Two stereotactic radiosurgery experts take stock after Cleveland Clinic’s 10,000th case
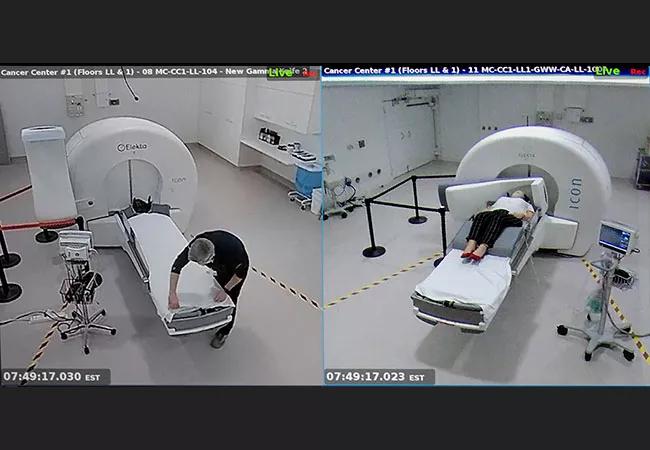
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/88b6d792-1bf4-41ad-b5da-5f232b8eb9c4/22-NEU-2763298-060-CQD-Hero-650x450-v2_jpg)
22-NEU-2763298-060-CQD-Hero-650×450-v2
When Cleveland Clinic treated its 10,000th patient with Gamma Knife® stereotactic radiosurgery early this year, clinicians in its Gamma Knife Center couldn’t help but think of the 10,000-hour rule from the Malcolm Gladwell book Outliers: The Story of Success.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Gladwell argues that the key to achieving true expertise in any skill is practicing for at least 10,000 hours,” says neurosurgeon Lilyana Angelov, MD, Director of the Cleveland Clinic Gamma Knife Center. “The analogy isn’t perfect, but it’s reasonable to consider 10,000 cases as a milestone signaling a distinctive level of expertise.”
That expertise was developed over 25 years of using several generations of Leksell Gamma Knife technology up through the acquisition of the latest model, the Icon™, in 2017 and a second Icon machine in early 2022. The two machines are located together on Cleveland Clinic’s main campus (see photo above), making it one of only two centers in the world with side-by-side Icon machines. “Having the machines side by side promotes a more seamless workflow, allowing us to treat more patients with the versatility that the Icon offers in terms of both frameless mask-based treatment and frame-based treatment,” Dr. Angelov notes.
The experience from those 25 years has also empowered Cleveland Clinic to train thousands of providers in the use of Gamma Knife technology as one of only five training sites worldwide authorized to teach Gamma Knife therapy. It has likewise yielded more than a few lessons in the optimal use of stereotactic radiosurgery. Consult QD recently caught up with Dr. Angelov and her colleague Samuel Chao, MD, a radiation oncologist and Associate Director of the Gamma Knife Center, to distill some of those lessons and update neuro-oncology providers on the technology’s current and emerging capabilities. Their responses to five key questions are shared below.
Advertisement
Brain metastases remain the predominant application of Gamma Knife at Cleveland Clinic, representing about 80% of Gamma Knife Center cases. “Gamma Knife treatment has a very high oncological impact in metastatic disease, with local control rates of 85% to 90%,” says Dr. Angelov. “Few treatments in oncology can boast control rates that high.”
Brain metastases are well controlled by stereotactic radiosurgery because metastatic cancer cells tend to be walled off by the brain, making them vulnerable to the precision targeting of Gamma Knife therapy. In contrast, primary brain tumors involve cancer cells that do not get walled off in the same way, rendering these tumors far less appropriate for Gamma Knife therapy. “Primary brain tumors are not a large part of our Gamma Knife practice,” Dr. Angelov explains. “We tend to limit stereotactic radiosurgery to recurrence of primary tumors, which often involves a focal area that’s more amenable to precision targeting.”
Another key application is benign brain tumors, including meningiomas, acoustic neuromas and pituitary adenomas. These have been treated with stereotactic radiosurgery for decades with high rates of success and low rates of recurrence. Gamma Knife also has a role in the management of several non-tumor conditions, including trigeminal neuralgia, arteriovenous malformations (particularly when difficult to reach surgically), and essential tremor and other movement disorders.
