Team provides coordinated, multidisciplinary, patient-centered care for high-risk pregnancies involving a heart defect
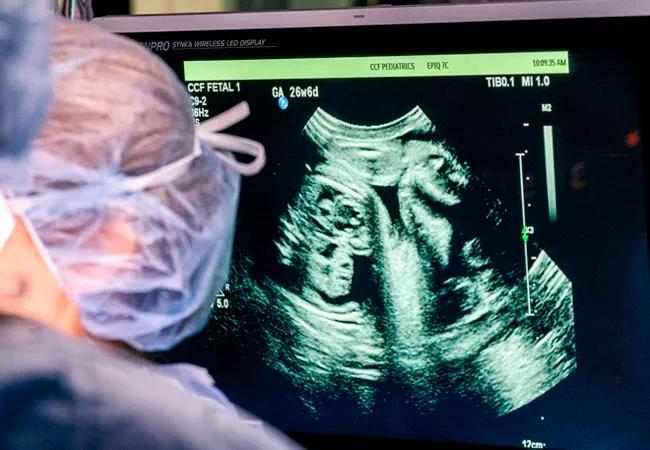
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c6c91b5d-9c0e-4785-8437-abc2426d9e59/22-CHP-3174213-CQD-Najm-Erenberg-FetalCardiacCareProgram650x450-1_jpg)
22-CHP-3174213 CQD-Najm-Erenberg-FetalCardiacCareProgram650x450 (1)
When a potential fetal cardiac defect is identified during a screening ultrasound, referral to Cleveland Clinic Children’s Fetal Cardiac Care Center should be the next step.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Our role is to see that the pregnancy goes well and that the fetus remains healthy while we plan for the care the baby will need after it is born,” says Francine Erenberg, MD, one of eight pediatric/fetal cardiologists on staff and a Co-Director of the Fetal Care Center. She and her colleagues see patients in clinics throughout Northeastern Ohio, as well as on Cleveland Clinic’s main campus.
“We put our patients at the center and coordinate care with all the necessary medical and surgical subspecialties. Our goal is to achieve the best possible outcome for both the mother and baby, while offering the counseling, support and information families want and need,” she says.
At the core of the Fetal Cardiac Care Center is the team of experienced fetal/pediatric cardiologists, congenital heart surgeons and fetal, pediatric and obstetrical anesthesiologists, who are well positioned to care for any congenital heart problems they find.
Because some patients are referred due to a genetic or non-cardiac abnormality that increases the risk of a congenital heart defect in the fetus, the fetal cardiac specialists will coordinate care with maternal-fetal medicine specialists, high-risk obstetricians, neonatologists, and the full complement of pediatric medical and surgical subspecialists, as needed.
“We confirm the diagnosis with an echocardiogram focused on the heart and discuss the findings with the parents. Then we introduce them to the other services they will need,” says Dr. Erenberg.
Babies with congenital heart defects typically survive until birth. According to Hani Najm, MD, one of four pediatric and congenital heart surgeons on staff and department chair, the minutes and hours immediately following birth are the most critical time.
Advertisement
“The opportunity to study a congenital heart defect in advance allows me to plan my surgical approach and decide what, if anything, we can do before the baby is born,” he says.
Members of the Fetal Cardiac Care Center team work together and with the parents to prepare for the birth.
“Outcomes are better when we can have teams of specialists, the ICU and everything the baby may need ready and available from minute one,” says Dr. Erenberg. “There is no delay in starting medical care while we make a diagnosis.”
The timing of congenital heart surgery is about to undergo a sea change. The mantra, “how quickly can we operate?” is gradually becoming “What can we do before the baby is born?”
“The neonatal period is the most complex for cardiac intervention,” says Dr. Najm. “If we can delay surgery for one or two months after birth until the period of high complexity has passed, the baby will have gotten feedings, is breathing normally and is stronger.”
Fetal heart surgery—already available at Cleveland Clinic Children’s—will make this possible.
“It is so exciting. If we can keep a fetus in the womb by doing an intervention so that we don’t have to operate in the first few weeks of life, it will be an incredible gain,” he says.
Although Darrell Cass, MD, joined the staff in 2017 as Director of Fetal Surgery, he has had only a handful of opportunities to collaborate with Dr. Najm. The most notable case was the successful removal of an intrapericardial teratoma causing massive pericardial effusion in a 27-week-old fetus.
Advertisement
Dr. Najm foresees tapping Dr. Cass’ skills and experience in the future; for example, in a fetus with hypoplastic left heart syndrome with intact atrial septum. “These babies develop severe pulmonary hypertension, because the pulmonary veins are obstructed, the mitral valve is closed and the blood has nowhere to go.
“If we can get comfortable doing surgery in the womb on these high-risk babies, and we can avoid doing surgery right after birth, it will change lay of the land,” he says.
Advertisement
Advertisement
A new CME opportunity in Chicago, May 15-16
Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner
Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve
Reproducible technique uses native recipient tissue, avoiding risks of complex baffles
A reliable and reproducible alternative to conventional reimplantation and coronary unroofing
Program will support family-centered congenital heart disease care and staff educational opportunities
Case provides proof of concept, prevents need for future heart transplant
Pre and post-surgical CEEG in infants undergoing congenital heart surgery offers the potential for minimizing long-term neurodevelopmental injury