Careful management of adverse intraoperative events may reduce morbidity and mortality

The use of hyperthermic intraperitoneal chemotherapy (HIPEC) during cytoreduction surgery (CRS) for epithelial ovarian cancer (EOC) can present metabolic and physiologic challenges that may alter the administration of intraoperative anesthesia, according to the findings of a new study presented at the 2019 Society for Gynecologic Oncology Annual Meeting in Honolulu, HI.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The retrospective review was directed by, Robert DeBernardo, MD, a gynecologic oncologist in the Department of Gynecologic Oncology and Director of Minimally Invasive Surgery in Cleveland Clinic’s Ob/Gyn & Women’s Health Institute. Dr. DeBernardo’s team retrospectively reviewed the cases of 64 women with diagnoses of EOC undergoing CRS with HIPEC between 2010 and 2018.
“We noticed some people develop acidosis when we started giving HIPEC, while others became hyperglycemic,” Dr. DeBernardo says. “There appeared to be a correlation with outcomes, which we sought to explore further.”
HIPEC is a technique that delivers chemotherapy directly into the abdominal cavity, while the patient is still in the operating room, once resection is complete. Tubing is placed in the abdomen and chemotherapy—usually cisplatin—is circulated at 42° C.
“Once the cancer is removed, we infuse the abdomen with the drug for 90 minutes, reconnect the intestines if the bowel was involved in the surgery, and then close,” explains Dr. DeBernardo.
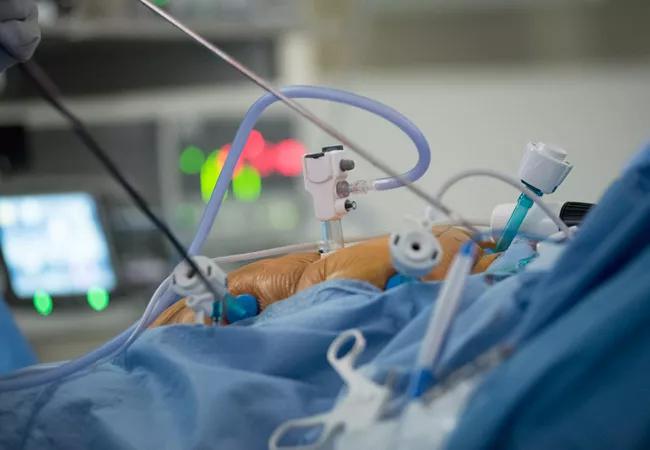
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/14a862e6-ae5d-4765-95e7-f386baf5b3f0/HIPEC_650x450_jpg)
HIPEC perfusion: Following surgical removal of all gross cancer, tubing is placed in the abdomen and the patient is closed. An assistant at the bedside gently shakes the abdomen and the heated chemotherapy continually circulates for the prescribed time period.
HIPEC improves the rates of progression free survival and overall survival; however, the patient is kept under anesthesia for an additional 90 minutes, allowing us to expose the peritoneum to a very high concentrate of drug,” Dr. DeBernardo continues. “This added surgical stress can be hard on patients. We sometimes refer to this as a high-risk, high-reward procedure.”
Advertisement
A vast majority of the patients experienced electrolyte abnormalities (96.9%) and required intraoperative pressor support (92.2%). Notably, 80.6% of patients developed hyperglycemia (>200 mg/dL) and 77.4% developed hypokalemia (3.5 mmol/L). Slightly less than half of the patients developed hypomagnesemia (<1.7mmol/L). Intraoperative insulin was administered in 60.9% of patients, and 60.8% received blood transfusions.
Of the 64 patients, 81.3% developed lactic acidosis intraoperatively, though there were no statistically significant differences between those with or without lactic acidosis in terms of outcomes, such as length of stay, postoperative adverse events, ICU admission, etc.).
“As we noticed a trend developing in the data, we became much more aggressive in our management of hyperglycemia and acidosis in the operating room. This, combined with the retrospective nature of this study, make it difficult to determine whether our own intraoperative interventions impacted the results.”
“When performing HIPEC procedures, care should be taken to monitor and maintain blood glucose, calcium and magnesium levels,” continues Dr. DeBernardo. “We put an arterial line in all of our patients so we can measure blood gas at any time during surgery, and we usually get results back within 5-10 minutes. We also noticed that glucose, particularly, as well as pH, are affected when we start the infusion. With acidosis, sometimes we adjust ventilator, or give bicarbonate. Careful management is key.”
Advertisement
Age, performance status and disease locations are all factors in selecting appropriate patients to receive HIPEC. “Not everyone is a great candidate for HIPEC,” Dr. DeBernardo explains. “If we can’t surgically remove all the cancer, then there will be no measurable benefit. A good candidate is one who is relatively healthy, and able to survive the treatment (i.e., not too frail) and move on to chemo afterward. We have also found HIPEC to move the survival curve dramatically for patients with platinum resistant ovarian cancer, for whom prognosis is usually quite poor. It’s a small group, but they fit in the high-risk, high-reward category: HIPEC may work for them when very little else does.”
Advertisement
Advertisement

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors

Study shows significantly reduced risk of mortality and disease complications in patients receiving GLP-1 agonists

Structured interventions enhance sleep, safety and caregiver resiliency in high-acuity units

Addressing rare disease and challenging treatment course in an active young patient