie Sobeck, DNP, RN, NPD-BC, PCCN-K developed training for open-chest procedure preparation.
“Nurses might be called upon to perform this skill, so it’s something that we need to educate them on frequently to keep them current in their practice,” Horabik says. “How well they perform can determine patient outcomes.”
Cardiac tamponade can be triggered by a variety of events, including trauma from a recent medical procedure or from an accident, infection of the pericardial sac, and even CPR. Symptoms can include chest pain, difficulty breathing or rapid breathing, lightheadedness and palpitations, low blood pressure, muffled heart sounds, and jugular vein distention.
Once a code blue is called and caregivers recognize the patient is in cardiac tamponade, the surgical team moves in and the clock is ticking, Horabik says. “The team wants to be inside the chest within five minutes to help relieve the pressure and fix the problem,” she says. It is the nurse’s responsibility to perform the prep work to make that happen.
The surgical process itself is straightforward. Sometimes opening the chest is enough to relieve the pressure and return normal rhythm. If not, fluid may be mechanically suctioned. Administration of intracardiac epinephrine or internal defibrillation may be required. The injury may be sutured or cauterized if the tamponade was caused by trauma or post-operative complications.
For the nurse, however, the key steps need to happen within five minutes:
Advertisement
As simple as it sounds, the training of these steps requires repeating to maintain the skills, the nurse educators say.
The open-chest sequence is taught as part of the team’s HVTI Basics, a course for nurses new to the cardiovascular institute and for new graduate nurses. Resources provided to the nurses include a pocket card containing quick reference information and important phone numbers. Ongoing education on the nursing units also takes place.
“We’ve been teaching open chest for a while, but because the incidence is so infrequent, nurses still felt underprepared,” Horabik says. “We decided to streamline this education and really define the nurses’ role. They’re not actually doing the surgery, but they are setting up for the procedure, and time is of the essence.”
While the steps are minimal and straightforward, preparation for the open-chest procedure can be a source of anxiety.
“It’s an OR procedure being done by caregivers who are not operating room nurses,” Horabik says. “That alone brings anxiety.”
One of the crucial details is knowing how to retrieve equipment quickly, Sobeck says.
“It can be a huge sticking point for the nurse if they don’t know where the open-chest cart is located,” she says. “Some have it directly on their units, while some have to go to a totally different floor to retrieve it. In some cases, they might have to go to different locations within the building to get the sternal saw, which has multiple parts that have to be brought. This is nothing that they would have experienced in their day-to-day nursing operations or even in nursing school.”
Advertisement
The instrument tray also may feel unfamiliar.
“The tray has all kinds of surgical instruments, but the surgeon only needs to use three of them initially,” Horabik says. ”So nurses may feel anxious that they don’t know what equipment is required. We tell them, ‘That’s OK. You’re not an OR nurse. It’s fine to ask the surgeon to point to the instrument they need. ‘“
With proper training and refresher information, however, nurses can be ready. Serrano-Smith and Sobeck both have been on duty at times when patients experienced emergent bedside sternotomy.
“I felt ready for it,” Serrano-Smith says. “The surgical teams show up quickly. You blink an eye and they are there. That’s how quick our response times are. As long as you can locate the equipment and get it where it needs to be quickly, then you have done your work and set things up so that team can take over.”
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader