Cleveland Clinic Children’s implemented an automated color-coded system to escalate timely care to prevent patient deterioration
At Cleveland Clinic Children’s, Blue’s Clues is more than a popular children’s television series.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“For us, ‘blue’ is a clue to pause,” says Amrit Gill, MD. “That’s a signal for our caregivers to look for clues that might lead to a patient’s rapid decline.”
As a pediatric hospitalist and Cleveland Clinic’s Associate Chief Safety Officer, Dr. Gill knows that earlier detection of deteriorating health leads to quicker intervention and better patient outcomes.
Considering that 10% of hospitalized pediatric deaths are preventable, clinicians rely on patient monitoring tools to detect declining health.
Pediatric early warning systems (PEWS) did just that — alert caregivers to early signs of patients’ clinical deterioration prompting timely interventions. Nurses completed this manual scoring process every four hours after new vital signs were taken.
Despite using PEWS for several years, Dr. Gill, Carla Anderson, APRN-CNS, and Jane Hartman, APRN-CNP, knew there were limitations.
Ms. Anderson describes the problem: “This type of monitoring was subjective and prone to errors. Plus, there’s no visibility beyond the nurse who recorded the patient’s score. There’s no immediacy for timely interventions until it’s potentially too late.”
Ms. Hartman adds, “We know that patients don’t suddenly deteriorate, but it was often the case that we recognized it all of the sudden. We knew there had to be a better way to care for these vulnerable patients.”
To move past these limitations, the team reviewed research, worked with the Children’s Hospitals’ Solutions for Patient Safety* network and considered existing scoring tools. Among their findings was Cleveland Clinic’s automated adult scoring tool, Vital Scout™.
Advertisement
“Vital Scout™ is a very sophisticated tool with proven outcomes, but our patients required a more precise scoring system,” says Dr. Gill. “We also wanted an extra layer of protection by engaging caregivers earlier in the process.”
This reality led them to clinical systems analyst Kris Kormos.
“Our pediatric caregivers needed more than PEWS,” says Mr. Kormos. “The goal was an automated tool that would signal a patient’s potential risk and immediately bring someone to the patient’s bedside to check on their status.”
Similar to Vital Scout™, the pediatric tool — Situational Awareness Virtual Electronic Scout (SAVES) — is an embedded system within the electronic health record (EHR) that translates designated vital sign values into a color-coded risk stratification score.
Using the existing technology, Mr. Kormos applied logic and rules to generate visual cues that increased situational awareness.
Dr. Gill describes situational awareness as the ability to use objective criteria, a “gut feeling” and critical thinking to recognize the current state as well as anticipate and mitigate risks.
“Honing these skills strengthened our communication and accountability.” Dr. Gill adds, “No matter the role, we have a shared commitment and responsibility to recognize and respond to changing circumstances.”
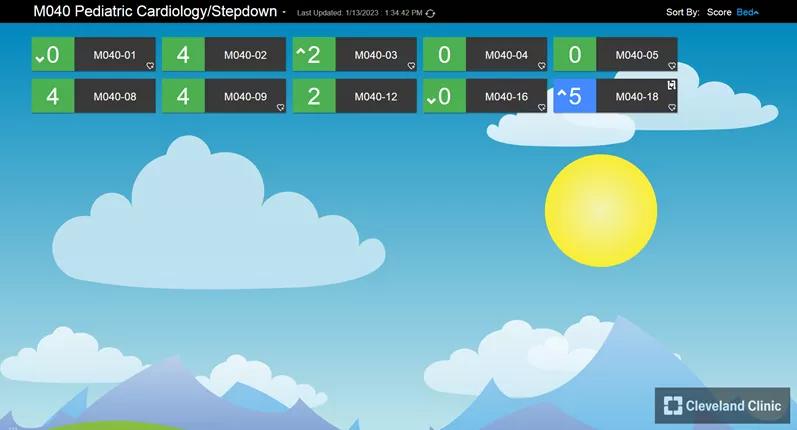
The color-coded scoring system provided visual cues that heightened situational awareness. Similar to a stoplight, green is good, blue signals a clue that something might happen, yellow is an opportunity to mitigate risk and red means immediate action.
Advertisement
For a broader reach, the color-coded scoring appears on every screensaver throughout the units. This increased visibility allows any caregiver to access the patient’s vital signs and intervene as needed.
Ms. Hartman, who recently retired from Cleveland Clinic recalls the benefits: “Reviewing our patients’ status was the first thing I did when I got in to the office. With a quick glance at my computer’s screensaver, I instantly knew which patients needed immediate attention based on their color status.”
“From the screensaver, a simple click into a patient’s EHR gives caregivers access to embedded quick links to communicate and document their assessment and next steps. These details are visible in one report, so they don’t have to jump around the chart looking for vital information,” explains Mr. Kormos.
“We’ve noticed a sharp decline in patients reaching red status since implementing SAVES,” says Dr. Gill. “This exceptional progress has now expanded to other units throughout our health system.”
Amy Cox, a clinical informatics nurse, recently supported the launch of SAVES at two regional hospitals and Cleveland Clinic Children’s Hospital for Rehabilitation. She prepped the care teams prior to go-live and continues to offer support.
“Being on site during the go-live provided quick clarification and guidance,” says Ms. Cox. “This support is ongoing to reinforce the appropriate workflow and encourage feedback. The input from caregivers is imperative to validate SAVES’ efficacy.”
The SAVES tools is not a static program. The team’s step-by-step approach requires consistently evaluating caregiver input, patient outcomes and data to validate the tool’s effectiveness.
Advertisement
Ms. Anderson says, “It’s been an evolving, iterative process to continuously fine-tune the scoring parameters. Caregiver feedback is constantly driving us to validate the current system and make adjustments as needed.
“Hearing from our caregivers resulted in using a percentage change-based score that automated adjustments to reach patients’ “normal” values,” says Mr. Kormos. “For example, we switched the pulse oximetry scoring to capture the last three values to more accurately recognize gradual deterioration.”
Ms. Anderson shares, “The best way to learn how to make anything better is to adapt and continue to improve — so that’s what we’ll keep doing. That’s what our patients deserve.”
Dr. Gill agrees: “Raising a child takes a village and the same applies to caring for our patients. Together, with caregiver and parent input, we remain focused, alert and attune to providing exceptional, safe care. Everyone has a voice and everyone is valued.”
*In 2009, Cleveland Clinic Children’s joined the Ohio Children’s Hospitals Solutions for Patient Safety (OCHSPS) network to focus on quality improvement initiatives to prevent patient harm. Now known as the Children’s Hospitals’ Solutions for Patient Safety, the network includes more than 145 children’s hospitals working together to reach zero harm.
Advertisement
Advertisement

Cleveland Clinic’s approach to improve care transitions and patient safety

Care managers ensure patients return home to recuperate with the right support

Maintaining patients' home medication regimens looms large, study suggests

Automating routine medical coding tasks removes unnecessary barriers

Digital “tripwires” detect and respond to malicious activity, boosting cybersecurity maturity

Effective provider training strategies incorporate multi-modal delivery

Thoughtful collaboration, data-driven decisions and effective change management lead to significant savings

A thoughtfully designed program to elevate participants’ leadership potential