As intervention and surgical techniques improve, facial reanimation patients can achieve a more natural look
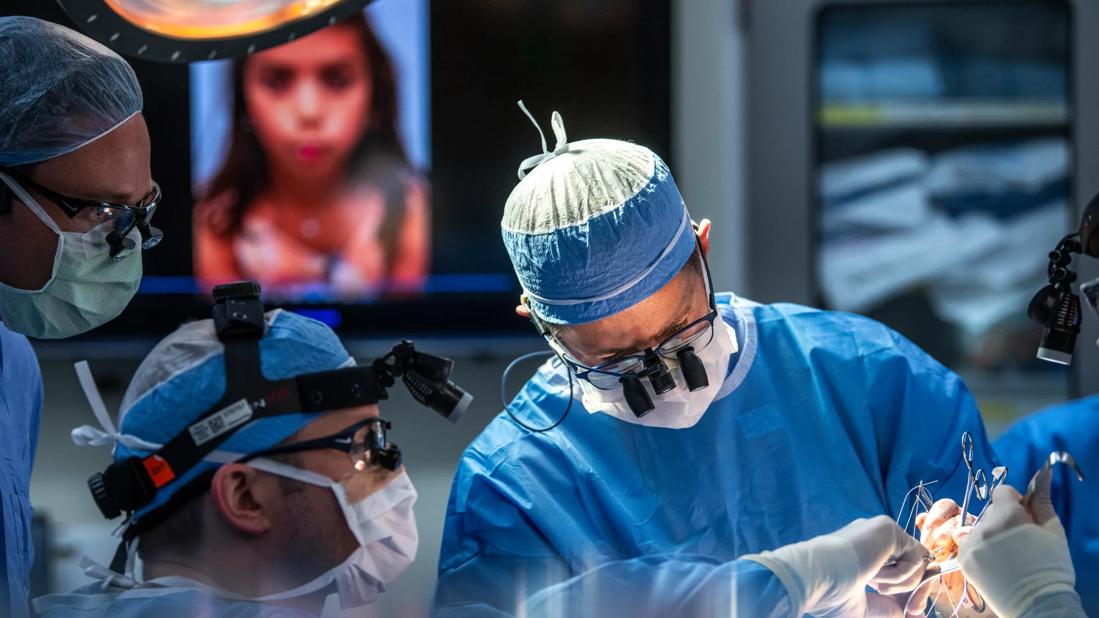
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/69603611-5eca-4061-9dde-ecb8b5c86bfc/CCC_2191938_06-08-21_349_AMO)
Byrne, md
Throughout his career in medicine, Patrick Byrne, MD, MBA, the Chairman of Cleveland Clinic’s Head & Neck Institute has framed his work around a specific goal. Specializing in facial reanimation, he has diligently pursued how to restore natural-looking smiles and facial expressions in patients who are born with congenital facial paralysis or developmental facial paralysis. “A lot of the various innovations and procedures I’ve done has really largely been in pursuit of that objective,” says Dr. Byrne. “When I started my career, I was impressed with the options we had for facial reanimation. But the progress we’ve made over the past 10 years or so is profound.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
There are a few significant milestones that have changed the trajectory of facial paralysis care, according to Dr. Byrne. One of these is the change in approach to timing. “In certain situations, we don’t wait as long as we used to re-innervate facial nerves,” says Dr. Byrne. “We’ve learned to intervene more quickly during the re-innervation window. We used to wait a year, for example, after an acoustic neuroma resection that resulted in facial paralysis. Now we’ll wait at most six months.”
Just as physicians don’t wait as long to re-innervate, patients have more options available to them and are coming in sooner for consultation. This means that for patients with adult or later-onset facial paralysis, there is a higher chance that Dr. Byrne and his team can still reanimate nerves. “Now, we see these patients within a year and we’re able to help them. We can go in and wake up their facial muscles by rerouting other nerves.”
Both within the re-innervation window (during the first year after the onset of complete facial paralysis) and beyond into the longstanding duration paralysis cases, there has been a great deal of innovation over the past decade. Dr. Byrne believes surgeons have far more nuanced and a greater number of re-innervation options. “The facial nerve is cranial nerve #7. My focus is on patients with facial nerve injuries, and congenital facial nerve anomalies. We used to do a rather blunt technique called hypoglossal-facial nerve transfer. We would take the 12th nerve, that powers tongue movement, and connect it end-to-end to the damaged facial nerve. This technique works, but patients would move their tongue a little bit and their whole face goes awry. It was just too much mass movement.”
