Study shows ultrasound can be valuable tool for improving patient satisfaction by reducing failed IV insertions
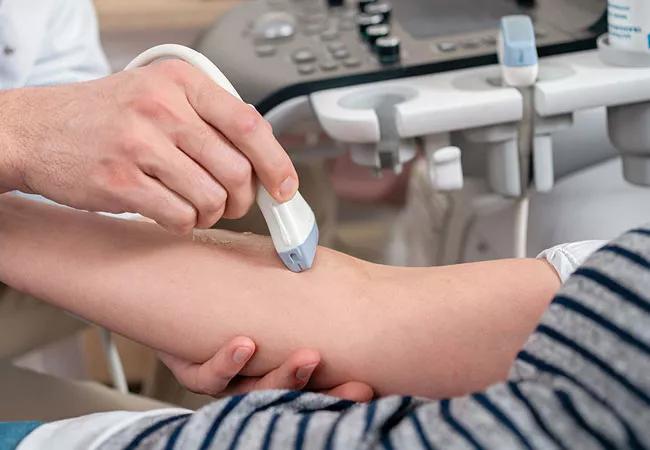
Ultrasound appears to help facilitate peripheral vascular access in hospitalized adult patients, according to a study led by Cleveland Clinic nurse researchers. In assessing factors associated with IV access success in a series of 394 medical-surgical patients at Cleveland Clinic, ultrasound use was an important predictor of first-attempt and overall peripheral IV access success, according to lead investigator Andrew Callahan, BSN, RN, Assistant Nurse Manager. He is scheduled to present the data at the Cleveland Clinic Nursing Research Conference in late April.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“We found that ultrasound was more successful than the standard landmark technique in enabling peripheral vascular access,” says Callahan.
Ultrasound was used in 227 of the 394 (57.6%) IV access attempts evaluated in the study. When asked why he wanted to study ultrasound access, Callahan explained: “Landmark techniques are important, but I thought there had to be a better way to insert IVs. I also met an elderly patient with cancer who told me that there were many nurses who assessed her arm veins, attempted to insert an IV and failed; she was frustrated.
“I listened to her story and wondered if we could use ultrasound for every patient. When researching peripheral IV access in adults, I found papers in the peer-reviewed literature that showed the effectiveness of ultrasound guidance for placing IVs. I presented findings from the ultrasound literature review to my manager, who indicated that our research department was thinking about studying difficult IV starts.”
Study participants consisted of medical-surgical patients who required IV access and nurses who attempted IV access on multiple nursing units. Nurses agreed to complete case reports that described their perceptions about more than 30 factors associated with successful IV insertions. Data were also collected from medical records.
Of the cohort assessed, the first-attempt success rate was 20% lower than the overall IV access success rate, which was over 80%. In multivariable modeling, multiple factors were associated with first-attempt and overall IV access success. Of the factors that correlated to first-attempt IV access, two were related to patient veins, four were related to nurses’ experience and perceptions about IV access, and one was associated with patient verbalization of difficult IV access. In addition, vein visibility and palpability were associated with overall IV access success.
Advertisement
“Since use of an ultrasound device was an important predictor of success, the hope is to facilitate nurse autonomy by teaching nurses how to use the imaging modality to reduce the number of IV attempts their patients require. Fewer attempts can decrease supply usage, nursing time and other resources needed to establish IV access,” Callahan says. “Patient satisfaction is also important. When I am using the ultrasound to start peripheral access, patients seem more at ease.”
Since overall success in IV access did not reach 100%, future research findings may be used to justify the creation of a systemwide vascular access team, he adds.
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader