Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/7841c2d8-ef50-4b2b-9abe-19ea08a4425e/bariatric-surgery-outcome)
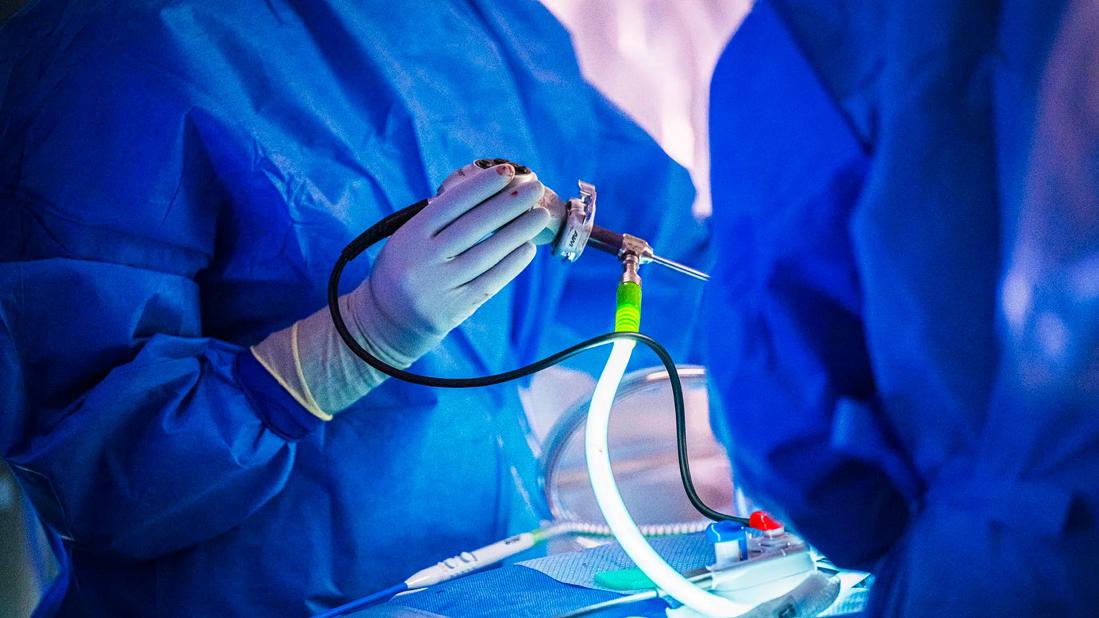
Bariatric surgery
Cleveland Clinic in Florida hosted the 21st Annual Surgery of the Foregut Symposium in February, bringing together a group of world-renowned surgeons, gastroenterologists and oncologists to share the latest in technological and therapeutic advances in foregut surgery.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The three-day South Florida event, which kicked-off with the 9th Congress of the International Society for Fluorescence Guided Surgery, drew an international attendance of physicians, surgeons, nurses, and allied health professionals.
According to Raul J. Rosenthal, MD, Regional Chairman of the Digestive Disease Institute for Cleveland Clinic in Florida and Activity Director for the symposium, sessions on robotics, complex bariatric surgery, and fluorescence imaging, in particular, generated a lot of interest and discussion this year.
The post-event educational outcomes assessment also found that more than 80% of surveyed attendees said they are likely or very likely to change their practice based on the information presented at the symposium.
“Many attendees shared they plan to expand their use of fluorescence-guided surgery, which is great news for patients who will benefit from safer surgery and enhanced outcomes,” says Dr. Rosenthal. He noted the first day of the symposium was dedicated to the inroads of fluorescence imaging in all facets of foregut surgery and beyond.
One of this year’s highlights was the Robert Hermann Memorial lecture entitled How to Successfully Manage Abdominal Wall Hernias in the Era of Robots and the Obesity Pandemic, presented by Michael Rosen, MD, Director of the Cleveland Clinic Center for Abdominal Core Health.
Dr. Rosen provided updates on the latest research concerning the management of patients with obesity who require ventral hernia repair and the open question of preoperative optimization. While obesity is known to be associated with an increased risk of surgical site infection (SSI) and surgical site occurrence requiring procedural interventions (SSOPI), it has been a challenge for surgeons to determine which patients would benefit from preoperative weight loss.