From the hypoglossal-facial nerves transfer, the techniques evolved to performing multiple cranial nerve transfers. “Today, we will often perform partial connections to the 12th cranial nerve (thus preserving tongue function while limiting mass movement), then separate the zones of the face control by also performing a direct nerve transfer of the buccal branch of the facial nerve (which helps generate the smile) to a branch of the 5th cranial nerve (which powers chewing). This allows the patient to learn how to power different areas of the face with different nerves, taking advantage of the varying properties of these donor nerves. We will also do a cross-face nerve graft, or two of them to the other side, in which we connect via long cable grafts to the “normal” facial nerve branches on the opposite side of the face in order to allow spontaneous movement,” explains Dr. Byrne. “The triple re-innervation strategy provides patients with a much more nuanced, subtle and natural appearance than the single re-innervation.”
Advertisement
For patients who have suffered from facial paralysis for many years, it may be too late to awaken their own native facial muscles. Congenital facial paralysis patients often lack the muscles of expression. In these cases, an expanded array of options has become available over the past few years. Among these are the Temporalis Tendon Transfer, or T3. The temporalis can be accessed through a skin fold between the lip and the cheek. The tendon and bone are redirected, attached to muscles at the corner of the mouth, which results in the corner of the mouth being pulled upwards in a more symmetric way. Because this is a fairly simple technique to learn to do, centers that don’t have access to sophisticated microvascular surgery can still offer a suitable option to their patients.
The most advanced techniques involve microsurgical free tissue transfer, in which muscle is transplanted from one area of the body to another while connecting multiple microscopic nerves and blood vessels. “In the past five years or so, the advancements are more focused on the artistry of the technique for microvascular free tissue transfer,” says Dr. Byrne. “We’ve moved away from large gracilis muscle in a single vector connected to a cross face nerve graft. Now we do smaller muscles separated and split into multiple little strips to recreate multiple different vectors of movement. These are fed by several different nerve sources. We’re achieving progressively more natural results, more consistent results and more predictable results. At Cleveland Clinic, we’re really focused on correlating the fine details of the cases, to the results we track, so we can continuously improve our craft.”
Advertisement
For Dr. Byrne, it is the culture within the Cleveland Clinic’s Head & Neck Institute, and specifically the group of facial reconstruction surgeons, which he believes help to differentiate it from other healthcare centers. “I am very fortunate to join three incredibly talented surgeons with an enormous wealth of experience and training, which importantly is highly specialized and laser-focused on cosmetic and reconstructive surgery of the face, head, and neck,” says Dr. Byrne. “I don’t think there’s any place, certainly in North America, which has four very well-trained, experienced facial plastic surgeons of this caliber with skills specific to the entire gamut of facial reanimation. Besides myself, Michael Fritz, MD, the Director of the Section of Facial Plastic and Microvascular Surgery, has over 20 years of experience in this field and is widely viewed as one of the very best microvascular surgeons in the world. In recent years, he has methodically created a really incredible team. Dane Genther, MD, and Peter Ciolek, MD, were each lured to the Head and Neck Institute from the top programs in the nation, where they were trained in all of the cutting edge techniques – not only in facial reconstruction but also in the very focused area of facial cosmetic surgery and treatments. The extensiveness of training and approaches is very beneficial. We are all extremely collaborative; we want to do cases together and we’ve made that a commitment. There is no competition between surgeons here – only a desire to push forward the field with world-class work. Cleveland Clinic is a place where this is encouraged.”
Advertisement
For Dr. Byrne, these advancements have helped him and the other facial plastic surgeons at Cleveland Clinic get that much closer in their pursuit of creating a natural smile. “I sort of obsess on seeing how people smile and how we can create that effect in our patients with facial paralysis. A person’s smile is such an important part of their character. Our smile helps us express ourselves and connect with others. Being able to give this ability back to someone who has lost it, or has never had it, is why I love this work so much. I hope the developments in this field that we’ve seen over the past few years are a sign that even more progress is on the way,” says Dr. Byrne.
Advertisement
Advertisement
Systematic review indicates more can be done for higher-risk patients
Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor
Case study illustrates the potential of a dual-subspecialist approach
Evidence-based recommendations for balancing cancer control with quality of life
Study shows no negative impact for individuals with better contralateral ear performance
HNS device offers new solution for those struggling with CPAP
Patient with cerebral palsy undergoes life-saving tumor resection
Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition