Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3e54dfff-8040-479d-b5fd-52644e43c85d/23-NEU-4052327_deep-brain-stimulation-of-dentate-nucleus_650x450_jpg)
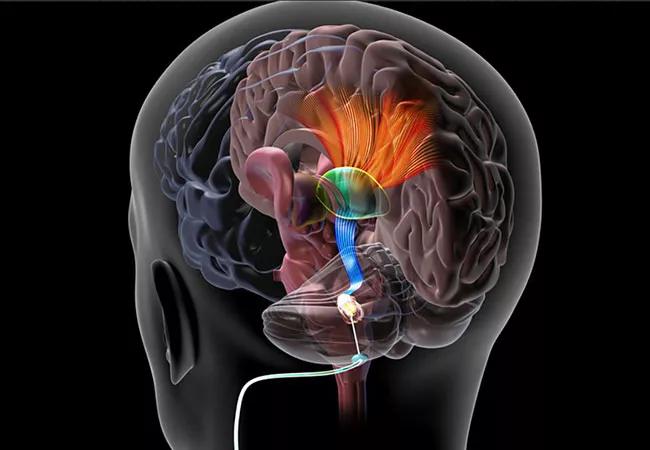
deep brain stimulation
Deep brain stimulation (DBS) has become the most commonly performed surgical treatment for Parkinson’s disease (PD) since its approval by the FDA for use in patients with movement disorders in the late 1990s and early 2000s.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
According to an analysis of the National Inpatient Sample database published last year, PD is also the most frequent indication for DBS, accounting for 67% cases in the United States. Other FDA approved indications include essential tremor, dystonia, obsessive-compulsive disorder, and epilepsy.
“DBS is not a curative procedure but combined with medication therapy it serves as an important treatment option to lessen symptoms and enable patients with Parkinson’s to perform activities of daily living,” says Tarannum Khan, MD, a board-certified neurologist with Cleveland Clinic Weston Hospital who specializes in movement disorders.
Dr. Khan joined Cleveland Clinic in Florida in 2006 and has seen the important progress made in caring for patients with PD, including the advancements in DBS. Hundreds of patients have undergone the procedure at Weston Hospital since it was first offered in 2008.
DBS involves stereotactically implanting a lead and electrodes in the brain and a pulse generator under the patient’s collarbone, and then connecting them via an extension wire tunneled under the skin. Electrical signals are delivered to specific areas of the brain important for motor control to make neurons more active, relieving PD symptoms.
“The pulse generator settings are fine-tuned to achieve the best possible effects for the patient, finding a balance between the motor and cognitive symptoms of the disease,” explains Dr. Khan. She notes there is both a clinician programming system and a patient programming system so that patients can make adjustments at home.
Advertisement
DBS does not halt disease progression but it does provide durable symptom relief. A 2019 study showed that 75% of participants followed for over 10 years felt DBS helped them manage their Parkinson’s symptoms.
“DBS works best when used along with medications,” adds Dr. Khan. “The combination often means patients need lower medication doses and subsequently experience fewer side effects.”
DBS was first approved by the FDA in 1997 to treat essential tremor and tremor associated with PD by targeting the ventral intermediate nucleus of the thalamus (VIM). Indications were expanded in 2002 to include treating advanced Parkinson's symptoms, including rigidity and dopamine-induced dyskinesia, by stimulating the subthalamic nucleus (STN) or the internal segment of the globus pallidus (GPi). The following year the FDA also granted a Humanitarian Device Exemption allowing the use of DBS in the GPi and STN for dystonia.
Most recently, DBS was approved in 2016 for use in the earlier stages of PD. “This was very good news for patients because a growing body of research indicates younger patients who are earlier in their disorder are more likely to have a better outcome,” says Badih Adada, MD, Chair of the Neurosciences Institute for Cleveland Clinic in Florida and Chair of the Department of Neurosurgery for Cleveland Clinic Weston Hospital.
More than 200,000 people worldwide have had a procedure to implant a DBS device and about 12,000 DBS surgeries are performed each year, according to industry estimates.
Advertisement
Since joining Weston Hospital in 2012, Dr. Adada has used DBS to treat patients with PD, essential tremors, and dystonia. “The DBS surgery I perform today is very different from what was performed earlier in my career,” he notes.
In 2016, Cleveland Clinic was the first hospital in South Florida to use the ROSA robotic system to perform cranial operations, including for epilepsy and brain tumor surgeries and DBS.
“With the robotic system, I can make sub-millimetric adjustments during lead insertion to achieve a high degree of accuracy for electrode placement,” Dr. Adada explains. “This is essential for patient safety and successful treatment.”
He also performs asleep DBS with the patient under general anesthesia and uses advanced intraoperative and postoperative imaging to confirm electrode positioning. Traditionally, DBS is performed while the patient is awake so that intraoperative test stimulations may be performed to confirm correct electrode placement.
Another recent advancement in DBS technology is the development of directional leads that provide greater control over stimulation versus conventional ring-shaped DBS leads that produce a circular electrical field.
“By customizing the size, shape and direction of stimulation, we can improve the therapeutic window and optimize symptom relief,” says Dr. Adada.
This technology also has been combined with new sensing technology built into the pulse generator to capture and record brain signals. The signals are then correlated with patient-recorded symptoms, side-effects, or medication intake to better personalize the neurostimulation treatment.
Advertisement
“This is the next step toward a closed-loop DBS system that will allow self-tuning stimulation instead of the constant stimulation, or open-loop system, currently used,” adds Dr. Adada.
According to the Parkinson’s Foundation, nearly one million people in the United States are living with PD, and 90,000 new diagnoses are made each year, making it the second most common neurodegenerative disorder following Alzheimer’s.
But not everyone with PD is a good candidate for DBS. A 2015 study estimated that only about 2% of people who qualified for the treatment actually received it.
DBS is approved for people who have had PD for at least four years and have motor symptoms not adequately controlled with medication. “These individuals may have significant episodes when their medication is less effective or they may experience uncontrolled, involuntary movements,” explains Dr. Khan.
As a Parkinson’s Foundation Center of Excellence, Cleveland Clinic in Florida employs a multidisciplinary approach to care for patients with PD. The team consists of neurologists with training in movement disorders, neurosurgeons, neuropsychologists, physical therapists, occupational therapists, speech therapists, nurses and social workers.
“We work closely to choose appropriate patients for DBS based on brain imaging and thorough neuropsychological evaluations,” adds Dr. Khan, who also leads the Multidisciplinary Clinics for Parkinson’s Disease hosted monthly in Weston.
“Our dedicated clinic days allow patients with PD to have grouped, back-to-back appointments with a neurologist and other care team members to address their unique physical, emotional, cognitive, and rehabilitation needs,” she says.
Advertisement
For more information, visit Cleveland Clinic Florida ConsultQD. Subscribe to the Florida Physician Newsletter.
Additionally, follow us on X (formerly Twitter), Facebook, and LinkedIn.
Advertisement
Evidence shows early evaluation improves survival and quality of life – yet many eligible patients are referred too late
2026 ADA Standards of Care promote holistic, multisystem management
Cleveland Clinic nephrologist in Florida addresses changes in clinical practice
Surveillance platform supports community clinicians and public health monitoring
Benefits include improved clinical outcomes and lower healthcare costs
Pulmonary endarterectomy plays central role in era of multimodal therapy
Evidence supports safety and efficacy of surgery in patients aged 80 years and older
One in four experience reduced anxiety