Complex fix requires methodical approach and extensive experience
By Sherief Shawki, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A 48-year-old woman was referred to Cleveland Clinic from an outside hospital four weeks after she had undergone ileal pouch-anal anastomosis and diverting loop ileostomy for familial adenomatous polyposis (FAP). She now reports that she has liquid stool coming out of her vagina accompanied by severe pain.
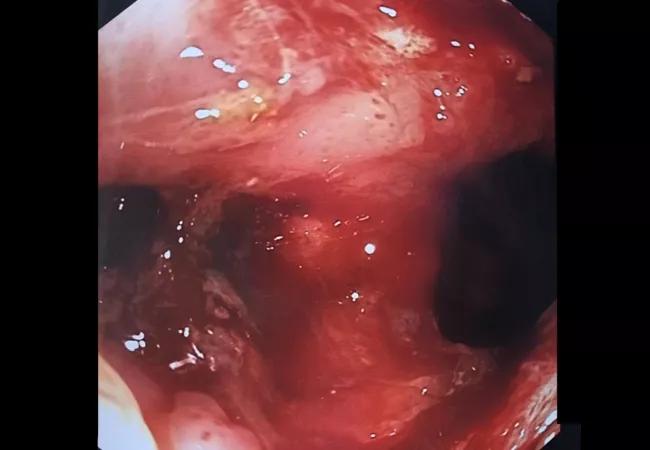
Patient records from the external hospital were reviewed. Examination under anesthesia at this time found bile in her vagina and revealed that the J-pouch was connected to the rectum as well as the vagina. There was no evidence of sepsis. We sutured close the efferent limb of the existing diverting loop ileostomy to prevent passage of bile into the vagina.
Eight months later, exploratory laparotomy was performed. After extensive lysis of adhesions, we were able to identify anatomy and pathology, and the previous findings were confirmed. The old pouch was dissected from the pelvis, and the pouch-rectal/vaginal anastomosis was taken down. The pouch was deemed nonreusable. An abscess was found deep in the pelvis and debrided.
As the anal sphincters appeared intact and functional preoperatively, a new ileal J-pouch was constructed and the vagina was reconstructed. Lengthening techniques were used to ensure a tension-free, hand-sewn pouch-anal anastomosis after rotating the mesentery of the pouch anteriorly to minimize the risk of fistulization with the suture line of reconstructed vagina. A new diverting loop ileostomy was created.
A few months later, the patient underwent reversal of her loop ileostomy and was able to gain full use of the new pouch.
Advertisement
The patient recently celebrated her first anniversary with her new pouch. She was doing well and reported good continence. Pouchoscopy showed an unremarkable pouch.
Restorative proctocolectomy and ileal pouch-anal anastomosis is the optimal surgical procedure for ulcerative colitis, FAP and select patients with Crohn’s disease to maintain continuity of the GI tract. (For additional background, see previous Consult QD post here).
Redo surgery of a failed pouch can save many patients from pouch excision and permanent ileostomy. Considerable thought, planning and care are especially warranted for these procedures that have potential outcomes so critical to a patient’s quality of life.
This case highlights several key points:
Properly constructing anastomoses is critical. Ileal pouch-anal anastomosis surgery fails in about 15 percent of cases, mainly due to technical errors. For both primary surgery and redos, operative planning, step-wise technique, good exposure and visualization are essential to ensuring that the correct structures are connected.
Reconstruction is a complex undertaking. Redo surgeries are big operations and must be performed in an open fashion. They require patience and a strategic, methodical approach to ensure best outcomes. Thorough preoperative evaluation, planning and timing of each step are critical.
Experience is needed. Reoperative corrective pelvic surgeries, especially pouch redos, should only be performed at a high-volume center with considerable expertise in performing complex gastrointestinal surgery. The availability of an experienced multidisciplinary team, not only during surgery, but pre- and postoperatively, help ensure best outcomes.
Advertisement
Salvage surgery is usually successful when performed at experienced institutions. Data from hundreds of patients with reconstructive surgeries of failed ileal pouch-anal anastomoses at Cleveland Clinic (reported in the Annals of Surgery and in the Diseases of the Colon & Rectum), reveals a 75 to 80 percent success rate. Patients with Crohn’s disease had a much lower success rate, only 37 percent. Pelvic sepsis was the primary indicator of failure.
Redos involved either creation of a new pouch or retention of the original pouch. Both local perineal and abdominal approaches yielded successful results; the choice of procedure should be determined on a case-by-case basis. Patients required a mean of two procedures to achieve pouch salvage, and there was no association between the number of pouch salvage procedures and failure.
Finally, surgeons at Cleveland Clinic are always available to other hospitals for inservice training or guidance on difficult cases.
Advertisement
Advertisement

Multidisciplinary framework ensures safe weight loss, prevents sarcopenia and enhances adherence

Study reveals key differences between antibiotics, but treatment decisions should still consider patient factors

Key points highlight the critical role of surveillance, as well as opportunities for further advancement in genetic counseling

Potentially cost-effective addition to standard GERD management in post-transplant patients

Findings could help clinicians make more informed decisions about medication recommendations

Insights from Dr. de Buck on his background, colorectal surgery and the future of IBD care

Retrospective analysis looks at data from more than 5000 patients across 40 years

Surgical intervention linked to increased lifespan and reduced complications