New research identifies a direct functional link between creeping fat and muscle

Investigators at the Cleveland Clinic are exploring the possibility that blocking “creeping fat” may in the future help to reduce stricture formation in Crohn’s disease.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Crohn’s disease starts with inflammation that progresses over time into fibrosis and stricture formation in the intestine. That ensuing luminal narrowing drives obstructive symptoms in patients, including cramping, dietary changes and abdominal pain after eating.
Mesenteric fat wrapping around the intestinal wall in people with Crohn’s disease was first identified and dubbed “creeping fat” nearly a century ago. However, only in recent years has the phenomenon come to light as a potentially major factor in the development of strictures and bowel obstruction.
Currently, most long-term therapies for the strictures are mechanical, either endoscopic dilatation or resection. “There’s a strong need to find novel therapies because more than half of patients with Crohn’s disease are affected by strictures in their lifetime,” says lead investigator Florian Rieder, MD, vice-chair of Cleveland Clinic’s Department of Gastroenterology, Hepatology and Nutrition, Digestive Diseases and Surgery Institute.
In a series of in vitro and in vivo experiments described at the Digestive Disease Week conference, Dr. Weiwei Liu, Dr. Rieder and colleagues identified mechanisms through which the creeping fat induces hyperplasia of the smooth muscle cells leading to stricture. “The luminal narrowing of the gut the patient’s experience in structuring disease for the majority are caused by a thickening of the muscle layer, not by accumulation of the scar tissue,” Dr. Rieder explains.
The experiments showed that long chain-free fatty acids released by the creeping fat activate the muscle cells to proliferate and that blocking the uptake of these fatty acids into the mitochondria of the muscle cells in a mouse model reduced the muscle proliferation and the luminal narrowing. “These are potentially relevant findings,” says Dr. Rieder. “How fatty acids affect muscle proliferation is completely novel, and to show a direct functional link between creeping fat and the muscle has not been reported prior.”
Advertisement
Previously, Dr. Rieder’s team explored the formation of Crohn’s disease creeping fat, showing that it arises from the migration of preadipocytes in mesenteric fat and differentiation into adipocytes in response to fibronectin production by activated muscularis propria cells.
Currently, they’re investigating potential methods for blocking the muscle cells’ ability to process the creeping fat, possibly with a chemical compound. “In an ideal world, you might be able to prevent creeping fat from forming, but we don’t exactly know yet why it forms or when it happens, so that’s probably a long shot,” Dr. Rieder notes.
Interestingly, while creeping fat is unique to Crohn’s among bowel diseases, it is also found in atrial fibrillation, where the cardiac fat surrounds the atrium and there is also a direct muscle-fat connection. In fact, Rieder became involved in looking at the phenomenon through a joint grant with Cleveland Clinic cardiologist David R. Van Wagoner, who studies fat-muscle interactions in atrial fibrillation.
“It’s a translational interdisciplinary team that’s working on this. We have basic scientists, clinicians, pathologists and radiologists. This is discovery research. We’re making progress towards finding novel targets to help our patients.”
Advertisement
Advertisement

Study utilizes prospective data from the RISK cohort

Nationwide research underscores the importance of individualized treatment
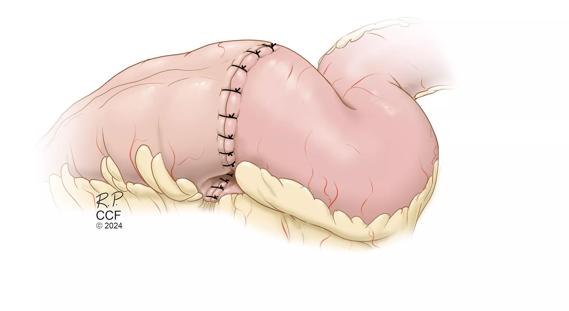
Findings support the safety of the technique

Strong patient communication can help clinicians choose the best treatment option
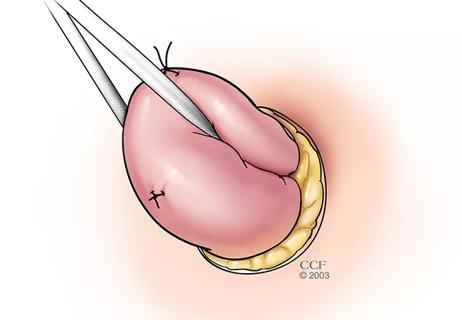
Findings from a 2023 ASCRS presentation indicate that both 2-stage and modified 2-stage approaches are viable management strategies for Crohn’s patients who require a temporary ileostomy

Retrospective analysis looks at data from more than 5000 patients across 40 years

The Integrated Program aligns IBD care and research across Cleveland Clinic locations

Diet has a profound impact on how the intestine functions