“The Icon machine has expanded the number of lesions we can treat in a given setting,” notes Dr. Chao. That’s because of its ability to accommodate both traditional minimally invasive frame-based patient immobilization and the newer mask-based noninvasive immobilization (see photo below) with real-time tracking for alignment. The introduction of mask immobilization has provided the option of fractionated and multisession radiosurgery, which involves distributing the radiation dose over several (typically five) consecutive days to allow treatment of large numbers of lesions or safer, yet precise treatment of lesions close to sensitive structures like the optic nerve. Multisession dosing is far more feasible with use of a noninvasive mask than a frame that needs to be repeatedly affixed and removed from the skull.
Advertisement
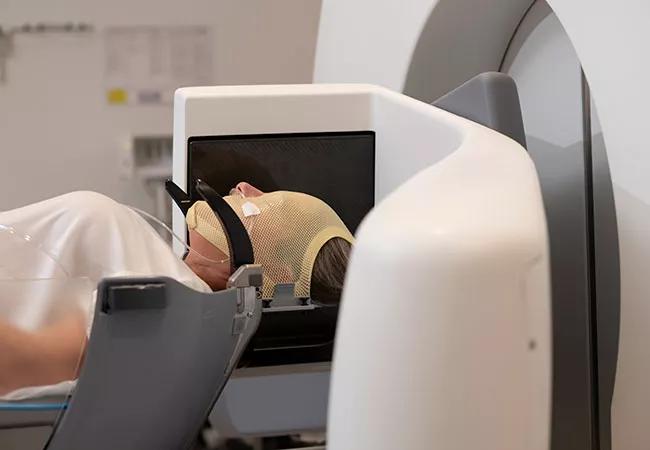
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/6ccc64c4-01c7-4cd2-8e0b-1dde39207d2c/22-NEU-2763298-050-inset_jpg)
Photo showing the mask-based immobilization possible with the Gamma Knife Icon machine.
“In the past, it would be a stretch to treat much more than five lesions in a patient with brain metastases, as the patient would need to be docked in a frame for hours, which could be quite uncomfortable,” Dr. Chao explains. “Now with the mask we can consider treating as many as 20 lesions over the course of several days.”
He adds that fractionated radiosurgery also allows treatment of larger lesions and lesions in challenging locations, particularly in cases of benign tumors. For example, fractionated radiosurgery is now used to treat large meningiomas over five days, as opposed to the six weeks required with conventional radiation therapy. Moreover, in cases such as a pituitary adenoma which is in a precarious spot underneath the optic nerve and chiasm, fractionated therapy can sometimes be used to deliver smaller radiation doses over time, which is safer to those structures when the tumor is too close. “Our enhanced ability to fractionate has led to more opportunities to use Gamma Knife than even a few years ago,” Dr. Chao says.
Dr. Angelov notes that she and her Cleveland Clinic colleagues use Gamma Knife almost exclusively for brain radiosurgery. “We favor Gamma Knife for brain applications because we believe it offers superiority in precision targeting, with accuracy of 0.1 mm, as well as in dosimetry and dose fall-off,” she says. “This allows for better local control while keeping the dose to surrounding normal brain tissue extremely low.”
Advertisement
She adds that another enhancement with the Icon machine is the integration of high-resolution onboard cone-beam CT to enable true stereotactic imaging to correct positioning at the time of treatment.
Both physicians say it has expanded to be applicable to more patients and more situations. This is due in part to the advancements in the technology and in fractionation capabilities noted above. “We are comfortable treating more lesions in a single patient and treating lesions that are larger, more complicated and in difficult locations,” says Dr. Chao. “Some physicians are not aware that sometimes radiosurgery alone (without additional surgery) can now be effective treatment for even large brain metastases.”
The technology’s expanded role is also a testament to the success of targeted systemic therapies for cancers below the neck, notes Dr. Angelov. “Patients with metastatic disease are living much longer, so the intermediate-term consequences of their treatment for brain metastases, such as not irradiating local normal brain tissue, matter more than ever,” she says. “That enhances the value of Gamma Knife therapy, especially relative to approaches such as whole brain radiation therapy.”