Advertisement
“As Dr. Rosen shared, there is still no clear evidence that preoperative weight loss interventions can reduce the impact of this association and more research is needed,” reports Dr. Rosenthal. “He also cautioned against the use of arbitrary cutoffs concerning patient BMI when determining eligibility for ventral hernia repair.”
Another area of great debate addressed by Dr. Rosen is the use of robotic-assisted surgery in abdominal wall reconstruction (AWR). “He has been on the frontline of this issue for a number of years and brought a great perspective,” says Dr. Rosenthal.
Dr. Rosen was principal investigator of the RIVAL trial, a multicenter, single-blinded, prospective randomized clinical pilot study that compared robotic inguinal hernia repair to laparoscopic repair. The study found no clinical benefit to the robotic approach though it incurred higher costs and more operative time compared with the laparoscopic approach.
“The robotic approach also demonstrated added surgeon frustration with no ergonomic benefit,” points out Dr. Rosenthal.
Likewise, the PROVE-IT randomized clinical trial, co-authored by Dr. Rosen, also found comparable 30-day clinical outcomes when comparing laparoscopic and robotic ventral hernia repair with intraperitoneal mesh, along with an increase in time and cost associated with the robotic approach.
Notably, however, a 1-year follow-up of the PROVE-IT trial looking at exploratory outcomes identified a potential quality-of-life benefit with the robotic approach and a potential reduced hernia recurrence risk with the laparoscopic approach, though no difference in rates of reoperation was observed.
Advertisement
“As Dr. Rosen summed up, while robotics are here to stay, we must be careful how we apply this technology and continue to look for the indications and contraindications that will impact patient outcomes,” says Dr. Rosenthal.
Another symposium highlight was the 10th Annual Walter Pories MD Lecture entitled Reoperative Bariatric Surgery: Understanding Revisions, Reversals and Conversions. It was delivered by Samuel Szomstein, MD, Associate Director of the Bariatric & Metabolic Institute and the Division of Minimally Invasive Surgery at Cleveland Clinic in Florida.
“My esteemed colleague took us on a deep dive into the world of reoperative bariatric surgery through the lens of our program in Weston, which is one of the largest bariatric programs in Florida,” says Dr. Rosenthal.
Approximately 280,000 bariatric surgeries, both primary and reoperative, were performed in the United States in 2022. Up to 25% of these patients may eventually require a secondary procedure, according to research cited by Dr. Szomstein.
Based on the Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP®) database for 2020-2021, weight gain, inadequate weight loss, and gastroesophageal reflux disease (GERD) are the most common indications for reoperations.
At Cleveland Clinic’s Bariatric & Metabolic Institute in Florida, 4,327 primary bariatric surgeries and 866 reoperations were performed between 2005 and 2022. Reoperations included 445 conversions, 401 revisions, and 20 reversals.
Advertisement
Here are some additional institute-specific statistics Dr. Szomstein shared, based on 2012-2022 data.
“Readmission, reintervention and reoperation are all more likely to occur with conversion and revision procedures than with primary surgeries,” notes Dr. Rosenthal. “These procedures can be highly complex and are best managed by high-volume centers. About two-thirds of our reoperations today are outside referrals.”
For more information, visit Cleveland Clinic Florida ConsultQD. Subscribe to the Florida Physician Newsletter. Additionally, follow us on X (formerly Twitter), Facebook, and LinkedIn.
Advertisement
Advertisement
Evidence shows early evaluation improves survival and quality of life – yet many eligible patients are referred too late
2026 ADA Standards of Care promote holistic, multisystem management
Cleveland Clinic nephrologist in Florida addresses changes in clinical practice
Surveillance platform supports community clinicians and public health monitoring
Benefits include improved clinical outcomes and lower healthcare costs
Pulmonary endarterectomy plays central role in era of multimodal therapy
Evidence supports safety and efficacy of surgery in patients aged 80 years and older
One in four experience reduced anxiety