Nurse specialists evaluate patients, insert lines and provide training
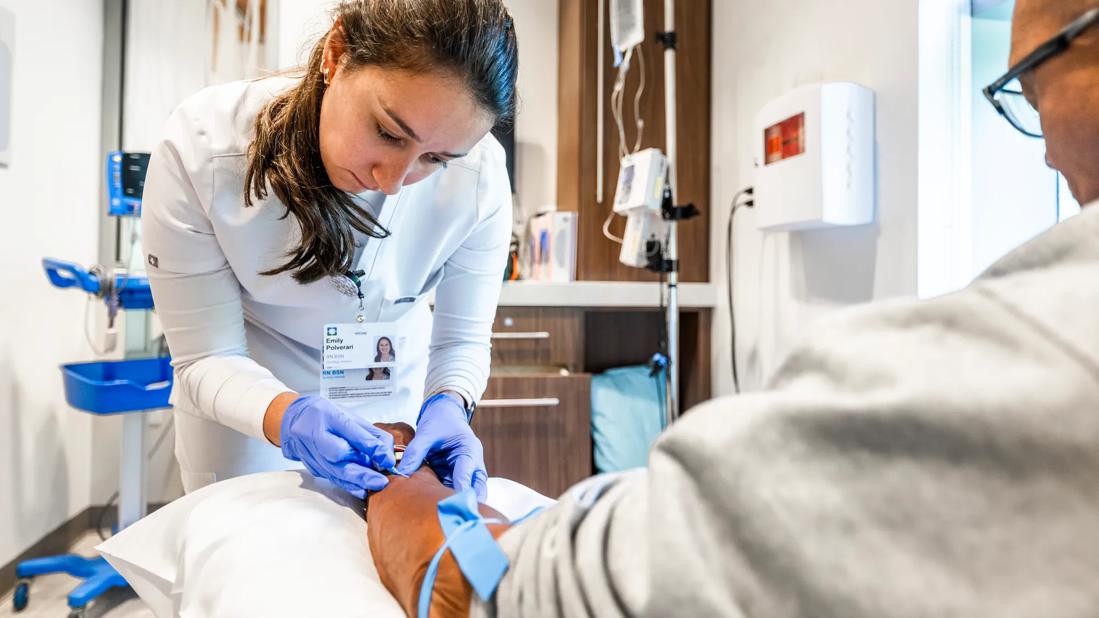
More than 2.7 million peripherally inserted central catheters (PICCs) are placed in acute care facilities in the United States each year, according to a report on the vascular-access devices market. While PICC lines offer many advantages, complications can occur, including infection and thrombosis. A dedicated team of nurses at Cleveland Clinic’s main campus helps prevent problems.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Patients go to a cardiologist when they have heart issues. Likewise, they should receive care from vascular-access specialists when they have vascular-access needs,” explains Shelly Altizer, MSN, RN, VA-BC, nurse manager of the Vascular-Access PICC Team at Cleveland Clinic.
The team includes 21 nurses who screen patients with orders for PICCs and midline catheters, insert the lines at the bedside and educate patients and nurses. Team members are also part of the Vascular-Access Affinity Group.
“We standardize best practices and ensure clinical excellence around vascular access through professional development and workforce education,” says Altizer, who chairs the group.
When a healthcare provider places an order for a PICC or midline catheter, a member of the PICC team initiates an extensive screening process.
“We thoroughly review the patient’s chart, including their medical and surgical history, before we go to the bedside,” says Altizer. They consider:
Advertisement
Once the screening process is complete, work at the bedside begins. The nurses assess the patient’s blood vessels, including the health and location of their veins. They also consider the catheter-to-vein ratio to minimize the risk for DVT.
“We don’t want to insert a catheter that takes up a large portion of the vein,” says Altizer.
After the vessel assessment, the nurses insert the PICC or midline. They also troubleshoot as needed. For example, they may help access ports or administer Cathflo®, which restores function to central venous access devices.
Bedside line placement has several advantages.
“Patients don’t have to wait for an interventional radiology room to become available, so you don’t have delays in patient care and treatment,” explains Altizer. “The team also sees outpatients, if needed, so they don’t have to cancel or reschedule appointments due to vascular-access needs. This is not only more convenient for patients, it can also help avoid unnecessary costs.”
When a nurse on the Vascular-Access PICC Team inserts a fresh line, they also seize the opportunity to remind clinical nurses about maintenance tasks, including dressing changes.
As an expert in vascular access, Altizer offers the following advice to clinical nurses:
Advertisement
“Our PICC team members have so much knowledge in vascular access and associated devices. They belong to professional organizations, receive board certifications and stay up to date on evidence-based practices,” says Altizer.
The metrics at main campus support the value of a dedicated team. In 2021, the Vascular Access PICC Team inserted thousands of central lines, with an associated blood infection rate of just 0.4%.
“Of course, we would love that number to be zero, but it shows that our rigorous infection prevention procedures, coupled with our first-time success rate inserting lines, reduces possible complications,” says Altizer. “And that increases patient satisfaction.”
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader