Infant with complex congenital heart anomalies thriving after biventricular circulation is restored
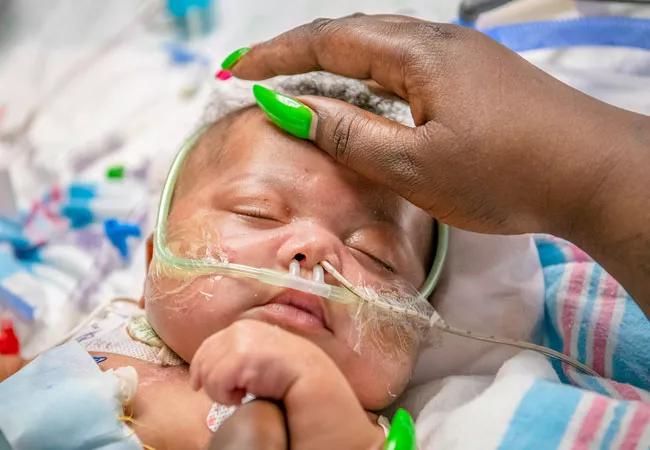
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b9bf4994-58f7-4241-a725-05ba4e413c01/21-CHP-2235358-CQD-650x450-Najm_jpg)
21-CHP-2235358-CQD-650×450-Najm
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
On May 19, 2021, we admitted a 2-month-old born with a double-outlet right ventricle. In this complex congenital heart anomaly, the pulmonary artery and aorta emerge from the right ventricle, and the left ventricle has no outlet. A ventricular-septal defect (VSD) also was present. Typically, VSDs are found below the aortic or the pulmonary valve. In this case, it was remote from either valve, which eliminated the possibility of a traditional repair. The infant had been on a ventilator since birth and was deteriorating rapidly. When his providers in the other center were unable to agree on a treatment plan, the parents requested their child be transferred to Cleveland Clinic Children’s.
In cases like this when the left ventricle cannot be leveraged to pump blood to the body, surgeons commonly create a univentricular heart circulation by combining both ventricles into one. As an alternative, I elected to perform a ventricular switch, a procedure I developed to restore biventricular circulation and avoid the collateral damage that accompanies univentricular circulation.
On June 4, I diverted the infant’s lung return to the morphologic right ventricle, making it the systemic ventricle, closed the VSD and connected the left ventricle to the pulmonary artery via a conduit, activating it and sending blood to the lungs (see simulation below). The surgery went well, and the infant was transferred to the pediatric intensive care unit (PICU), where he is being weaned off narcotics and total parenteral nutrition.
Advertisement
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/L4QKl3V7Iyc?feature=oembed)
Ventricular Switch Heart Procedure
The ventricular switch procedure is not designed for a specific anomaly, but enables us to correct a variety of anomalies that prevents the left ventricle from pumping to the body and the right ventricle from pumping to the lungs. The principles of this procedure have been previously detailed.
The procedure is not standardized and may differ greatly from patient to patient. However, the universal concept is to reroute the arteries so that the right ventricle pumps to the body, and the left ventricle pumps to the lungs.
Planning for these complex procedures is greatly facilitated by 3D printing of the heart. Having an exact replica of the heart enables me to study the heart closely and plan the operation (see image below). Then I simply execute my plan in the operating room.
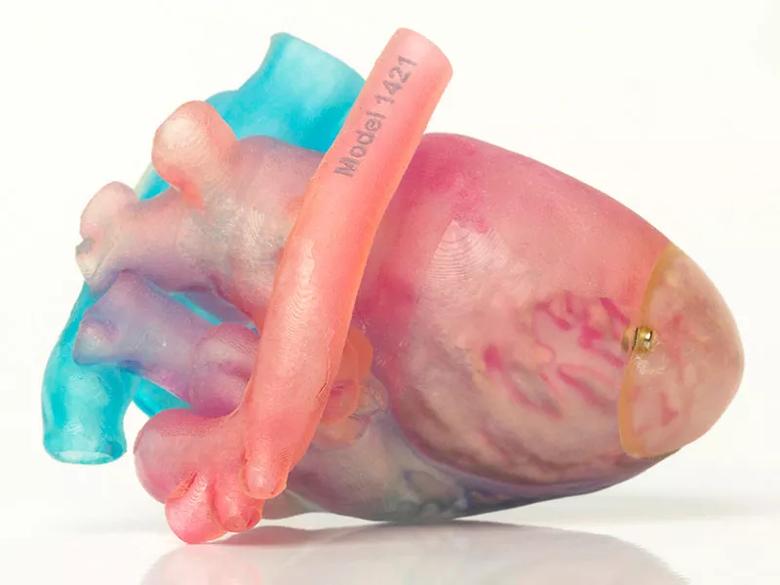
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b6de5e13-1667-456b-afaf-156b2fd88a8d/21-CHP-2235358-CQD-805x600-Najm-inset_jpg)
In all previous patients, I performed the procedure in a staged fashion beginning when the child was larger and better able to tolerate the complex intracardiac routing. This was the first time I performed it in a single operation, and in an infant so young. I felt there was no choice. This 3-kilogram baby was cyanotic, had oxygen saturation levels in the 50s or 60s and was in heart failure. Doing the procedure in stages would have required treating his heart failure with a pulmonary band, but this would have decreased blood flow to his lungs and worsened his cyanosis. I felt he would not survive this palliative procedure and decided to perform the entire procedure at one time.
I expect this child to have a fairly normal life. He has two ventricles pumping to the body. The conduit connecting the ventricle and pulmonary artery will need to be replaced in three to five years, but that is not a concern.
Advertisement
In middle to late adulthood, his right ventricle may—and I emphasize “may”—fail. This happens to patients born with the right ventricle connected to the aorta: They could develop heart failure because the right ventricle eventually wears out. If this occurs in this child, it will be a matter of managing his heart failure, and we have excellent options for this. He will not be at risk for failure of a univentricular heart, which is catastrophic and results in multiple organ failure.
When a patient with complex heart anomalies has two ventricles, do not ignore the second ventricle, even if it is moderately hypoplastic. It can still be used to establish an effective biventricular circulation, which is always preferable to univentricular circulation.
About the author: Dr. Najm is the Chair of Pediatric and Congenital Heart Surgery and Executive Co-Director of the Pediatric and Adult Congenital Heart Center at Cleveland Clinic.
Advertisement
Advertisement
Join us in Florida this winter for a long-standing CME favorite
International experts provide a guide for rapid decision-making focused on transcatheter options
Join us in New York Dec. 6-7 for broadened version of a CME crowd-pleaser
New study illuminates mechanical underpinnings of secondary leaks
Introducing Prajwal Rajappa, MD, MS, Director of Pediatric Precision Oncology
The one-stop THRIVE clinic addresses renal, psychosocial, educational and other challenges alongside cardiac surveillance
Large series confirms early and long-term survival advantages over partial pericardial resection
Intracardiac echo mapping of para-septal fat pads provides fast, accurate and radiation-free targeting