What geriatricians can do to stop it
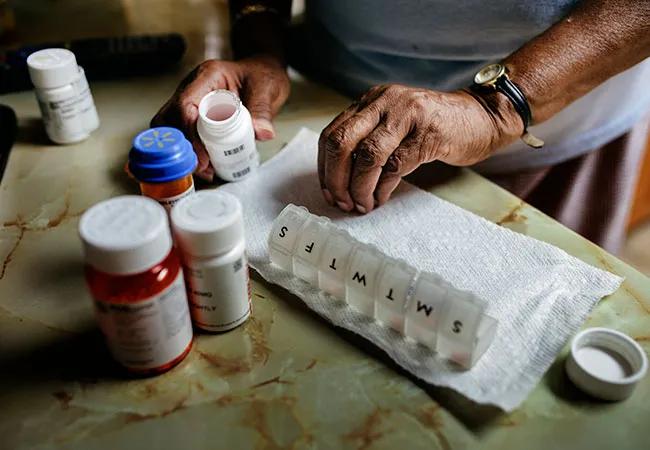
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5f79fff6-c046-42ba-bbe6-89c76db85523/Diabetes-Meds-1190823309)
Patient organizing medications
The abundance of pharmaceutical advertising has taught patients to beware of drug side effects. The Food and Drug Administration (FDA) requires drug manufacturers to disclose these risks alongside any potential benefits.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
But not for vitamin and herbal supplements.
The FDA considers them “foods,” not “drugs.” However, dietary supplements also can cause side effects and unwanted interactions with other substances.
This is a big concern for older adults with growing health issues, says Ronan Factora, MD, of Cleveland Clinic’s Center for Geriatric Medicine.
“The older population tends to take a lot of supplements by choice,” he says. “They could be lured by TV commercials or the advice of friends. And because they never hear a long list of potential side effects as they do with drugs, they assume there aren’t any.”
Compounding the problem, many supplements — which are easy to access, without a prescription — tout benefits that have little or no scientific evidence.
“Too much of some dietary supplements can be harmful,” says Dr. Factora. “Some can interact with prescription drugs or change how the body metabolizes them.”
He lists these examples:
Advertisement
“We need patients to know as much about taking their dietary supplements as they do about their prescription medications,” says Dr. Factora. “They should treat them the same.”
He recommends geriatricians do these three things:
It’s hard for physicians to keep up with the ever-expanding market of dietary supplements, Dr. Factora admits. That’s why he encourages patients to talk with a pharmacist.
“For people that want to take control of their health and boost their wellness with dietary supplements, it’s important to learn from a professional that best understands the properties,” he says.
Advertisement
Advertisement
New research highlights serious risks and the critical need for earlier advance care planning
Initiatives focus on the physical and emotional well-being of geriatric patients and their caregivers
Researchers explore the mental and physical benefits of social prescribing
Multidisciplinary approach helps address clinical and psychosocial challenges in geriatric care
Effective screening, advanced treatments can help preserve quality of life
Study suggests inconsistencies in the emergency department evaluation of geriatric patients
Auditory hallucinations lead to unusual diagnosis
How providers can help prevent and address this under-reported form of abuse