New innovations improve treatment of this rare disease
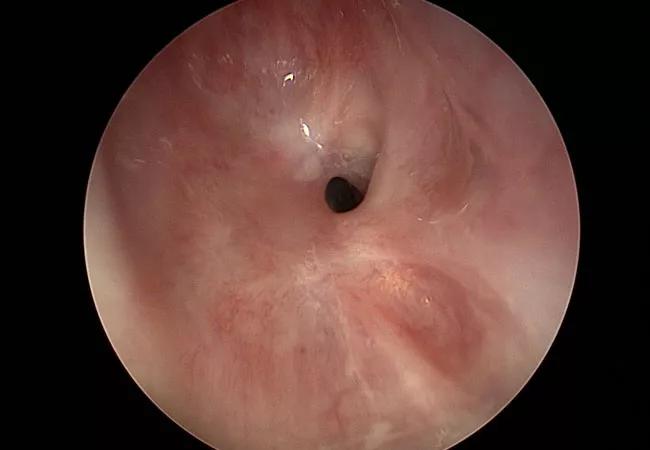
Subglottic stenosis is a narrowing of the larynx below the vocal cords, essentially blocking a patient’s airway. It can be caused by trauma (including from tracheotomy or intubation) or autoimmune disease (including granulomatosis with polyangiitis, sarcoidosis and systemic lupus erythematosus). However, in some cases, the condition is idiopathic.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“The standard delay in diagnosis for a patient with idiopathic subglottic stenosis (iSGS) is one to two years,” says Robert Lorenz, MD, a surgeon in the Head and Neck Institute at Cleveland Clinic. “The condition is often misdiagnosed because the etiology is uncertain and the symptoms — including stridor, coughing and breathlessness — are nonspecific. Up to a third of patients are initially diagnosed with asthma.”
Patients with iSGS commonly use bronchodilators for months or years with no improvement, he adds. When symptoms aren’t successfully managed by asthma treatment, it’s time to change course and consider this rare disease.
While diagnosing iSGS can be challenging, treatments for the condition have advanced in recent years, as reviewed in this Journal of Thoracic Disease article co-authored by Dr. Lorenz.1
Incidence of iSGS is low, about 1 in 400,000 people. But 99% of those diagnosed are female, predominantly white women between ages 20 and 50.
“There are a number of ongoing studies, mostly coming out of the North American Airway Collaborative, on why the disease largely affects patients who are white, fertile and female,” says Dr. Lorenz. “The cause likely will have a hormonal aspect, but that’s yet to be defined.”
For now, iSGS is a diagnosis of exclusion, he says. Patients are evaluated for history of trauma to the larynx. If symptoms began within three to six months of having a breathing tube, for example, traumatic etiology may be suspected.
Diagnosing autoimmune etiology involves detecting other hallmarks of autoimmune disease, such as sinusitis and ear problems, as well as suggestive lab results. Treating this type of subglottic stenosis is centered on treating the root autoimmune disorder.
Advertisement
For idiopathic (and some traumatic) subglottic stenosis, treatment often begins conservatively, with an endoscopic procedure.
“Our goal is to do as little intervention as possible, especially if the patient is only minimally stenotic and has no breathing problems,” says Dr. Lorenz
If patients are symptomatic, standard treatment consists of:
The procedure can be repeated as needed. For most patients, one treatment controls symptoms for one year or longer.
For refractory conditions or for patients who don’t tolerate the endoscopic dilation well, the second line of treatment is serial steroid injections. For this procedure, the standard steroid injection, lysis and dilation is performed, followed by monthly steroid injections for three consecutive months. Injections can be done during an office visit or, if the patient prefers, under general anesthesia in an operating room.
The third line of treatment is the Maddern procedure, developed over the last decade. Introduced in the U.K., this transoral procedure entails shaving away the fibrotic tissue in the larynx and relining the area with tissue grafted from the thigh. Dr. Lorenz, who has performed nearly 30 Maddern procedures — the most in the world — recently revised the procedure to use lining from the cheek rather than the thigh.
Advertisement
“Cells from the cheek are optimal because they don’t contain keratin, which can slough off, collect in the airway and cause blockage or irritation,” says Dr. Lorenz.
The grafted lining adheres with the help of a silicone stent, which is removed after two weeks.
Patients with more complex lesions affecting cartilage require conventional surgical treatment, such as cricotracheal resection. This invasive procedure, while effective at treating iSGS, involves removing the muscle that allows vocal inflection.
Dr. Lorenz most recently introduced a modified procedure, extended tracheal resection, which entails removing the stenotic lining inside the voice box while preserving the muscle that attaches to the cartilage structure, thereby retaining vocal pitch. In an open procedure through the neck, the diseased uppermost portion of the trachea is removed along with lining of the lower larynx. Healthy tracheal tissue is used to reline the subglottic area.
“As we unravel more about the pathophysiology of iSGS, we will continue to discover more advanced ways of treating it,” says Dr. Lorenz. “There are new discoveries and trends in treatment all the time, which makes it even more important to diagnose patients with iSGS as promptly as possible.”
References
1. Aravena C, Almeida FA, Mukhopadhyay S, Ghosh S, Lorenz RR, Murthy SC, Mehta AC. Idiopathic subglotic stenosis: A review. J. Thorac. Dis. 2020.; 12(3):1100-1111.
Advertisement
Advertisement

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP

Patient with cerebral palsy undergoes life-saving tumor resection

Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition

Detailed surgical process uncovers extensive middle ear damage causing severe pain and pressure.