Why leadership training for physicians is crucial to successful healthcare

Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The healthcare landscape is shifting at a rapid pace. These changes require collaborative engagement from physicians in every specialty in order to deliver safe, effective, efficient and reliable healthcare. However, traditional medical education fails to create truly collaborative leaders, while team-based care is proven to improve patient outcomes. Understanding health and disease remains the backbone of medical school and graduate training, while the nuanced teamwork and communication tools for successful doctoring are relegated to the hidden curriculum.
How can physician leaders bridge the gap in healthcare providers’ training? Cleveland Clinic’s Global Executive Education (GEE) programs are effectively formalizing physician leadership education based on our own successful Leading in Healthcare (LHC) course.
Leadership competencies differ from clinical skills and are traditionally taught neither in medical school nor in graduate medical education. Indeed, as I have noted in previous publications, physicians have been historically trained as “heroic lone healers” and hence may be “collaboratively challenged.”1 However, approximately 98,000 hospital patients die annually from preventable medical errors, and nearly one-third of patients are adversely affected by preventable errors during admissions. What’s more, improved collaboration benefits a myriad of clinical outcomes, including perioperative and intensive care unit mortality.
As more and more physicians take on administrative or leadership roles within the healthcare arena, there is an additional need to enhance the collaborative, team-based model of healthcare delivery. Indeed, a study published in 2011 examined CEOs in the top-100 best hospitals in U.S. News & World Report in three key medical specialties: cancer, digestive disorders and cardiovascular care. A simple question was asked: Are hospitals ranked more highly when they are led by medically trained doctors or non-MD professional managers? The analysis showed that hospital quality scores are approximately 25 percent higher in physician-run hospitals than in manager-run hospitals. Yet, most physician leaders are not formally taught leadership or team-management strategies; instead, these skills are learned on the job.
Advertisement
What if we did a better job of formally teaching our emerging leaders how to be the stewards of collaborative healthcare teams? A case study of Cleveland Clinic’s LHC program reveals how we effectively filled that void to create successful leadership teams: Action learning projects provide participants with multidisciplinary experiential learning opportunities through which they produce tangible benefit to the institution.
Formal leadership training, although deemed to positively impact the individualized clinical care as well as the hospital system at large, is still generally an organic process. However, since 1990, Cleveland Clinic has trained over 500 Cleveland Clinic caregivers — physicians, nurses and administrators — in its LHC program. LHC invites nominated, high-potential caregivers to engage in ten days of offsite training in leadership competencies which fall outside the domain of traditional medical training. Core to the curriculum is emotional intelligence (with 360-degree feedback and executive coaching), team-building, conflict resolution and situational leadership.
The course culminates in a team-based innovation project presented to hospital leadership. Sixty-one percent of the proposed innovation projects have had a positive institutional impact. Furthermore, in ten years of follow-up after the initial course, 43 percent of the physician participants have been promoted to leadership positions at Cleveland Clinic.
The growth of leadership training programs reflects the growing need for physicians to develop and nurture leadership competency. More importantly, a focus on leadership development reflects an appetite amongst physicians to become drivers of healthcare improvement. Cleveland Clinic’s Global Executive Education suite of executive leadership programming shares the best practices in healthcare leadership through a proven method of experiential training. We provide physicians not only with collaborative skills to take back to their own institutions, but participants also have the opportunity to join a powerful, international network of thought leaders and healthcare executives.
Advertisement
Physicians seek mastery of science, procedural skills, anatomy and physiology from the day they step foot in organic chemistry. Mastering team-based leadership skills through programs like LHC will give physicians the tools to successfully guide medicine through the decades of change that lie ahead.
Dr. Stoller is a practicing pulmonologist, Chair of the Education Institute and holds the Jean Wall Bennett Professorship in Emphysema Research at the Cleveland Clinic Lerner College of Medicine and the Samson Global Leadership Academy Endowed Chair.
References:
Advertisement
Advertisement

Advanced software streamlines charting, supports deeper patient connections

How holding simulations in clinical settings can improve workflow and identify latent operational threats

Interactive Zen Quest experience helps promote relaxing behaviors

Cleveland Clinic and IBM leaders share insights, concerns, optimism about impacts
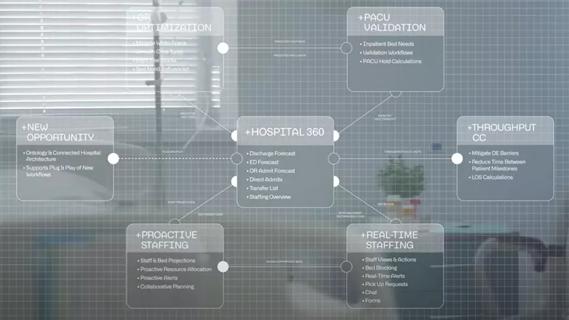
Cleveland Clinic partners with Palantir to create logistical command center

A Q&A with organizational development researcher Gina Thoebes

Cleveland Clinic transformation leader led development of benchmarking tool with NAHQ

Raed Dweik, MD, on change management and the importance of communication