Gene signatures differentiate clinical response
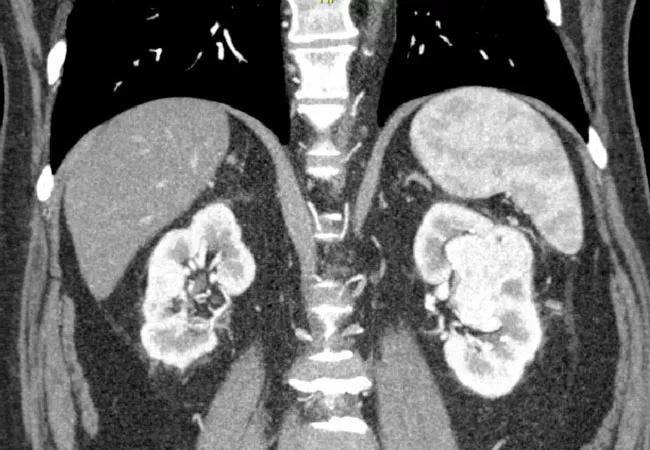
Advances in immunologic drugs are changing treatment options for patients with metastatic renal cell carcinoma (mRCC). Combinations of monoclonal antibodies against PD-1 or PD-L1 and VEGF inhibitors are showing promising results, compared with single-agent monoclonal antibodies.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In June, results of the phase 3 study IMmotion151 indicated that patients with untreated mRCC fared better with a combined regimen of atezolizumab (a PD-L1 monoclonal antibody) and bevacizumab (an anti-VEGF monoclonal antibody) than those that took only anti-VEGF drug sunitinib. Progression-free survival (PFS) in the atezolizumab/bevacizumab group was 11.2 months compared with 7.7 months in the sunitinib group. The time to deterioration (TTD) in interference was 11.3 months in the combination therapy group compared with 4.3 months for sunitinib. In addition, compared to patients taking sunitinib, more patients taking the combination therapy reported little or no difficulty from treatment side effects.
While these results were clinically significant, researchers sought to understand the molecular signatures supporting them. That led to a supplementary study, analyzing the genomics of tumors treated in IMmotion151.
The study’s lead investigator, Brian Rini, MD, Professor of Medicine at Cleveland Clinic Lerner College of Medicine and Leader of the Genitourinary Program at Cleveland Clinic Cancer Center, presented these supplemental findings at the 2018 European Society for Medical Oncology (ESMO) Annual Meeting in Munich, Germany.
“Understanding molecular signatures is important because too often our approach is empiric. We give a medicine, and then wait to see if it works,” says Dr. Rini. “These data give us biologic insight into renal cell carcinoma to enhance our ability to choose the correct therapy.”
Advertisement
Biomarker analyses in the phase 2 IMmotion150 study suggested that T effector (Teff) and interferon gamma gene expression signatures (GEs) were associated with different outcomes in treatment groups. So were angiogenesis GEs.
As such, researchers conducted genomic analyses to validate these GEs with clinical outcomes in IMmotion151. They also correlated the GEs with Memorial Sloan Kettering Cancer Center (MSKCC) risk groups and sarcomatoid histology.
They found:
These results validate the molecular signatures that differentiate clinical outcomes with combined PD-L1 and anti-VEGF monoclonal antibodies. They also identify tumor genomic profiles associated with prognostic risk groups and sarcomatoid histology.
“Findings from this study help us better understand the biology of kidney cancer,” says Dr. Rini. “They also will inform future strategies to enable personalized therapy in mRCC patients.”
Advertisement
Advertisement

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors

Study shows significantly reduced risk of mortality and disease complications in patients receiving GLP-1 agonists

Structured interventions enhance sleep, safety and caregiver resiliency in high-acuity units

Addressing rare disease and challenging treatment course in an active young patient