In fact, Dr. Chao notes that advancements in systemic therapies may ultimately reshape the role of Gamma Knife in treating metastatic disease. “Systemic therapies and their role in the multimodality management of brain metastasis are being studied, including here at Cleveland Clinic,” he says.
Beyond the recent growth in fractionated radiosurgery noted above, Cleveland Clinic is involved in a number of innovative uses of Gamma Knife technology.
Advertisement
One is staged radiosurgery based on tumor volume, a technique for large brain metastases developed in Japan and introduced in the U.S. a few years ago by Dr. Angelov at Cleveland Clinic. Designed to address the challenges of large lesions, the technique involves giving doses in two discrete treatment sessions with the aim of shrinking the tumor with the first dose and then shrinking it further with the second dose. The goal is to allow an increased overall dose to improve local tumor control while administering smaller individual doses to reduce toxicity.
“Staged radiosurgery tends to give us 88% to 90% local control for large lesions as compared with 50% control using single-session treatment,” says Dr. Angelov. She adds that the staged approach is now gaining traction among radiation oncologists for treatment of tumors in other organs as well.
Cleveland Clinic also is among a number of centers increasingly using resection cavity radiosurgery for appropriate patients. This technique is used postoperatively for patients requiring resection for metastatic disease in an effort to avoid whole brain radiation.
Likewise, Cleveland Clinic is helping to pioneer neoadjuvant radiosurgery for metastatic disease, in which Gamma Knife is applied to a large target mass prior to resection in the hope of killing off cancer cells at the outset, prior to surgical perturbation. The aim is to sterilize the tumor field and avoid the need for postsurgical radiation therapy. “We believe it reduces the risk of seeding, or leptomeningeal spread, and it may also reduce the risk of radiation necrosis,” Dr. Chao explains. Cleveland Clinic is leading a dose-escalation study of this approach.
Additionally, Cleveland Clinic is part of a number of collaborative investigations of radiosurgery, including studies of multimodality therapy combining radiosurgery with immunotherapy to get even higher control rates in metastatic disease.
Cleveland Clinic’s Rose Ella Burkhardt Brain Tumor and Neuro-Oncology Center is structured to promote multidisciplinary evaluation and consultation for all patients who need it. While brain metastasis cases are often straightforward enough to not require discussion at the center’s brain tumor board meetings, other radiosurgery cases more frequently do. “More complicated cases, such as recurrent gliomas and some meningiomas, are presented at tumor board because we need to explore questions that demand a multidisciplinary answer, such as whether to proceed with radiosurgery or how to time it relative to surgery,” says Dr. Chao. In those cases, neurosurgeons, neuroradiologists, medical oncologists, radiation oncologists and others weigh in.
The brain tumor board also comes into play in the uncommon instance that radiation necrosis develops after radiosurgery. “Our tumor board has a robust program for evaluating and managing radiation necrosis, which may include several medical management options or even minimally invasive surgical options such as laser interstitial thermal therapy (LITT),” says Dr. Angelov. “This is part of the linear continuity of care that we offer to all patients after Gamma Knife therapy.”
She and her Gamma Knife Center colleagues see patients two months after their radiosurgery and every three months thereafter. “We like to maintain ongoing follow-up to address the nuances of these patients’ needs,” Dr. Angelov notes. “But we do this in cooperation and collaboration with their referring provider. When a patient is referred for brain tumor evaluation, we will consider every tool in our tool belt. When radiosurgery is appropriate, referring physicians can be assured that we will be using the most precise radiosurgery option available and applying insights from one of the most extensive Gamma Knife experience bases in the nation. When treatment is completed, patients return to the care of their referring provider but are always encouraged to also continue coordinated follow-up of their brain disease here to monitor and tend to any radiosurgery-specific needs.”
Advertisement
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation
Best practices for supporting patients with honesty and compassion
Goal-of-care discussions drive earlier hospice access
Clinical trials and de-escalation strategies
Combination therapy improves outcomes, but lobular patients still do worse overall than ductal counterparts
Bringing empathy and evidence-based practice to addiction medicine
Supplemental screening for dense breasts